Stress and heart disease
I have drifted around the issue of stress and cardiovascular disease (CVD) for some time. For many years I pursued the idea that stress was the cause of CVD. Indeed, I had it all worked out, fitting all facts about CVD within this model. But…
I was at a conference in Saudi Arabia a few years ago, giving my ‘How stress causes CVD’ lectures, to great acclaim, or so I thought. However, Paul Rosch, who was also attending said to me, one evening at dinner. ‘It is all very well to show that stress is associated with heart disease, but you have not really established a mechanism.’
This, I realised, was true. I could show things such as the fact that severe depression can cause insulin resistance, even type II diabetes. Also, that depression is associated with a much higher rate of CVD, as are almost all metal health diseases. On average, someone with a mental illness can expect to die around twenty years earlier than those in the surrounding population.
I could show that psychosocial stress lead to Hypothalamic Pituitary Adrenal-axis [HPA-axis] dysfunction, which then drove the metabolic syndrome, with a much higher rate of CVD. The HPA-axis is the conductor of the entire ‘stress’ system.
At one stage I became very interested in spinal cord injury, and CVD. I discover that, the level the spinal cord injury occurred, made very significant differences to the rate of CVD. This, in turn, seemed almost entirely dependent on whether the autonomic nervous system was spared, or damaged.
The autonomic sympathetic/parasympathetic nervous system co-ordinates the ‘flight or fight’, stress, response. It runs down the spinal column before fanning out to link up to all of the organs in the body. You have little conscious control over it, which is why it is often called the ‘unconscious’ nervous system.
The sympathetic part of the autonomic system does such things as, speeding up the heart rate, constricting the bladder, redirecting blood to the muscles. Also stimulating the release of stress hormones, such as cortisol, to increase blood clotting and raise blood sugar levels – all good things in preparation for a fight.
I figured, along with many others, that if the fight or flight response was chronically activated, this would have severe and potentially damaging effects on the body. A chronic ‘dysfunctional stress response’ if you like. It appeared that much of the damage caused by a dysfunctional stress response centred around the stress hormone cortisol.
This idea was further strengthened by the looking at Cushing’s disease, a condition whereby the adrenal glands produce too much cortisol – for various reasons. People with Cushing’s disease have a spectrum of biochemical and physiological abnormalities, from raised blood pressure to severe insulin resistance, raised blood clotting factors, and suchlike.
Those with Cushing’s almost always develop the metabolic syndrome, and often frank type II diabetes. They have a vastly increased risk of dying of CVD. Around 600% (relative increase in risk). Last week I was sent a paper, looking at Cushing’s, called ‘Markers of atherosclerosis in patients with Cushing’s syndrome: a meta-analysis of literature studies.’
The authors found: ‘Cushing’s disease is associated with an increased intima-media thickness (IMT), higher prevalence of carotid plaques, and lower flow-mediated dilation as compared with controls. These data consistently suggest the need for a strict monitoring of early signs of subclinical atherosclerosis in Cushing’s patients.’1
In fact, the prevalence of atherosclerotic plaques was 988% higher (relative risk), than in controls. This is, basically, a ten-fold increase in the risk of plaques, and that moves Cushing’s Disease from association to causation.
I have also looked at people who used steroids for various medical conditions and found that they had a greatly increased risk of CVD. It is estimated that regular steroids use increases CVD risk by around 400% (relative increase in risk). For those who do not know, steroids are often called corticosteroids, because they all used cortisol as the building block. [Cortisol is also called a ‘steroid’ hormone].
CORTISOL
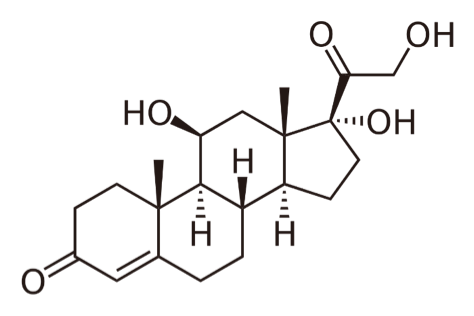
PREDNISOLONE – A commonly prescribed ‘steroid’
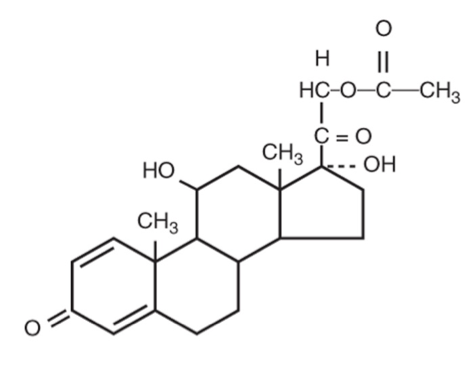
Whilst everything was, of course, rather more complex that this, with far more strands of evidence to gather together. I had worked my way towards a pretty clear causal chain that looked something like this:
Negative psychological and/or physical stress → HPA-axis dysfunction → abnormal cortisol secretion → metabolic syndrome/type II diabetes → atherosclerosis → increased risk of CVD
Now, I think that this model is still perfectly usable, and it explains a lot. However, although I drew a simple arrow from metabolic syndrome/type II diabetes → atherosclerosis, this is the bit that Paul Rosch was talking about. What is actually happening here? It is all very well to state that something causes something else, but you still need to explain how.
I realised that I did not know how, other than in general terms. I also realised that there were many other things that ‘cause’ CVD, that are not stress related e.g. smoking, omeprazole, Kawasaki’s disease, air pollution, Avastin etc. etc. How could all these be fitted into that one small arrow. That is when I ripped up the stress hypothesis, to start again. Pretty painful, but necessary.

Thank you
“Bugger me ! A doctor who doesn’t know !”
I have written this and it may seem to be ‘sarcastic’. But in fact I am pleased and grateful to read this post. Admitting that you do not know, that you need to think it through again is wonderful and rare. Humility is rare. Thank you.
I look forward to reading more as others make contributions via comments and as you sift through the evidence.
interesting stuff
and good for you exposing the many steps on the route!
Thank you. Interestingly you mention smoking, which is associated with raised cortisol too. eg this study “Smoking cessation was accompanied by an abrupt decrease in salivary cortisol, and this was sustained over the abstinence period.” http://www.sciencedirect.com/science/article/pii/S0167876005002679
Yes, I have wondered about this in the past. I think it can explain some, but not all of the effect of smoking
Good day all.
This is interesting, I am prescribed Omeprazole although I usually only use it they way you would a normal anti acid, when I actually have heartburn, not every day.
I have also been prescribed statins which I do not take. My Brother died from atherosclerosis and my Mother has a pacemaker, my Dr thinks my cholesterol is too high (I also have underactive thyroid which can cause high cholesterol )and epilepsy, talk about a lame duck !
I’m so scared of taking too much medicine that I now just stick to Keppra and Thyroxine, despite my GP’s efforts to convince me that statins are the way to go.
I have developed a slightly fatalistic attitude to heart disease as I take the view that you’ve got to die of something, right ? I have seen so many other people over prescribed drugs which have caused other conditions such as type 2 diabetes and liver problems that I think I’ll stick with a low medicine regime where possible.
As ever your posts are thought provoking and informative.
As we get older, I think fatalism is vital. There is obviously a tendency to become more worried about health issues, and if that drives you to the GP surgery more frequently, it is almost inevitable that you will end up with more prescriptions!
Realising that the medicine you took as an antacid, also increased your risk of CVD, was, I am sure, something of a wake-up call! I ended up taking diclofenac for the pain caused by my statins, and omeprazole for the extra acidity from the diclofenac, and B12 injections because the omeprazole reduced my stomach acidity to the point where it could not absorb B12 from food! Oh and the statins also raised my blood glucose! After ditching all that junk, I reckon I am reasonably fit for my age, and my blood sugar is back in the normal range (though I do try to avoid sugar now).
Very interesting, David, as your case history is along the same lines as my own.
4 years after ditching the meds, I remain in need of the occasional slurp of Peptac, having developed acid reflux, due, I believe, to the ingestion of multiple, ( unnecessary) meds over many years. On picking up my ‘script this month, the pharmacist asked me to have an annual medicine review. I have never been asked to do this before, but went ahead, explaining that all I take these days is Peptac, and I thought there was very little to discuss. (But if carrying out these reviews adds to the pharmacist’s income, I don’t really mind). What does bother me though, is that when I asked my GP for the same service (a legitimate request at age 65,), it was met with derision and abrupt rudeness, as though I was being a nuisance. Strange how Government policy backs such reviews by pharmacists, yet the GP obviously didn’t think a review was needed, and that I ought to just tootle on taking ever increasing loads of tablets prescribed by the Practice Nurse.
I have managed very nicely without 3 types of hypo-glycaemics, an antihypertensive, and statins….but alas, I still require the Peptac. Why ever did I allow myself to be caught up in the spiralling situation for so long, before taking a stance, and eventually questioning the GP? Not that questioning the GP was helpful…I was told to maintain the status quo, or risk an ominous event. That was me put in my place!
If all those meds were so necessary, how come I am in better health after 4 years without them? Now that is an interesting review for the pharmacist, don’t you agree?
Just wondering whether Rennies work instead of Omeprazole for this kind of stomach acidity? They are just calcium carbonate and magnesium carbonate, and I’ve always found them effective for heartburn and acid reflux, but have no idea whether they have the same level of effect in situations where Omeprazole is prescribed.
I think the like of Rennies are where most people start, then graduate to Gaviscon before getting the hard stuff prescribed. That was my path. Now on low carb and wheat-free I’m back using Rennies for my two or three bouts of indigestion per year.
I suspect the magnesium is good, not so sure about the chronic use of calcium though.
Our practice used to insist on a Prescription Review with a nurse every six months to a year even if you’d just seen a doctor or the Prescription Manager would cancel your repeat prescription, so they also probably get a fee for so doing.
They routinely cancel naughty things like test strips for diabetics but I never heard of that happening for statins.
Pharmacists can be useful people to have onside, unless they work for Boots, who mostly just refer you here
http://www.webmd.boots.com
yes I am a bit bitter, they bought up our local pharmacy and mediocritized it. Could have been worse though, the pharmacy at the GP Practice tore up their previous agreement to serve out-of-town customers only, and are rather good.
Chris…I detest Boots nowadays. I try to find independent pharmacies, but it is getting ever more difficult.
I am appalled at the use of Prescription Czars in our NHS. A number of years ago, a friend of mine was on the point of suicide. She had an out of control colostomy, and used 8 bags a day, under the care of a Stoma nurse….so no dispute that she required them, I can assure you of that.
In desperation I visited her GP with her to support her plea, and the GP was appalled that her request for more bags had been dismissed. She got the bags in the end…..but oh dear, the worry she went through was disgusting. Only qualified medics/nurses/ practitioners, who know about caring for people, should be in a position to prescribe or withdraw medications/ appliances/ treatments, as appropriate.
