I have been waiting for some time now before it became officially impossible to be healthy. In recent years the boundaries of health have been inexorably squeezed tighter and tighter. Recently, they snapped shut. The land of the healthy now no longer exists. Tis but a memory.
I wondered if it would be cholesterol that would obliterate health first, but it turned out to be blood pressure. This was pretty much second favourite in my book.
As with many areas of ‘health’ the definition of a healthy blood pressure has fallen and fallen. A few years ago we had go to the stage of a condition known as pre-hypertension. A state of having a high blood pressure that wasn’t really high, but represented an ill-defined danger of some sort. This pressure was set at 115/75mmHg. Far lower than the average blood pressure in the Western World.
However, with the latest CV prevention guidelines (yes, them again) we have managed to get the optimal systolic blood pressure down to 90mmHg. Underneath, you will see a little graph that I created using the CV risk tool. The tool can be downloaded here:
So you can check out for yourself that what I am saying is true.

I put in figures for a healthy male, and then only changed the blood pressure level. As you can see, as the blood pressure goes up, the risk of a CV event goes up, and vice-versa. Going from 90mmHg to 150mmHg causes your risk to go up from 2.6% to 6.5%. A 250% increase in relative risk. What this tells us is that 90mHg represents the absolutely optimum blood pressure. Anything higher and your risk increases, and it increases quite steeply.
By definition, this means that a systolic blood pressure of 90mHg is ‘healthy’ and anything above this becomes increasingly ‘unhealthy.’ Now it has to be said that a systolic blood pressure of 90mmHg is low. Pretty damned low. Indeed, I have been asked to check patients out because their systolic BP was 90mmHg, and the nurse was rather worried about them.
I can hardly blame the nurse for this, because the definition of hypotension (dangerously blood pressure), is…yes, you guessed it, a systolic blood pressure of 90mmHg and lower. You can check this ‘fact’ on the National Institutes of Health site.
This means that we have reached a situation whereby a systolic blood pressure lower than 90mmHg increases risk; and a blood pressure higher than 90mmHg increases risk. I suppose you could say that anyone with a blood pressure of exactly 90mmHg is healthy, so the land of health still exists as a microscopically thin sliver of habitable area. But for all intents and purposes, health has gone.
Can it really be true that there is no such thing as a healthy blood pressure?
In order to believe this you have to believe in the linear or log-linear model. A model that can, to a major degree, be laid at the feet of a certain Jeremiah Stamler. He stated that ‘the relation of SBP (systolic blood pressure) to risk of death is continuous, graded, and strong, and there is no evidence of a threshold.’ In short, as BP goes down, risk goes down, and there is no lower limit beyond which this is not true. Well, until you reach 90mmHg, it seems.
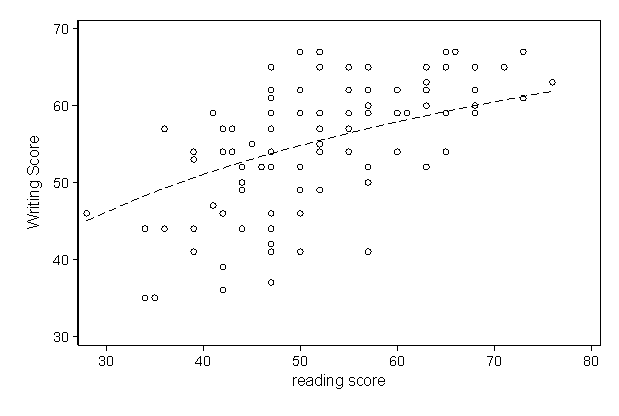
This idea is based on mathematics, whereby Stamler took all the studies he could find, matched BP with risk, and then created his perfect curve. You can see how this type of thing is done by looking at a curve created by matching writing score vs. reading score. [I took this example from the internet1]. The dots may seem all over the place, but there is a trend from bottom left to top right.
The curve is a linear model, which smooths out all of the data variations. Excel spreadsheet will even calculate a curve like this for you, if you have a graph with dots which may seem completely random.
In the world of hypertension, the log-linear model rules.
‘This(the log linear model) is the paradigm for the relationship of all cardiovascular risks to blood pressure, and forms the foundation of the current guidelines for hypertension.’ These words from the European Heart Journal in the year 2000, since then the paradigm has not changed, and neither has the model. The latest CV guidelines are based on it.
How could it be otherwise? Do you really think anyone has done a study lowering blood pressure from 100mgHg to 90mmHg? If so, think again. In fact the model was first created from the Framingham study data. This is the world’s longest running, and most cited, study on cardiovascular disease. It has been running since 1948 in a town called, unsurprisingly, Framingham in the US.
Now, this would be all fine and jolly – if the model were actually correct.
In 1980 Ancel Keys, who is not my favourite ever person it must be said, looked at the Framingham data. He concluded that the linear model, in terms of the relationship between overall and coronary heart disease was unjustified.
Twenty years after this, a group of statisticians from UCLA looked at the data again. And here is what they said:
‘Shockingly, we have found that the Framingham data in no way supported the current paradigm to which they gave birth. In fact, these data actually statistically reject the linear model. This fact has major consequences. Statistical theory now tells us that the paradigm MUST be false for the target population of the study.’2
Was this paper refuted? No, not exactly….
“The National Institutes of Health’s National Heart, Lung, and Blood Institute (NHLBI) issued a statement regarding Port’s findings saying that they found it “thought provoking” but “After careful review of this study, the NHLBI finds that it does not offer a basis for changing the current hypertension guidelines.”
End of.
Which means that we are here. A world where health was finally extinguished by using a mathematical model. A perfect world for the pharmaceutical industry. Everyone is ill, and all shall have medications, for ever.
‘Can you do Addition?’ the White Queen asked. ‘What’s one and one and one and one and one and one and one and one and one and one?’
‘I don’t know,’ said Alice. ‘I lost count.’
2: Port S. et al: ‘There is a non-linear relationship between mortality and blood pressure.’ European Heart Journal (2000) 21, 1635-1638