Prescription Czar haha yes! I suspect their first priority is to cancel enough prescriptions that they can afford their salary. Ours had a Policy where if you requested your repeat “too early” it was either delayed or cancelled so pretty much everyone would run out of their meds on a semi-regular basis.My mother in her nineties would find something she thought she had reordered missing, assume she’d forgotten to request it and re-request it, thus proving beyond doubt that patients could not be trusted. Also it gave the pharmacy a lot of extra work making up separate prescriptions for one item each on different days.
Straight out of the American HMO/Insurance company playbook where patients got a 30 day renewal but could only request it calendar monthly.
A friend down the road (different practice, same game) had glucose test strips prescribed by her Endocrinologist (who she saw for hypothyroid). Only 50 a month, cost to NHS around £12 – £14. She used them to come off all her diabetes meds and maintain an A1c below 6% for about 15 years, and her thanks? Every six months to a year the script was cancelled and she would have to ring the Endo who would ring the GP to have them reinstated again.
I know no end of diabetics who were deregistered when their A1c went below 6% and frighteningly some were Type 1 – insulin dependent. Often without their doctor’s knowledge – the worst story I heard was a Type 1 whose repeat for insulin failed to arrive, and on ringing the receptionist was told “Oh you don’t need that any more, you’re no longer diabetic!” GP was FURIOUS. Many others who were accused of using “too much insulin” – well you kinda do when you’re Type 1 and even a cold can send your requirement soaring. Frankly charges for attempted murder should follow the charges for practising medicine without a licence. I think ours went along with the PCT and the previous Practice Manager.
As for Boots, I stopped using them years back when they told me some Neutrogena product my ex used had been discontinued. What they meant was “we decided to stop stocking it” – there was a shelf full in the Real Chemist. Oh yes and the same when I went to buy a semi-obscure motherboard battery – “Oh we don’t stock them!” On the way out of the shop through a different door I passed a stand covered in them . . . When they first took over the local pharmacy the staff used to keep a secret stash under the counter of things for their regular customers they were no longer permitted to stock, until a Regional Manager found out. Most customers voted with their feet as soon as an alternative was available, the shop is almost empty nowadays
I too, have an underactive thyroid, and had a heart attack 51/2 yrs ago. Stopped taking statins three years ago. Stopped taking Omeprazole 2 yrs ago (back on Ranitidine). The thyroid heart disease connection is interesting. I’m on 100mg Thyroxine daily (well actually at night). I’m told that too much thyroxine can cause a heart attack. I discovered that I had an underactive thyroid in 2008, the heart attack followed in 2012 but I smoked at the time. I have what I think is a pretty healthy diet, I exercise some on a daily basis and I’m not overweight. At last measure my cholesterol was 7.1 but my gp says it’s probably ‘naturally’ high? WHat does that mean? How do you tell? Last year, when I was seriously working out at the gym on a daily basis it dropped to 4.9. What the hell! I’m sick and tired of it. This ‘health’ obsession has turned me into a hypochondriac! So now I’m getting CBT.
As was pointed out to me by a friend who survived rather serious cancer, after my heart attack/operation (2 stents), I should regard every minute as time I would not otherwise have had and just live for moment.
Hi Michelle, for your hypothyroidism you might want to explore using natural thyroid, there is quite a bit written about the benefits vs syntheroid, etc. My wife has been taking NPThyroid from Acella for years now and is doing much better than on synthetic hormone. Be well, don’t be scared…
Hi Malcolm, sad to hear you have thrown out your ‘ stress response’ hypothesis. Don’t give up looking and maybe there doesn’t have to be ‘one arrow’ but many. I personally believe that most diseases and disorders begin in the gut. As we know, sympathetic dominance will compromise the the ability of the digestive process, it makes sense to me that you will then get a cascade of issues i.e. achlorhydria (hence PPI’s being a problem) bacteria, viruses etc will then not be killed off, digestive enzymes won’t be released in the same way, hence not breaking down proteins etc. This then sets up a cascade of systemic inflammation, gut permeability, lack of proper absorption of nutrients, bi products of dysbiosis, LPS, food intolerance. When you add in to this mix alcohol, antibiotics, pharmaceutical and recreational drugs, poor diet, smoking, environmental pollutants, chemicals, is it really any wonder that we create systemic inflammation that can lead to atherosclerosis ( amongst many other things).
So to me it is just dependent on where you want to look along the continuum from A-Z. Could you call stress the actual cause? I’m just not so sure it is ever as simple as that but you can certainly not rule it out as a mediator. Just my thoughts anyway. Keep up the great work!
I haven’t thrown it out, just realised that there is a bigger picture – that stress has to fit in. A bit like a jigsaw puzzle where you think you have all the pieces in order- but you haven’t. Rather than hammer the last bit in, I needed to pull it apart and get it right. Or as right as is possible.
Excellent Malcolm – always thought that stress was overrated as causal (though can contribute via hormonal effects). For your little arrow, can insulin signalling & glucose dysregulation fit in there somewhere? Pretty much all Heart Disease victims are essentially diabetic (in Europe anyway – 2015 EUROASPIRE here) : https://static1.squarespace.com/static/52faa95ee4b0b0a74811f732/t/5965da563a04116acaf3373c/1499847255723/Eurospire+Kraft.JPG?format=750w
Speaking of KD, here’s a paper discussing early athero issues in children – well worth a read. Interesting as you take a 30,000 foot view of all the important risk factors they recommend to look for (to catch the doomed kids). Forgive my confirmation bias, but they scream “insulin dysregulation”:- LDL to HDL ratios, BP, FI, BG/HG, obesity, smoking etc. They hardly mention the old LDL BS at all, except maybe that smoking oxidises the poor little LDL’s… 🙂 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2812791/pdf/kcj-40-1.pdf
Looking forward to number XXXIII !
Best
Ivor
Thanks Ivor. Of course insulin dysregulation is a big player. But you insulin fanatics (I jest) need to explain how CVD is going down whilst type II diabetes is exploding?
Yep, but smoking rates have collapsed in tandem – and you’ve mentioned a few other things that have reduced too. But is CVD going down? I have paper that shows sub-clinical athero fell until 1994 (in line with smoking reductions), then began rising again (they blame diabetes for this). We have turned a fire-hose of medications on the public which would have offset the IR-driven increases somewhat (along with the smoking etc.) – but yet we see this puppy recently:
http://www.medpagetoday.com/cardiology/prevention/63150
Looks like the diabetes elephant is beginning to stomp it’s feet, in spite of many other factors being reduced in the past decades….!
(Interestingly, smoking jacks up insulin, along with dysbiosis, stress and many other causal agents…) 🙂
But yes, it ain’t ALL the insulin/leptin etc. axis – just most of it maybe…!
The older people with heart disease (from diabetes??) are dying, to be replaced by epidemic numbers of youngsters with rampant diabetes from having been almost forcefully acculturated to sugar and all manner of other simple carbs. They’re young and resilient, so they’ll hang on for a while.
One set depleted; the other augmented.
I wonder if antibiotics aren’t skewing the ’cause of death’ results. It used to be that pneumonia, “the old man’s friend”, finished off many of the elderly. Now they are pumped full of antibiotics and something else has to kill them, and that something else becomes a ‘leading cause of death’.
It might be more useful to have some sort of cutoff point and run two sets of stats: cause of death for the young and the healthy; and cause of death for the elderly and the frail.
Not sure how to define the cutoff point. It needs to be more than just age, because older people are so much healthier these days, with longer working lives.
Possible reasons for decline in CVD deaths : procedures (stents, CABG), more medicated people (BP, statins, coumadin, aspirin etc.), quick response (ambulances, # of cardiologists, defibrillators everywhere), lifestyle (less smoking, low fat diet?)
“Mortality in the United States: From 2014 to 2015, age-adjusted death rates increased 0.9% for heart disease, 2.7% for chronic lower respiratory diseases, 6.7% for unintentional injuries, 3.0% for stroke, 15.7% for Alzheimer’s disease, 1.9% for diabetes, 1.5% for kidney disease”
How is CVD diagnosed? – BP, cholesterol, angina symptoms, ultrasound
Agree with Ivor that blood glucose and insulin are very important factors in CVD, they can also be controlled without medication. Can medication stop/control CVD?
Cancer rates are increasing and could exceed CVD rates. Blood glucose level is probably be the connection. With low chronic and postprandial glucose levels not much can go wrong (assuming macro and micronutrients are adequate).
Is there a connection between CVD and Alzheimers as well?
Ivor, I enjoyed your talk at the Public Health Conference.
The importance of insulin in the rise of obesity and diabetes is completely credible, but heart disease has been falling during the same period. The decline in smoking might be part of the answer but there is surely more to it?
Hey Stephen thx 🙂 On the run here but I replied somewhere else on this thread to similar point – is heart disease falling? It should be plummeting due to smoking, massive meds deluge and other factors – but see my link to medpage below 😉
“Yep, but smoking rates have collapsed in tandem – and you’ve mentioned a few other things that have reduced too. But is CVD going down? I have paper that shows sub-clinical athero fell until 1994 (in line with smoking reductions), then began rising again (they blame diabetes for this). We have turned a fire-hose of medications on the public which would have offset the IR-driven increases somewhat (along with the smoking etc.) – but yet we see this puppy recently:
http://www.medpagetoday.com/cardiology/prevention/63150
Looks like the diabetes elephant is beginning to stomp it’s feet, in spite of many other factors being reduced in the past decades….!
(Interestingly, smoking jacks up insulin, along with dysbiosis, stress and many other causal agents…) 🙂
But yes, it ain’t ALL the insulin/leptin etc. axis – just most of it maybe…! ”
See here what is really important in driving CVD – look to the youngest victims, for the most insight on cause: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2812791/pdf/kcj-40-1.pdf (clue – it ain’t cholesterol, unless you use non-HDL – which of course includes the jacked-up trigs ! )
Superb thoughtful blog as ever.
Would it be possible for you to provide the evidence link regarding the relationship between Omeprazole and CVD as this doesn’t appear to be in many “mainstream” thought bubbles, or is it embedded in a previous blog I have missed?
Thanks
I have covered it. Try Googling omeprazole heart disease Malcolm kendrick
In addition, it could well be that PPIs are responsible for some cancers as opposed to being a preventive.
http://www.seattletimes.com/seattle-news/health/popular-heartburn-drugs-may-increase-esophageal-cancer-risk/
Is the stress hypothesis truly dead, or does it just need more work? And isn’t it possible that many different things lead to the same outcome? If I have read all of this properly, then it is the cause of the initial endothelial damage that is the important bit (and I may have the wrong end of the stick)? Is it possible that (for instance) the drugs referred to above don’t cause the damage, but in some way make the cells more susceptible to damage? A bit out of my depth, but maybe one shouldn’t throw the baby out with the bath water?
Not dead, but needing to be re-assessed and put in the correct place.
Pleased to hear it!
p.s. you’ll love this quote from the kiddies paper (page 3, halfway down right hand column): ” In one study, children between the ages of 6 and 19 years with metabolic syndrome showed an increased risk of CVD {odds ration: 14.6, 95% confidence interval: 2.8-45.3} at 25 year follow-up compared to the general school population.”
Click to access kcj-40-1.pdf
Will read. Most interesting.
Malcolm,
Maybe I am being hopelessly naive, but could you possibly expect to find *the* cause of heart disease?
Also, isn’t the idea that there must be a mechanism part of the problem here? I mean cholesterol is still supposed to be the ’cause of heart disease’, and the ‘mechanism’ is that it is there in the plaques. All the rest of the evidence that cholesterol is innocent is just ignored!
Unfortunately poor people suffer more sickness generally, and poor people also tend to live in more polluted places, and suffer more stress – I don’t believe statisticians can possibly untangle what causes what – so do you need to fit air pollution into your theory?
Nobody searches for the cause of broken bones – playing rugby, osteoporosis, bad balance, carelessness when crossing the road, all obviously contribute. Wouldn’t something similar have to apply to the vascular system – so a quick GOOGLE tells me that Kawasaki’s disease inflames the blood vessels – so do you really need to worry that it doesn’t fit your general explanation?
Being told you have no mechanism has obviously rattled you, but the mainstream has no evidence for its theory – which is worse?
Furthermore, the mind clearly has a huge part in causing or preventing physical illness – isn’t that mechanism enough?
Tis the journey that is most important.
At last! A brilliant piece on cholesterol on RT.com.
See: https://www.rt.com/shows/watching-the-hawks/397528-pentagon-lgbt-gang-us/
About 8 minutes in
And the American Heartless Association. Apparently, the latest stats reveal that people with low cholesterol are TWICE as likely to have a heart attack.
Do you have a link?
Dear Dr. Kendrick,
Re the source: Sorry, I don’t have it but I’ve emailed RT and hopefully they’ll respond. Did you watch it? It shows that slowly, ever so slowly, reality is sinking in.
Succinct. . .
Traced it back. This is the piece by Harlan Krumholz et al from 1994.
We knew this already.
And? Is this ancient study any good? What did ‘we’ know? Unless you want to sound like the RT report, some detail would be useful (BTW, RT still haven’t gotten back to me yet).
‘Eat fat to get thin! (Daily Mail) We’re bombarded with the stuff! No wonder nobody really has a handle on reliable dietary information. We end up spinning on the spot.
I might add that some time ago (like last year) I cut out a lot of my carbohydrates. So for breakfast instead that awful muesli, I now eat a tasty trad brekkers, cooked in cold-pressed virgin coconut oil, of streaky bacon (the tastiest part of the porker), mushrooms, tomatoes and a free range egg. Delicious and I’ve actually lost weight (yeah I know, not scientific. Do I exercise? What else do I eat? Do I drink etc?)
(Not that Yale has paid much attention to it since!)
Barbrovsly,
Click on the first link for the pdf. Decide for yourself.
You might be interested in other stuff on this site as well.
https://www.bibliotecapleyades.net/ciencia/ciencia_industryhealthiermedica172.htm
JD: Thanks for the link, i’ll study its conclusions. B
Maybe Vitamin D3 is the link between stress & heart disease?
If we had optimal vitamin d levels (equivalent to the levels naturally maintained by indigenous peoples living traditional lifestyles (50ng/ml 125nmol/l) http://www.zoeharcombe.com/category/health/ ) we would be better able to regulate stress and also have CAC scores of under 100.
Here we see how even a modest daily amount of vitamin d3 lowers cortisol levels and improved CVD risk markers
Effect of vitamin D supplementation on cardiovascular risk factors and exercise performance in healthy subjects.
Click to access eResearch%204424%20pp.pdf
And Cortisol causes vitamin d deficiency.
Decreased serum vitamin D levels in children with asthma are associated with increased corticosteroid use
https://sci-hub.io/10.1016/j.jaci.2010.03.008
It’s also the case that the basic form of vitamin d3 cholecalciferol is required to maintain endothelial function and inhibit inflammation.
Dietary Vitamin D and Its Metabolites Non-Genomically Stabilize the Endothelium
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4607301/
Vitamin D Inhibits Monocyte/macrophage Pro-inflammatory Cytokine Production by Targeting Mitogen-Activated Protein Kinase Phosphatase 1
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3368346/
This paper explains the mechanism by which endothelial dysfunction leads to heart disease.
Vasa Vasorum in Normal and Diseased Arteries
http://circ.ahajournals.org/content/129/24/2557
So, In asthmatic children (or adults, for that matter), is it the inhaled steroid that causes lower D levels? Or is it the other way around?
Inhaled steroids do not seem to be a problem. The dose is small and has no discernible effect on CVD – that I have seen.
Tedhutchinson
Interesting references, I looked at the Tsimane data, and was surprised by the low level of HDL 39,5 in my type of data, and this after 6/7 hours of vigorous exercise a day. I thought exercise was supposed to increase HDL?
Any comments?
The Tsimane like the Kitavans and all those other healthy indigenous tribes follow different rules viz-a-viz lipids. Kitavans have no heart disease yet they have higher ApoB than than the CHD-sozzled Americans. Likewise they have highish trigs and not so high HDL – and their lipid ratios are nothing to write home about. The point is that lipid measures are only MARKERS for the real root causes. So in Western bad-environment peeps, the high HDL indicates that you are less insulin resistant than the other goons. Likewise the lipid ratios. Likewise the ApoB/LDL-P. But they are all intensely fallible – because they indicate better physiology – but they are not really CAUSAL in themselves. That’s why the cholesterol goons piss me off so much – they are running after fool’s gold. The monkeys.
Now that is a very brave conclusion Dr K. Thankyou. Looking forward to part 33. I bet you never thought we’d be saying that when you wrote part 1!
Neither did I to be honest.
My deep respect for this analysis and assessment to rethink again and again.
As a physical therapist I am very interested in your comment about spinal cord injury and CVD. Two questions please: (1) Can you provide a link to more information you have gleaned on this subject and (2) could spinal dysfunction (misalignment of vertebral bodies, stenosis etc) create a lesser but still measurable increase in CVD?
Thanks for your consideration and still hooked on all your postings Dr K.
You could start here. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3776463/
Many thanks! 👍🏻
That was “a few years ago” when Paul brought you up short and you realized you had to start again.
Have you started; gotten somewhere? Is there more wisdom just ahead?
I hope so
Your jigsaw analogy is very apt – perchance there is no one cause, maybe all the jigsaw pieces must be in the right order in order for CVD to develop?
Great article… but tell me, do topical creams like betnovate carry thr same CVD risks?
They do not seem to. The dose is much smaller (systemically) than with oral steroids.
MK- “That is when I ripped up the stress hypothesis, to start again. Pretty painful, but necessary.”
It’s not enough to value truth above all else. It often takes finding the courage to pursue it – wherever it might lead..
I expected NO and endothelial health to fit in somewhere on the arrow diagram, given previous posts.
Is it an established fact that plaques cannot develop behind a healthy endothelium?
I am not sure if it is an established fact. However, I think you would struggle to find any situation whereby plaques can develop behind healthy endothelium. (I have not managed yet)
When does correllation become causation?
HR > 6 is a slam dunk – According to several epidemiologists that I have spoken to on the matter. Others may disagree.
Yep – HR > 6 and you gotta sit up and take notice – recently an Asian study showed HR of ~12 for Hyperinsulinemia and breast cancer – ouch !
Not that I don’t mostly agree – but when you say “association to causation” – there are a couple of other bits:
Which way is the arrow of causation? ( fer-instance does CAD cause the slightly low HDL and high LDL that the statinfiers go on about?)
AND both variables could be caused by some third unknown variable(s).
Cushing’s syndrome is pretty much defined as and overproduction of ACTH which in turn stimulates the release of cortisol yet other glucocorticoid steroids as well – which cause other releases. One bit that misleads is the idea that these hormones have some single effect(hint – we are evolved not engineered – rare to see single functions). My hunch is that one of them acts as a growth factor or co-factor that leads to the initial thickening of the inner intima. Could work with insulin?
That being said – as someone with advanced CAD – I went through a 15-year period of my life when I was younger of extreme endless stress.. Lost my hair early as well. I’ve often wondered if that unending stress was the real cause.
This paper – where the children were under stress adds to the story
https://academic.oup.com/eurheartj/article/24/6/515/2733916/Acute-infections-in-children-are-accompanied-by
Which correlated markers are causes and which are effects? Arrow of causation matters.
But most importantly – as long as cardiologists ‘know’ that CAD is caused by LDL – it reduces the efforts to find the real cause and come up with better preventions.
xtronics: This is interesting in light of the study in Japan showing, for both men and women, a lower rate of CVD and stroke among those who had measles in childhood, and an even lower rate for those who had both measles and mumps.
Gary,
You mean to say that, had I not contracted both measles and mumps in childhood, My CAC Agatston score would have been even higher than the 1,640 that is turns out to be?
Ouch
JDPatten: I have no idea. Among Japanese men and women on a population level, having these two childhood diseases is protective. Population studies have nothing to say about individuals, though, so this one has no particular relevance to any of us. Where it is relevant is in establishing vaccination policy by governments.
Dr Malcolm,
Yes. Ouch me! I asked for the test myself to get the docs off my back about statins. I knew (thought!) I was healthy and a low Agatson would show it. Surprised me! Now I have a “preexisting condition” and the docs all have that look – like they’d rather not be on the losing team.
@Gary Ogden
But that is my point – correlation does not necessarily show causation. Could be many other explanations – correlative studies mostly show where one might find something interesting with a controlled experiment – or carefully planned series of experiments. To show the arrow of causation – we also have to look at time. Sadly, most studies are done to keep the grant money flowing – if we learn something at all, we are lucky.
What if the kids that got sick – were counted because they had better health-care? What if some treatment from getting sick had an effect? What if a 95% confidence study was one of the 5% that was off? What if the researcher fudged the data?
All of this is really tough in biology – take most any system and you will find it interacts either directly or indirectly with many other — so we add a bit of X and see a Y result – but we don’t see that X actually causes Z that effects Y. The problem is there are countless Zs.
Basing healthcare decisions on narratives that are based on correlation is how we got to the LDL nonsense in the first place – we shouldn’t replicate the process..
Ha! This just in:
CAC can be due to a lifetime of intense exercise and not NECESSARILY due to classic heart disease plaque.
http://www.cardiobrief.org/2017/07/13/coronary-artery-calcium-rises-with-intense-exercise/
(I’d like to think that this describes me and my high score.)
JDPatten, the idea that exercise causes calcified arteries seems simplistic. According to Tim Nokes endurance athletes typically carb load. His updated recommendation is to use fat as the energy source. Maybe it was the carbs and not the exercise that caused calcified arteries, makes more sense to me.
JDPatten: I read that, too, but am not quite sure what to make of it. What’s your take? It seems these folks are not dropping like flies, but live long and in good health.
Andy,
Actually, it’s always seemed to me to be a simplistic notion that a CAC score should precisely indicate your atherosclerotic plaque burden, and only that.
Inflammation from chronic infection can do it. Why not exercise abuse?
Exercise abuse can result in things like heel spurs. Why not left descending spurs? Osteoarthritis doesn’t depend on plaque.
CAC, as viewed by the Med Establishment is too precise and channeled to reflect the complexity we’re coming to expect of Life.
Of course, what you point out is indicated in the research paper. There can be a mix. Why not?
@JDPatten
These are not normal people doing normal training – These are “Masters Endurance Athletes”. The pattern of damage has been known for some time. I would not recommend anyone do marathons.
There are other papers that show the advantage of doing sane training:
Exercise Type and Intensity in Relation to Coronary Heart Disease in Men
I do a combination of strength training (al a Rippitoe ) and intervals on off days.
I listen to my body – running marathons means ignoring what your body tells you..
xtronics: I think you’re absolutely right about the harm of overtraining. I trained for, and ran, one marathon. It was the beginning of the end of my running career. Now I do strength training, short runs with a few intervals, lots of walks, and hikes in the woods.
Gary
Have you read this book
Age is Just a Number: What a 97 year old record breaker can teach us about growing older Kindle Edition
by Charles Eugster (Author)
4.4 out of 5 stars 54 customer reviews
To be brief he started sprinting at age 90, or so and was definitely very fit. I note he died aged 98, after a very active life.
So I suppose the lesson is, no generalisations?
Thank you.
Many thanks, Dr K, for being the blogger, of all those I read, who takes the most trouble to reply to your many grateful commenters. It is good to know that you really care that your message is reaching an appreciative audience.
Not much point otherwise I suppose
I had a doctor, now retired, who talked a lot about the HPA axis, and the fact that mine was ‘disordered’. He was a researcher into ME, and once mentioned that a study done at Dundee (I think) found abnormal levels of premature arterial stiffening in patients with an ME diagnosis. However, I don’t know which criteria were used for the ME diagnosis, and my doc hotly contested the eventually successful attempts by the medical profession to widen the parameters.
One consequence of my disordered HPA axis has been that I’ve ended up with ‘low adrenal reserve’, a problem not recognised by mainstream endocrinology. 24 hour saliva adrenal profiles have shown my cortisol bumping along the bottom of the graph throughout the period. I take a small amount of HC or the upstream hormone, pregnenolone, in an attempt to compensate. I have a familial risk of CVD too. My general health is poor, so I watch my nutrition and enjoy the occasional sunshine the far north of England has to offer.
Tricky area ME, one that appears overwhelmed by anger and prejudice at times, and rational debate usually flies out of the window. My own belief is that certain physical/physiological stressors can lead to HPA-axis dysfunction that can often be manifest as something, that some people, call ME. Or ME/CFS. This can, I am certain, be triggered by certain viral infections. But there are usually other things going on as well, such as mitochondrial dysfunction.
I’m glad you mention mitochondrial dysfunction; when mine was tested a couple of years ago following three decades of ill health, the results put me a long way below the bottom of the normal range. The apparent stressors leading to ME all occurred within a period of 18 months during adolescence and were mainly viral. PA and Hashimoto’s appeared in short order, followed by chicken pox at age 21. It went on from there.
Keep those mitochondria healthy – I say. I wish I knew exactly how.
One way is brief bouts of intense exercise, such as lifting heavy weights and/or short sprints.
As far as I understand Prof. Thomas Seyfried has a very good take on how the mitochondria work (it is quite complex) on different kind of fuels, sugar, fat and ketones and the latter to be preferred if you want to fight any cancer.
His book “Cancer as a Metabolic Disease” is overwhelmingly “serious” (tough reading for a lay person) – Seyfried knows what he is talking about!
The people I know with ME have suffered psychological bullying.
I think this is often the case.
TS: And scientists have had their careers destroyed. “Plague,” by Kent Heckenlively, JD and Judy Mikovits, PhD. is a shocking account of what the medical/scientific establishment can do to people who make inconvenient discoveries.
Personally i think your bad stress model is quite correct. there might be many mechanisms involved that lead to CVD and finding them all during a lifetime is a herculean task!
The sympathetic system controls our internal organs, it keeps them fully functional. So, if the sympathetic system is always triggered because a person is constantly under ”fight or flight” (for example, sexual abuse from childhood that is repressed at an emotional level, because of shame, don’t wanna talk about it etc.) this means, the body eventually enters a state where the sympathetic system will simply stops to function properly. (exhaustion?) Which in turns will lead to an array of body symptoms, and eventually to the heart stopping. What i wrote was simplistic, but it’s the idea that matters.
Why the heart stops?
maybe the sympathetic system send a kind of neuro-electric current to the heart, and at one point that wiring starts to be faulty.
See under Takotsuba ‘heart attack’ a pure sympathetic overdrive condition, causing the left ventricle to change shape into that of a Japanese octopus trap. No, I am not making that up. Go to Google and type in Takotsuba – an increasingly recognised cause of central chest pain and a form of ‘heart attack’ brought on purely by severe emotional stress.
My grandfather died in 1933 during the Great Depression. Great shape, non-smoker – death certificate showed acute indigestion. He was having an argument with my father who was 12 at the time. He died during the argument. Did I mention he had 7 kids and one on the way and they lived in rural Alabama. That the definition of stress and the result. All of his kids except my father lived or are living long healthy lives. Dad died of a heart attack and all his sons (myself included) have high calcium scores. Wonder if the stress of a fleeting second be passed on in the genes?
Could have been a heart attack presenting with symptoms of indigestion. Happens a lot.
Interesting.
https://en.wikipedia.org/wiki/Takotsubo_cardiomyopathy
Emotional stress, just like cortisol, when it stays too high for long period of times, months or years, will weaken the immune system and the adrenals to the point of rendering them almost useless. So, with a weak immune system, a vast array of microbes, bacteria, viruses and what not, could alter the normal functioning of the heart, not to mention a vast array of ”dis-eases” as well, like diabetes.
I’m inclined to think that Elizabeth Cappetta is on to something here. We know so little about the microbial sea in which live, yet we assault it and attempt to alter it at every opportunity. Thanks again, Dr. Kendrick, for never having lost your curiosity.
What about Dr. Sroka’s observations about the heart rate variability approaching zero at the time of an MI?
I think that would be very interesting. Do you have a reference to this?
Here is a reference.
Click to access K._Sroka_2.pdf
I have tried to understand what this is about but have so far failed.
This is all very interesting. I am learning so much… Thank you!
Here’s my take on the link between stress and cardiovascular disease:
1) Stress is known to deplete magnesium in the body, a mineral which is generally said to be in short supply these days in our diet due to modern farming techniques.
2) Blood serum tests done by the NHS are not useful to pick up any deficiency because the blood serum levels are maintained by using the body’s stores of magnesium until it is no longer available – so only when the body is seriously low in Mg will it show up in the standard test .
3) Low magnesium levels are known to be closely associated with heart disease.
http://www.medicalnewstoday.com/articles/255783.php
…and a further link on the same lines – http://www.todaysgeriatricmedicine.com/archive/050613p30.shtml
This one might be of interest…
https://www.ncbi.nlm.nih.gov/pubmed/11485106
CONCLUSIONS:
Different categories of psychological measures to varying extent are associated with characteristic patterns of coagulation and fibrinolysis activity. Associations between psychological factors and several coagulation and fibrinolysis variables related to atherosclerosis provide a plausible biobehavioral link to coronary artery disease.
Yes, I think this is a fascinating line of enquiry.
Would using something like this be beneficial to the body producing too much cortisol? Or is this just the opposite of what a person would need? I think I’m maybe not understanding what it is you’re saying about cortisol. (?)
Enter the world of cortisol physiology at your peril. It is fearsomely complex.
That’s ok, I read a blog by a great chappie called Malcolm Kendrick. I expect he will be soon providing a “Cortisol Physiology for Dummies” blog soon. 🙂
Another piece of great information! Thank you for your study!
Indeed, if you can excuse the purple prose, the sage & precious Dr Kendrick is worth his weight in Rubies.
Proverbs ch 3 verse 15 has it right, Rubies are still more valuable…
Stick at it Doc.
“guinea pigs on a scorbutic diet rapidly developed atherosclerosis. When I say rapidly, I mean within days. I think this point is worth repeating. If you make a guinea pig scorbutic, it will develop plaques, identical to those found in human arteries within days.” — https://drmalcolmkendrick.org/2017/01/16/what-causes-heart-disease-part-xxiv/
If you stress guinea pigs, do they also develop plaques? It might be interesting to run a stressed group and an ascorbutic group of guinea pigs in tandem and contrast commonalities and differences in the plaque-forming mechanisms.
One more “dot” to connect in the link between stress and myocardial damage is the Mast Cell. there are actually CRH receptors on the cell membrane so that sufficient stress to cause activation of the HPA will also cause activation of mast cells with release of inflammatory mediators. Mast Cells can release as many as 200 different mediators (maybe more) resulting in multiple manifestations of diseases depending on genetic predisposition and location of mast cells.
You cited an example of this: the TakoTsubo and Kounis syndromes.
https://tmsforacure.org/expert-information/mast-cells-heart-kounis-syndrome-takotsubo-cardiomyopathy/
The mast cell–a potential link between inflammation and cellular cholesterol deposition in atherogenesis https://www.ncbi.nlm.nih.gov/pubmed/8131778
Oxidized Low-Density Lipoprotein Contributes to Atherogenesis via Co-activation of Macrophages and Mast Cells
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4374860/
And we can start to link to acute coronary syndrome:
Mast cells and acute coronary syndromes: relationship between serum tryptase, clinical outcome and severity of coronary artery disease
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5051537/
I am also a believer that infectious causes of atherosclerosis can occur via the endothelium or adventitia , and the mast cell could be the connection, with multiple possible triggers:
The possibilities are endless:
Mast cells and inflammation
http://www.sciencedirect.com/science/article/pii/S0925443910002929
I think that many cases of POTS and non-epilleptic seizures in patients with “dysautonomia” as well as Lyme disease and co-infection are related to Mast Cell Activation Disorders. This can be carried on to explain many of the manifestations of “heart and vascular” diseases.
I hope that this stimulates further discussion and thought!
Are mast cells something that the average person should be stressed about?
My interest is in understanding how research can be applied to daily living. Read the references. Then I googled “mast cells and hyperglycaemia” the indication was that they are associated. Conclusion: keep blood glucose controlled by diet and don’t worry.
Dr. Gerber: Thank you for this. Interesting that you mention POTS. This is a common adverse reaction to the Guardakil shot. I wonder if these girls are now at greater risk for CVD.
Gary: you probably know already… Vaccines Revealed documentary is now showing at http://www.vaccinesrevealed.com
It’s very well done.
Sasha: Thanks. Yes, I was aware of it, but haven’t yet had a chance to view it. Looks like it covers information I’m already aware of. I certainly would recommend it to anyone concerned about human health.
Thank you, Dr. K. So candid and so brave. I still your connecting of stress, in times of war and/or severe social disruption for example and increased heart disease is very very plausible.
Malcolm, as an admirer of your work thank you again for sharing. I am interested to know how increased CVD risk due to family history fits in to the whole causation picture?
I don’t think there is any true family history in CVD. As in, genetic – perhaps epigenetic.
What about CHIP, as described in this article. Various genetic anomalies are mentioned that effect heart disease . . . they say.
https://www.medpagetoday.com/cardiology/atherosclerosis/66181
JDPatten, loods like ageing can induce DNA mutation. Autophagy via mTOR pathway to the rescue, Also reduce oxidative stress from excess carbs.
Nature. 2013 Feb 21;494(7437):323-7. doi: 10.1038/nature11895. Epub 2013 Feb 6.
FOXO3A directs a protective autophagy program in haematopoietic stem cells.
Warr MR1, Binnewies M, Flach J, Reynaud D, Garg T, Malhotra R, Debnath J, Passegué E.
Abstract
Blood production is ensured by rare, self-renewing haematopoietic stem cells (HSCs). How HSCs accommodate the diverse cellular stresses associated with their life-long activity remains elusive. Here we identify autophagy as an essential mechanism protecting HSCs from metabolic stress. We show that mouse HSCs, in contrast to their short-lived myeloid progeny, robustly induce autophagy after ex vivo cytokine withdrawal and in vivo calorie restriction. We demonstrate that FOXO3A is critical to maintain a gene expression program that poises HSCs for rapid induction of autophagy upon starvation. Notably, we find that old HSCs retain an intact FOXO3A-driven pro-autophagy gene program, and that ongoing autophagy is needed to mitigate an energy crisis and allow their survival. Our results demonstrate that autophagy is essential for the life-long maintenance of the HSC compartment and for supporting an old, failing blood system.
I know its the elephant in the room, but Jack Kruse seems to be pretty adamant that most disease today is caused by chronic blue light and the ever increasing nnEMFs in the form of wifi and 3g, then 4G and then 5G. This then combined with critically low Vit D levels and distored circadian biology.
I think you would struggle to fit all of disease epidemiology into chronic blue light exposure.
What you eat could also affect CVD by increasing cortisol
HEART HEALTHY WHOLE GRAINS > gliadin > zonulin > leaky gut/brain > brain function altered (anxiety, depression, hostility, insomnia ) > increased adrenalin/cortisol (adrenalin dysfunction) > mental stress > more cortisol
HIGH CARB DIET > postprandial and chronic hyperglycaemia > increased cortisol (HPA axis dysfunction) > gluconeogenesis > blood glucose level increased > more cortisol
EFFECT OF HIGH CORTISOL: increased blood glucose, immune response reduced, increased inflammation, increased blood pressure, central nervous system activation, altered thyroid function, reduced bone density, fat/protein/carb metabolism altered, increased abdominal fat, metabolic syndrome, arthritis, acid reflux, depression, chronic fatigue, insomnia, hostility, anxiety, etc..
Again we are looking at one end of the outcome scale(the bad one) and trying to work out why. How about looking at people with good outcomes despite multiple alleged risk factors. Currently doctors just call these people “lucky”. By the same logic, people having AMIs are just unlucky.
I am 57, with longstanding T1 diabetes, a family history of vascular disease, on a higher dose of steroids (both cortisol AND prednisolone) long term than doctors recommend, have high cholesterol, refuse statins, refuse the antihypertensives that 4 doctors have recommended, eat a diet very high in saturated fat, and stopped going to the dentist 15 years ago.
Yet my cardio-respiratory function exceeds 99.5% of the general population my age. I achieved this by copying people with good outcomes from the same endocrine conditions. By doing what successful people do. Not by following medical advice.
Medical researchers still refuse to collect information on people like me. Wouldn’t want any data to upset the applecart, would we?
A good point. The book, the Blue Zones is very interesting in this regard. A study of people who live the longest. Dr Aseem Malhotra and Donal O’Neil have just published a book called the Pioppi Diet. Based on a village in itlay where people live long and healthy lives. I have a copy sitting in front of me – but I haven’t read it yet.
Dr. Aseem is along my LCHF line. This book about the Pioppi diet seems to be “popular” and when I read the following article arguing against Pioppi and Dr. Aseem it cooled me down.
https://health.spectator.co.uk/the-pioppi-diet-is-a-superficial-lifestyle-guide-based-on-distorted-evidence/
My view on LCHF is that we have for sure the basic metabolic science on our side so we don’t need to go “popular”.
to Dr. Sjöberg,
That’s debatable. For example, Aloe Vera moisturize the skin, therefore would you make a link between dry skin and the lack of use by human beings of Aloe Vera?
Just because eating a LCHF diet remove the symptoms of diabetes in many human beings, doesn’t mean a carb rich diet is the culprit.
If they are the only two conditions being considered I would disagree.
Gaetan, not sure about aloe vera. LCHF has been good for me too. Anything that raises glucose and insulin is a big culprit in my estimation too. There are many other culprits as followers of this blog are discovering.
Gaetan,
You are certainly right about this!
As far as I understand this it is a wrecked metabolic system (the metabolic syndrome), which though seems to affect half of the worlds population today, which opens up for the “treatment” with LCHF. And here it is “all” about insulin resistance in my present world. Anyway, optimal treatment seems to be a diet 80 % fat (natural – no PUFA) and 20 % high quality protein from the animal world to restore your health.
“Overindulgence” as a “cause” is in my eyes simplistic official stupidity – no science here! Normally it takes about 30 years to gain those 30 extra kilo, which is one indicator of the metabolic syndrome, so then you have “evidently” constantly been “overeating” 3 grams per day (no character?). The “stupidity” is here obvious to say the least but few seem to realize this.
Insulin is by the way a fat storing hormone so to keep it low has a logic which is done by cutting the carbs – you don’t need them!
As Gary points out – do the opposite to what is officially recommended by the dietitians and doctors (except the recommendations from our Malcolm) to get your health back.
Hello & hmm,
1) i don’t have health problems ! 🙂
2) i think you all failed to understand my point. LCHF is not a treatment but since it doesn’t cause insulin resistance (no sugar in the blood) the symptoms go away for many. That doesn’t mean sugar is the culprit whatsoever, it simply means, many people lost the ability to digest a rich carb diet, why? i do not know. Probably has to do with adrenals and sympathetic system being out of touch, just a guess. Why is the pancreas not working properly or why do the cells prevent insulin from doing its job?
3) people also heal their diabetes by eating rich carbs diet.
or
https://www.deathtodiabetes.com/fruits-that-help-reverse-diabetes.php
etc.
4) Just like Aloe Vera is a solution for dry skin, LCHF diet is a solution for diabetes. But neither address the root cause of the problems IMHO. I too, if i were diabetics would switch to LCHF to not have the symptoms anymore. Just like i use ALoe VEra because i haven’t found yet why i have had dry skin forever !
Pioppi diet might not have the same effect in an urban environment. Pioppi is an ideal place to live.
Agree
Gaetan . . . I think I I understand your point. You seem to be saying that people with diabetes (T2D) have ended that way because they have developed insulin resistance (IR) – to which most these days would agree. You seem reluctant to speculate on how people developed the IR in the first place, and you seem reluctant to put the blame on carbohydrates.
Like you, I would say that T2D folk have lost he ability to deal with high carb diet diet effectively – 40g carb per day is a problem for many.
My issue is in saying that “LCHF diets is not a treatment” for T2D. In my case after a few months of LCHF my HbA1c drop into pre-diabetic region, and after 1yr dropped to 34 mmol/mol. My fasting insulin measured a year ago was low.
So, I would say that LCHF was definitely a *treatment* . . . that is : it was an ‘intervention’ that suppressed the dangerously high levels of damaging serum glucose.
The question I now ask myself is this: Was the LCHF treatment a *cure* . . or is it simply a way to control my diabetes – have I regained insulin sensitivity? Am I now able to deal with more carbs? . . . can I say I no longer have diabetes . . .(which is where I think you are at Gaetan).
I have a little evidence that I may have mended . . . after some very naughty cheese cake/cheese and biscuits and wine a while back I checked out the glucose 2 hours later . . . down to 5.4 (fist pump) mmol/l . . 3 hrs 4.9 mmol/l (double fist pump)
I am now planning to see where I stand on IR – glucose tolerance. I will go for a 2hr Caryn Zinn version of the IR test – fasting blood sample – 100g glucose – wait 2 hours – another blood sample. Send off the samples to get the insulin checked. See how hyperinsulinaemic I am. It is going to be fun getting my doctor’s practice to cooperate.
Will also take the fasting glucose so using this and the fasting insulin I can work out the HOMA-IR – to see what it has to say about my insulin resistance and beta cell function.
If I have mended then LCHF goes from *treatment* to *looks like a cure*.
One experiment I could try is to go back to the bread/potatoes/pasta diet that I was eating before diagnosed as T2D – regain the 25kg that I lost – and see if I end up T2D diabetic again.
Andy S,
One thing that strikes me in Pioppi, if i understand correctly is, they work on their lands as farmers throughout their lives and don’t have food addiction as they are relatively poor. Obesity is non-existent.
So, i believe, yes as i don’t have scientific evidence, that physical exercises, keeping our body fit, is the PRIMARY marker for health and lengthy life. Then comes the emotional well-being and the positive or negatives thoughts we put in our minds, lastly is the food we eat, as long as it is food.
For example, if someone buy ”food” in a grocery, but that food can last weeks on a shelf, it is not really food, but a food-like product. real food decay, after a week most real food becomes inedible. Sure there are exceptions, especially with a freezer. But my point is most of the food in a grocery is not food but food like products.
https://health.spectator.co.uk/the-pioppi-diet-is-a-superficial-lifestyle-guide-based-on-distorted-evidence/
”Do you know what the people of Pioppi actually eat? Processed carbohydrates. Farm workers in rural Italy do not – could not – survive on a diet of fish and seasonal vegetables. Pasta is as central to the Italian diet as potatoes are to Britain’s. So too is bread. This is the elephant in the room for anyone trying to pretend that Italians eat a low carb diet. As a 94 year old Pioppi resident said last year: ‘Pasta is my favourite food. I don’t understand why so many people try to cut that and bread out of their diets – it is like medicine for the heart and it is silly not to eat it.’
Once you accept that pasta and bread are important elements of Mediterranean cuisine, the actual Pioppi diet involves lots of fruit, vegetables, fish, starchy carbohydrates, mushrooms, nuts and eggs, but little or no cake, biscuits, processed meat, crisps and red meat. In other words, it is the UK government’s Eatwell Guide with extra virgin olive oil. Maybe those official dietary guidelines are not so deadly after all?”
Gaetan, in Canada we had the official food pyramid. My doctor gave me a copy 10 years ago and I followed the recommendation to eat 7-11 servings of carby foods. Found Atkins and tried that, dropped 15 lb. Occasional excursions into high carb meals resulted in AF type heart palpitations. This is my experience, we ate all different. I have found what works for me: low carb(leafy greens,carrot+beet juice, berries/fruit in season), high fat (coconut oil. butter, lard, olive oil), adequate protein ( eggs mostly, cheese, sardines, animals)
Calories from carbs do count if you want to maintain your weight and health.
On the average a Pioppi diet would probably be suitable, a few individuals might not find it so good. One diet does not fit all, there are literally thousands of diets, find the one that works for you.
Yes, that’s what I saw in Italy also. They all eat pasta practically at every meal. And bread fairly often too. You rarely see overweight people, at least in Northern Italy, especially those older than 30 or so. The younger generation seems puffier for some reason but nothing compared to the US or UK.
Italians could be more tolerant to wheat consumption by natural selection over thousands of years, similar to milk consumption. Consider the Pima and other cultures. Also there is adaptation to diseases, temperature, altitude, native foods etc.. Could carb tolerance be and adaptation? The French paradox took a while to be solved, there are many more paradoxes to investigate (Pioppi paradox?).
There was no French Paradox. There was an incorrect theory, which was contradicted by the French data. Instead of accepting the facts, the ‘experts’ called it a Paradox. Calling facts a paradox is a long established way to support hypotheses, when you cannot think of any other way to explain what you found. It is the weakest form of post-hoc hypotheses. There should be a general rule. Once you find two paradoxes, that do not fit your hypothesis, your hypothesis is wrong, and must be discarded.
I think it also has a lot to do with the quality of their pasta. I have also seen some people say that our gut biome is extremely malleable and can change drastically within a few months.
Andy S,
i’m going to play the devil advocate here.
”Italians could be more tolerant to wheat consumption by natural selection over thousands of years, similar to milk consumption. ”
People on HFLC diet could be more tolerant to meat & fat consumption by natural selection over thousands of years, similar to milk consumption.
“Could carb tolerance be and adaptation?”
Could meat/fat tolerance be and adaptation?
see?
We can say anything about a diet and people who thrive on it or not.
Many ancients cultures relied mostly on carbs.
For example the Aztecs;
http://www.aztec-history.com/aztec-food.html
the mayans;
http://ancientmayalife.blogspot.ca/2012/12/food-of-ancient-maya.html
The roman and greek empire mostly relied on bread & wine;
https://www.thespruce.com/eating-like-an-ancient-greek-1705715
and many more.
But then the nordic tribes, for example the inuits, relied mostly on fat and meat. what else could they eat anyways in the frozen north?
So maybe the diet has to do with what is available and what is not.
Would you say the inuits were more healthy? i doubt it overall.
Gaetan, I was thinking outside the box. All species adapt to eating what is available, koala, panda, grizzly bears come to mind. They are health eating their evolutionary diet, difference is carbivores small/ carnivores large. Humans are omnivores with large brains trying to find out what is a healthy diet, too many experts, food choices and diet books. Fast forward to a million years from now where humans exist on corn, wheat, soy and beans. Due to population pressure humans might evolve back into a shrew sized creature, our primitive ancestors .How will our dietary decision made now affect the future of mankind? Could be a good topic for a movie akin to Planet of the Apes. Come to think about it, were the apes vegetarian in that movie? Just thinking outside the box.
Gaetan: Read a book by Bernal Diaz del Castillo “The Discovery and Conquest of Mexico” one of the conquerors. Maize and veggies was not the only source of food, humans were kept in cages and fattened for eating. Human sacrifice did not go to waste, the bodies were distributed for food.
Cannibalism was not a rare occurrence historically. My suspicion is that the neanderthals met the same fate.
Gaetan: Diet is indeed directly related to what is available. Pre-Columbian Mexico and central America were particularly poor in protein sources from large herbivores, unlike the northern parts of north America, Europe, sub-saharan Africa, and parts of Asia. This explains the dietary choices of the Aztecs and the Mayans. The bodies of the victims of Aztec sacrifices were distributed to, and shared among, the priestly class, since they were such a valuable source of complete protein.
Did the Pioppi Diet authors speak to the local doctor? You can’t tell the true state of a population just by looking around. Animals in the wild all look so fit and healthy, yet they are often infested with ticks and fleas and intestinal parasites. If you could ask them, “How are you today?” you’d probably get the usual human range of grumbles and moans, plus of course the sick and the infirm get taken out by predators. In Pioppi maybe the sick and infirm get carted off to a faraway hospital or locked up in the attic.
Then there’s infant and child mortality. If you are not adapted to the local diet you will die young in the absence of medical care. It could be in Pioppi you are looking at a population sample skewed by the grim reaper. Certainly that would have been the case in older times.
Andy S,
I have read a book by Bernal diaz del castillo, he was in charge of recording the conquest alongside Hernan Cortes. When they arrive near Tenochtitlan (the Aztec Capital) what they see put them into wonderment, they can’t believe their own eyes about the magnificence of what they are looking at. A white city, with many plants of all kind, Jewels, statues etc. not going to write a novel here…
So in the end the conquistadors killed Moctezuma and his son Cuhotemoc, and that was it for the Aztecs, the very end of a civilization caused by greed and religious beliefs.
About cannibalism, i think it was a practice not just among the Aztec, albeit quite rare i believe, but also among the islanders, haiti, dominican republic, cuba etc. (of course those islands had different names back then)
Christopher Colombus, the greatest murderer of all times, oops i mean explorer, is probably responsible for the massacre of all the original indians living on their islands and which were replaced by black slaves bought on the market.
Quite different from what i heard when i was a little kid in school.
To all,
Again, the point i am trying to make is, human beings eat what is available to them, and meat i believe would come last because hunting requires skills, cooperation, and can be dangerous as well. so why bother when we have fruits hanging out of trees, or mushrooms popping up from humidity, not to mention stealing eggs here and there or collect nuts or grow various kind of plants.
I don’t think old civilizations asked themselves if they had enough fat or carbs. I think for most, finding food to eat 3 times a day was already a big deal. More so that they probably suffered from malnutrition or were simply undernourished, where as today most of us are over-nourished. Or at the very least we can eat whenever we want, even when not hungry…
I realize you’re talking about the West but overall, a full third of the world’s population is either undernourished or malnourished. According to the book “The End of Plenty”, agronomists estimate that once you take into account what’s fed to farm lot animals, rice, wheat, and corn provide about 85% of all calories consumed by humans. Thus, the discussion on whether one should be vegan or LCHF can only take place among the affluent. A very big part of the human population are just happy when they have enough to it.
nickmelhuish: Good! I generally do the opposite of medical advice, and have excellent health. A bit more than a year off my only drug (lisinopril). What I’ve noticed in recent months: Since I’ve increased my mineral intake (potassium, salt, and magnesium), I no longer get those annoying minor injuries that plague athletes, and I recover faster. Two days ago I took a 6-mile (10 km) hike from 7,000′ to 9,000′ (2,552-3,280m) and back. Within 24 hours I was still tired but pain free. This was my first hike of the season. Minerals are important! Don’t skimp on them, especially salt; The kidneys are admirably designed to deal with salt, and too little is dangerous; very difficult to eat too much.
Well, as you’ve always said, CHD is multifactorial. I think stress must have a huge role to play. I presume you’re familiar with Prof Robert Sapolsky’s work at Stanford. It’s some time since I read his book, ‘Why Zebras Don’t Get Ulcers’, so can’t remember if he said anything about heart disease.
Sapolski is a hero of mine. Love his work. He has looked closely at stress in Baboons due to battles for social supremacy. Lots of data on cortisol and white blood cell counts, and suchlike. Very strong links with stress and infections.
About Baboons I read a personally interesting note that only those baboons who are bold attract females. Then it must be all about the hormone testosterone which is known to bring on the baldness. This was a comforting knowledge for me when I lost most of my hair in the early twenties.
Does testosterone induce CVD?
Bold should be bald of course!
Bold and bald, a dangerous combination I feel.
I guess you are right about bald+ bold.
My life experience, at 70 now, tells me that it is the “rough” guys (bald + bold?) who has a swarm of beautiful dangerous (?) women around while we timid guys (bald and timid) face an uphill challenge in this realm. With my “baldness” I have though not have had any serious problems with the opposite sex – e.g. I have never experienced any negative remarks referring to my “hairstyle”.
Dr. Göran Sjöberg: I am as bald as you, a process which began in adolescence, but seem to be getting less timid with age. I do have a full complement of facial hair. A couple of years ago I stopped cutting all of it, so I’m a bit wild-looking. Call me a crackpot, but I think this has had a positive impact on my health, plus I save on razor blades and barbers.
Zebras must have a genetic switch that rapidly turns off the stress response when danger is over. Research should be conducted to find the genes and develop medicines applicable for humans. Alcohol and pot might give a clue.
Fair play . Have to say I was fascinated the first time I read your writing re spinal cord injury and autonomic dysfunction . I love learning something new . Just finished Terence Kealeys Breakfast is a Dangerous Meal . Delighted to hear what he had to say about fat cell biochemistry and his description of an atherosclerotic artery plaque content : “it’s pus”. Brilliant ! I could see it in one .. keep it coming Malcolm . Thanks
Very good
There wasa time when I sub’d to a printed copy of New Scientist here in Oz. But in recent years it has declined and I have sought my science elsewhere. ( Including now here )
Out of pure curiosity I just did a search of your name “Dr Malcolm Kendrick” on New Scientist’s website.
There were no results at all ! New Scientist either does not ‘know’ you or chooses not to ‘know’ you.
I am not shocked.But this does confirm what i already thought. It has gone downhill.
And in finding this blog it seems i have found an elite company of people keenly interested and well informed on human health.
I am reading up on the link between insulin and ferritin and the effects high insulin has on iron storage in the body. Blood tests may include hemoglobin, but ferritin results less than iron overload levels do not get any attention. Here in the USA, all the flour is fortified with iron. Men have higher levels of iron than women, in general. The effects of gradually increasing ferritin don’t effect women until after menopause, which is when they start catching up with men in terms of iron, diabetes. Does this apply to CVD too?
Margaret; It is also interesting that cancer cells sequester ferritin (and glucose) as a way of metabolic growth; could high levels of both glucose & ferritin contribute to cancer cell development? LCHF diets (Warburg effect) have a role in supressing cancer development, and more recently artemisinin is being used to slow cancer cell growth by attaching to ferritin in the cell, and creating a peroxide, which degrades or kills the cancer cell, with very few side effects. Recent trials in London with colorectal cancer show ART to be effective…..cheap & few side effects… (My case study records support this theory)
Does high Iron ferritin levels in the blood have an effect of heart disease ? PD Mangan at Rogue Health has written a number of posts with peer reviewed science papers, showing that high ferritin Iron levels are indeed associated & probably a causal factor in heart disease.
http://roguehealthandfitness.com/?s=Iron
Mangan’s primary focus is on older males seeking to prevent or slow aging via such things as High Intensity Training, a Low Carb diet, Intermittent Fasting, a range of OTC supplements and keeping iron ferritin levels ‘optimal’ rather than ‘normal’. He suggest that the normal range used for blood tests includes significant numbers of people who have high iron levels, thus biasing ‘upwards’ the range used.
Wow, what a great website. I learned Metformin lowers body iron. I have Type 2 diabetes, but avoiding medications. So maybe I will just donate blood and convince my doctor to order a ferritin test along with the HbA1c tests. (N=1 experiment.) Many thanks for your input.
Altern Ther Health Med. 2017 Jul;23(4):26-32.
Oral Consumption of Vitamin K2 for 8 Weeks Associated With Increased Maximal Cardiac Output During Exercise.
McFarlin BK, Henning AL, Venable AS.
Abstract
Background • Vitamin K1 and K2 are not typically common in a Western diet because they are found in a variety of fermented foods. Vitamin K2 in particular has been demonstrated to restore mitochondrial function and has a key role in production of mitochondrial adenosine triphosphate. Thus, it is reasonable to speculate that dietary supplementation with vitamin K2 could increase the function of muscle with high mitochondrial content (ie, skeletal and cardiac muscle). Objective • The purpose of this study was to determine if 8 wk of dietary supplementation with Vitamin K2 could alter cardiovascular responses to a graded cycle ergometer test. Design • The study was a randomized controlled trial. Setting • The study took place in the Applied Physiology Laboratory of the Department of Biological Sciences at the University of North Texas (Denton, TX, USA). Participants • Participants were aerobically trained males and female athletes (N = 26). Intervention • Participants were randomly assigned either to a control group that received a rice flour placebo or to an intervention group that received vitamin K2. For weeks 1 to 4, participants received 300 mg/d; for weeks 5 to 8, they received 150 mg/d. Subjects assigned to the control group received similar doses to mirror the intervention group. Subjects consumed the supplements during an 8-wk period while they maintained their typical exercise habits. Outcome Measures • At baseline and postintervention, participants completed a standard, graded exercise test on an electronically braked cycle ergometer. Before the test, participants were fitted with a mouth piece, and their oxygen consumption, carbon dioxide production, respiratory rate, and respiratory exchange ratio were measured. In addition, participants were fitted with skin-mounted electrodes that measured noninvasive cardiac output, stroke volume, and heart rate. To assess the cumulative exercise change, an area-under-the-curve (AUC) value was calculated separately for each outcome variable at each treatment time point.
Results • Vitamin K2 supplementation was associated with a 12% increase in maximal cardiac output, with P = .031, with a trend toward an increase in heart-rate AUC, with P = .070. No significant changes occurred in stroke volume.
Conclusions • Although vitamin K2 supplementation has previously been reported to improve cardiovascular function in diseased patients, to the research team’s knowledge, the current study is the first to report its potential in active individuals. More research is needed to fully evaluate the potential effects of the observed effects.
PMID: 28646812
Erett,
That is a HUGH amount of K2. Every thing I’ve read about supplementing with K2 suggests taking 150 to 300 micrograms (mcg) per day. The numbers in this study 300 mg/d (300 milligrams/day) are 1000 times those numbers. Could “mg” be an error?
Phil
Renfrew, PA USA
Are these milligrams (mg)?
That would be about factor 1000 over common supplements.
The one I finally bought (because it not silly-underdosed) had 2700 micrograms K1 and K2 total per capsule. And I use to split this dose to about a week (in oil) because I figure uptake of small doses is better.
However Strunz reports K supplements being used in milligrams in Japan to fight osteoporosis, IIRC.
I suppose it just depends on finding a source that sells you vitamin K by the gram. Unfortunately, K1 seems to come more commonly in grams than K2 does.
The French Paradox Explained.
In Kate Rheaume-Bleue book, Vitamin K2 & The Calcium Paradox.
How a little-known vitamin could save your life.
She explains the French Paradox, It was one of the books I could not put down
I have Kate Rheaume-Bleue’s book. It is a good one and well researched. However I prefer Dr Dennis Goodman’s recently published book ” Vitamin K2; The missing nutrient for Heart & Bone Health” ( Author-House 2015 ) It is simply shorter, less detailed & easier to understand.
NB : K2 needs to be taken with D3. This helps prevent calcification of the. arteries by ensuring calcium is absorbed into the bones preferentially instead of the arteries. But it is not a complete explanation of heart disease. Other processes are at work. I have taken K2 & D3 for 3-4 years. But in November last year found out that I still had a high calcium score. And ordered to take statins which I declined for reasons all here know & understand. My refusal lead the cardiologist to refuse me as a patient. And so I have sought to find out what is going on myself. hence my genuine pleasure to find Dr Kendrick’s web site.
In the meantime I have I have read elsewhere that high iron ferritin levels in the blood is necessary part of the inflammatory process. There are damaging micro-organisms in the body and in the bloodstream. These micro-organisms need iron to grow and expand. Where ferritin levels are low this micro-organism expansion is restrained.and so too is inflammation. And then the CVD process is also restrained. But in persons with high ferritin iron blood levels such organisms can access that iron, multiply and then cause CVD.
Pre-menopausal women generally have lower ferritin iron blood levels because of the regular loss of iron via blood flow. And generally also have less CVD risk. However after menapause, the risk of CVD rises for women gradually to equal that of men.
Thus, as well as D3 & K2, one of my own fixes has been to take B3 Niacin which actually chelates iron from the body reducing ferritin iron stores. Of course this needs to be guided by blood tests to prevent anemia.
Here is a link which studies ferritin Iron levels and CVD. ( From Annals of Pharmacology ? )
https://books.google.com.au/books?hl=en&lr=&id=41WECgAAQBAJ&oi=fnd&pg=PA318&dq=iron+cardiovascular&ots=yyriNY9XMV&sig=Gsg32Et7-eUnvTw7cpHDtPl1RKs&redir_esc=y#v=onepage&q&f=false
https://blog.bulletproof.com/106-the-powers-of-vitamin-k2-with-dr-kate-rheaume-bleue-podcast/
Joy! And thank you Dr Aseem Malhotra in the Pharmaceutical Journal for endorsing what Dr Malcolm has been saying for many a year and for others who are now backing his report. Dr Malhotra is quoted in today’s Daily Express as saying “There appears to be no clear reduction in coronary heart disease mortality in Western European countries from statins for primary…and secondary …prevention. The researchers conclude that lowering cholesterol shows no benefit on mortality, no reduction in cardiovascular events and reports of substantial harm. Instead of “should have gone to Specsavers” how about “should have read The Great Cholesterol Con”!
Hi all
A brand new blog from Dr Mike Eades called “Why are doctors so stupid particularly about nutrition”.
Here’s the link:
https://proteinpower.com/drmike/2017/07/11/why-are-doctors-so-stupid/
I’ve been these waters with the NHS healthcare professionals and I know many visitors to Dr Kendrick’s website/blogs over the years have too.
N.B. Dr Eades signs off details of his next blog on saturated fat and LDL levels.
Can’t wait!
The cholesterol and calorie hypotheses are both dead — it is time to focus on the real culprit: insulin resistance
http://www.pharmaceutical-journal.com/20203046.article?clearcache=1
14 JUL 2017 By Maryanne Demasi, Robert H Lustig, Aseem Malhotra
This suggested link does not work. Can you please change or ncorrect it ?
Charlie, Here is the right web address link :
http://www.pharmaceutical-journal.com/opinion/insight/the-cholesterol-and-calorie-hypotheses-are-both-dead-it-is-time-to-focus-on-the-real-culprit-insulin-resistance/20203046.article
This doesn’t work either. Is it because I’m in the U S?
Currently here
http://www.pharmaceutical-journal.com/20203046.article
The original article pointed to from a blog post literally disappeared after I switched to the pdf link to download it and switched back again.
Naturally i assumed dieticians had had it deleted already but digging around I refound it, presumably they were doing some site reorganisation.
Charlie, could insulin resistance be a “condition” (INSULIN RESISTEMIA) rather than a “culprit” ? A pathological condition where cells would rather die than be stuffed with more glucose.
The authors’ conclusion: “In summary, for many patients at high risk of CVD, one of the safest and most effective ways to reduce the risk of heart attack and stroke is to consume a high fat and low glycaemic load Mediterranean diet and engage in regular exercise. ”
“The real culprit” that gets you into “insulin resistant state”, ie. low fat diet with omega 6 seed oils plus excess calories that increase abdominal fat. Abnormal blood glucose levels can explain many of the problems of CVD, cancer, Alzheimers etc. etc..
Good evening from Holland dr Kendrick,
After having read you commentories for quite some time we would like to raise the question : whether or not it wise to continue using statins when a person has had heart surgery due to heart problems, my husband takes  medicines for high bloodpressure and simvastatine. Our doctor told him he had to take them for the rest of his life. He had a ICD inplanted after his operation in 2010.
We read that in that case you need statins so he takes them every night. We like to hear from you what is wise.
For your information, wr can say we are keeping good health due to a healthy lifestyle. My husband is 77 and I,am 71 years.
We would appriciate to hear your comment, Sincerely yours, Nanno and Coosje Bakker
P.s. Today we read in our newspaper an article about people dying due to taking medicins, the name of dr. Peter Gotzsche and your name. ..statins leads to heartattacks and suicide. That brought us to wright this mail to you, excuses for our dutch/english writing.
Verzonden vanaf Samsung-tablet”Dr. Malcolm Kendrick” schreef:
Bakker,
Myself with a serious heart disease (CVD) since 20 years would never dream of taking any statins. With Peter Gotzsche I consider it as a criminal activity of GP’s to prescribe statins to guys like me and even a more criminal act to people without any heart problems. Stupidity is a too mild expression – it is corruption of the health care system! There is no science and no logic whatsoever in this behavior!
Ferritin interacts with elevated insulin according to this paper:
http://www.jbc.org/content/249/21/7024.short
There is an association with elevated ferritin with insulin resistance.
http://www.sciencedirect.com/science/article/pii/S0026049510000971
My take is it hasn’t been shown that ferritin is a problem on it’s own ( I still wouldn’t take iron supplements).
If I eat real foods, don’t get fat, don’t have insulin resistance – I think there are better things to worry about.
Instead of thinking about keeping BG down – it should be insulin. I wonder if the risk from insulin is the area under the curve or if the peaks matter?
xtronics
The first paper is fascinating . . it seems to show that in 1974 people were trying to work out details of the insulin receptor that we now take for granted . . It says what they were trying to do in its title “Electron Microscopic Demonstration of Insulin Receptors on Adipocyte Plasma Membranes Utilising a Ferritin-Insulin Conjugate” They felt they demonstrated that the insulin receptor was only found to be active on the outside of the cell membrane and the insulin molecule only acted from the outside and was not taken into the cell. They needed a procedure to chemically attach the insulin to ferritin to show up the insulin in the electron micrographs. There is no indication in the paper that serum ferritin and insulin would react in the body on their own.
I agree with your emphasis on focussing on insulin. In aYouTube video I watched a few months ago Ivor Cummins champions he work of the late Dr Kraft which shows that measuring postprandial insulin levels over 5 hours is a far better predictor of metabolic health than fasting glucose or HbA1c.
The problems is that we *do* have home kits for measuring BG levels, but there are no equivalent insulin meters.
” I wonder if the risk from insulin is the area under the curve or if the peaks matter?” good question.
My belief is that peaks matter. But I cannot provide you with any clear cut evidence.
Allostatic load is “the wear and tear on the body” which accumulates as an individual is exposed to repeated or chronic stress. It represents the physiological consequences of chronic exposure to fluctuating or heightened neural or neuroendocrine response that results from repeated or chronic stress.
https://en.wikipedia.org/wiki/Allostatic_load
Vegetated land cover near residence is associated with reduced allostatic load and improved biomarkers of neuroendocrine, metabolic and immune functions.
Egorov AI1, Griffin SM2, Converse RR3, Styles JN4, Sams EA5, Wilson A6, Jackson LE5, Wade TJ5.
Author information
Abstract
BACKGROUND:
Greater exposure to urban green spaces has been linked to reduced risks of depression, cardiovascular disease, diabetes and premature death. Alleviation of chronic stress is a hypothesized pathway to improved health. Previous studies linked chronic stress with a biomarker-based composite measure of physiological dysregulation known as allostatic load.
OBJECTIVE:
This study’s objective was to assess the relationship between vegetated land cover near residences and allostatic load.
METHODS:
This cross-sectional population-based study involved 206 adult residents of the Durham-Chapel Hill, North Carolina metropolitan area. Exposure was quantified using high-resolution metrics of trees and herbaceous vegetation within 500m of each residence derived from the U.S. Environmental Protection Agency’s EnviroAtlas land cover dataset. Eighteen biomarkers of immune, neuroendocrine, and metabolic functions were measured in serum or saliva samples. Allostatic load was defined as a sum of potentially unhealthy biomarker values dichotomized at 10th or 90th percentile of sample distribution. Regression analysis was conducted using generalized additive models with two-dimensional spline smoothing function of geographic coordinates, weighted measures of vegetated land cover allowing decay of effects with distance, and geographic and demographic covariates.
RESULTS:
An inter-quartile range increase in distance-weighted vegetated land cover was associated with 37% (95% Confidence Limits 46%; 27%) reduced allostatic load; significantly reduced adjusted odds of having low level of norepinephrine, dopamine, and dehydroepiandrosterone, and high level of epinephrine, fibrinogen, vascular cell adhesion molecule-1, and interleukin-8 in serum, and α-amylase in saliva; and reduced odds of previously diagnosed depression.
CONCLUSIONS:
The observed effects of vegetated land cover on allostatic load and individual biomarkers are consistent with prevention of depression, cardiovascular disease and premature mortality.
Published by Elsevier Inc.
KEYWORDS:
Allostatic load; Chronic stress; Depression; Green space; Health effect biomarkers
PMID: 28709033 DOI: 10.1016/j.envres.2017.07.009
We need to keep in touch with nature. Absolutely, one hundred per-cent.
Trees give off chemicals which have a calming effect on humans. There is speculation that it dates back to our evolutionary past when we were an arboreal species. Trees feel like “home” to us.
My N=1 experience confirms this. After reading the article in New Scientist, I started eating my lunch in a small grove of trees near the office. I definitely felt calmer and more relaxed than when I ate in the office.
A couple of other articles of interest:
“A new study found that an additional ten trees on a given block corresponded to a one-per-cent increase in how healthy nearby residents felt.” — http://www.newyorker.com/tech/elements/what-is-a-tree-worth
“The Japanese practice of ‘forest bathing’ is scientifically proven to improve your health” — https://qz.com/804022/health-benefits-japanese-forest-bathing/
Remarkably, insulin resistance and metabolic abnormalities in the knockout mice were largely alleviated after treatment of NAC. n-acetylcysteine
Oncotarget. 2017 Jun 28. doi: 10.18632/oncotarget.18793. [Epub ahead of print]
Insulin resistance in vitamin D-deficient mice is alleviated by n-acetylcysteine
Cui ZH1, Yuan Q1, Mao L1, Chen FL2, Ji F3, Tao S1.
Author information
Abstract
Vitamin D deficiency will lead to insulin resistance. In the current study, vitamin D3 1α-Hydroxylase [“1α(OH)ase”] knockout mice were generated to mimic vitamin D deficiency in vivo. As compared to the wild-type mice, the liver tissues of the knockout mice showed impaired insulin signaling, decreased glucose transporter 4 expression and increased reactive oxygen species production. Meanwhile, p53-p21 activation, apoptosis intensity and pro-inflammatory cytokines (IL-6, IL-1 and MIP-1α) level were significantly increased in the knockout mice livers. Significantly, such effects in the knockout mice were largely attenuated by supplement with anti-oxidant n-acetylcysteine (NAC). Remarkably, insulin resistance and metabolic abnormalities in the knockout mice were largely alleviated after treatment of NAC. Therefore, inhibition of oxidative stress by NAC alleviated insulin resistance in vitamin D-deficient mice. Oxidative stress could be the primary cause of insulin resistance by vitamin D deficiency.
KEYWORDS:
N-acetylcysteine (NAC); inflammation; insulin resistance; oxidative stress; vitamin D
PMID: 28687021 DOI: 10.18632/oncotarget.18793
Emotional trauma and CVH.
An anecdotal evidence.
When Russia invaded Finland during WW2, and made the Fins sign a peace agreement with the soviet Union after stealing a good hunch of their land, here is what the Finnish president, Kyosti Kallio said with bitterness after he ratified the treaty;
”Let the hand wither that is forced to sign such a treaty” A few months later his wish was fulfilled when he suffered a stroke that paralyzed his right side.
From the book – the deadly embrace –
And if you look at the explosion of heart disease in Finland after the great forced relocation of people in Karelia at the end of WW2 – well, makes you think.
p.416
”no less than than twelve percent of the population lived in the Isthmus, well over half a million people. They had to moved out within 2 weeks of the signing of the ‘peace’ treaty, and resettled elsewhere.(…)they left behind their houses, their businesses, their livelihood – everything they could not carry with them.”
Being relocated against our will is definitely traumatizing. The ability to cope with trauma is equally very important. Maybe the difference in CVH is actually this ability to cope with trauma.
Possibly. I think resilience is partly physiological, partly (learned) psychological, and partly sociological – by which I mean how much support do you have from others around you.
Yes absolutely, and how much support one’s willing to get on his own. It’s a body-mind matters / combo. Visiting a modern doctor and taking a statin is probably the worse outcome. Lifestyle changes, attitudes changes and so on will lead to long lasting health improvement. But this you mention all the times.
‘Stress’ in any way associated with CVD ? – My (not any more!) cardiologist vehemently asserts that even ‘association’ is a load of ……..
Despite n=1, I have no doubt that (mishandled?) stressors/Depression from a head surgery had a starring role in the drama a year later, of “ALL” my old stents clotting.
Naturally it was all my fault, in part due to SDS. – Statin Deficiency Syndrome.
I await your re-defined pathway from Depression to (heart) Disease…
Mr. Chris: Agreed. Staying active, both mentally and physically, is one of the keys to a good life. The marathon experience was great fun, as about 30 of us trained together and participated, but it went beyond my physical capability. I’ve since found greater benefit in building muscle mass, with a little bit of aerobics, than in chronic aerobics only. I have no intention of stopping, whatever age I keel over. I just can’t sit much.
Gary
The Pioppi diet contains lots of carbs, bread pasta etc. If you are doing hard manual work, such as low le vel farming you will burn those up rapidly. As the good doctor explained in June 2015, the problem with carbs comes when you don’t burn them up, they are converted to Palmitic Acid and stocked. If I am going to do something strenuous, I stock up on toast and marmalade!
Mr. Chris: How right you are. Manual labor surely will burn all the carbs you can shove into the pie hole. I had another hike in the giant sequoias today, actually two, each about 4 miles (13 Km total), drinking deeply of nature. Moderately strenuous. What did I crave among the foods in my day pack? The apple and a big bag of raisins, eaten with gouda and manchego cheese. Carbs are sometimes good for us.
Now that you mention it, looking back to when I was as my peak in fitness/weight/glucose control, I was concentrating on resistance (as opposed to aerobic) training.
Not only the physical benefit, but the deep, fundemental satisfaction etc that comes from pushing more /ALL weights on a seated leg press… more than many younger blokes… – Priceless !
D.O.B – Middle of last Century.
James: Resistance training makes me feel better than running ever did. It is under-rated; it is powerful and easy to do (I use body weight only). Plus I can lift the ordinary objects we deal with in daily life without injury, regardless of their weight.
A useful definition for ‘general fitness’ especially for the more senior folk…
Desperation must be setting in if today’s article on Science Daily is anything to go by!
https://www.sciencedaily.com/releases/2017/07/170724172718.htm
The Steven Nissen wind up toy. Put money in the wallet, and the Steven Nissen toy will play any song you want. (Warning, requires almost continuous insertion of money to operate at maximum efficiency).
So you’re saying a large garden gnome wouldn’t do? Has anyone checked?
Hahahahahaha classic!
Tom Dayspring too, allegedly. And when I read that Professor Lord Sir Rory Collins was in change of the UK Biobank my first thought was “Is it in the Cayman Islands?”
Don’t be too hasty in dismissing ‘stress’ as a major causative factor in cardiac events. It took over 50 years to grow my first occlusion a… And 12 months of intense Stress. to take my health from ‘perfect’ down to a 5 way CABG …. We won’t dwell on the cardiac benefits of living on the edge of mental collapse, or a pre-emotive strike!
My impression is that mental/emotional state is more significant in determining likelihood of. subsequent. events, than the First one.
I have far from dismissed stress – if I have given that impression then this would be in error. I have just realized that stress must be fitted into a wider picture.
Dr Kendrick
The French= sociable, less sugar, saturated fat= very low incidence of CVD
Or, put otherwise, sociable= low Stress
By the tone of your comment, I take it that this particular Talking Head is well known for such utterances, . – Dilutes his gravitas somewhat. . .
I wasn’t sure where to add this link but I am finding more and more, on social media, almost exactly the same information you, Dr Kendrick, have been documenting. My worry is when will the government get rid of the processed c*** on our supermarket shelves and concentrate on whole, nutritious foods. Maybe, not until we talk with out feet!
I didn’t need any confirmation of the information on your pages, but sometimes the way information is presented adds to my understanding. Thank you Dr Kendrick for all your efforts and hard work.
Here’s a link, professionals are catching on and admitting they are wrong!
http://www.somedaily.org/world-renowned-heart-surgeon-speaks-really-causes-heart-disease/
I believe this is a very complex issue. I leave this recent post of my blog about the complexity of cardiovascular disease.
https://pesescadhta.com/2017/08/18/why-some-people-with-very-risky-lifestyle-and-lots-of-risk-factors-can-live-longer-than-others-free-of-risks-a-long-standing-question-in-medical-practice/
Dr Kendrick, I’m very glad to read this blog article as I have just finished your excellent book (Cholesterol Con) and found the stress hypothesis you suggested just a little too simplistic. Which is not to say that I didn’t find that whole section highly informative and very useful indeed but I did feel you had somewhat over-egged that pudding.
One question I have arising from the book is that you point out that veins do not become atherosclerotic but arteries do but you do not go on the offer any explanation as to why this is the case. Has this been covered elsewhere, perhaps in a blog post? I would greatly appreciate you pointing me in the right direction.
Many thanks for your excellent book and contribution to the field of improving human health. I have used your information to try and persuade my mother-in-law to give up her statins.