29th December 2017
What is stress?
I have talked about stress quite a lot, but as many people have pointed out, the word itself is meaningless. Or perhaps it would be more accurate to say that is has too many meanings, or that it means different things to different people.
Paul Rosch, a very brilliant man1, told me that when he was first looking at stress soon after the Second World War, he was working with Hans Sayle, a Hungarian. Sayle often commented that, had he understood English better, he would have used the word strain, not stress. He fully understood that ‘stress’ is the thing that creates ‘strain’ on the body. It is strain that matters, not the stress.
This, I think, is absolutely critical. You can look at some people’s lives and they may seem highly ‘stressful’, whereas others appear to be relaxed, and avoiding stresses wherever possible. However, you have no idea at all who is under the greater strain.
I remember a cardiologist, many years ago, pointing to an elderly woman who had just had a heart attack. ‘She lives in an idyllic cottage in the middle of the country, married, with loving children. No stress at all. So, don’t tell me stress causes heart disease.’ I merely shrugged. How could the cardiologist possibly know what was going on under the surface?
Perhaps her husband came home and beat the living daylights out of her every Saturday night. I remember seeing another lady, a few years earlier, who was deeply upset because she had been in hospital for an operation, and whilst there her husband had her two, very large, dogs put down.
Yes, she loved the dogs, but her main anxiety was that she had bought them for protection. When her husband went out for an evening and drank, he would come home and beat her mercilessly. She had bought the dogs for to keep her safe, now they were gone.
This couple were upstanding members of the community. They were regarded as having a perfect marriage and a perfect life. He was a magistrate and a local businessman, she ran a couple of charities. Having heard her story, I later watched them together, smiling and a laughing at local events. This was after I knew what actually went on in the home. Superficially, I could not tell anything was amiss between them.
On the other hand, some people can appear to lead lives that are full of stressors, yet can cope very well. Probably because have good physical and psychological resources, and are highly resilient. They usually have many other supportive factors in their lives. A loving partner, friends, family, and suchlike.
I think we are all also guilty of deciding that what causes us strain, will also cause someone else strain, and vice-versa. In fact, identical stressors can create very different effects. I give a few lectures every year. I quite enjoy it, I feel in control, and confident that I am good at giving talks and I find the process positive and enjoyable. However, I know of people who find the idea of standing up in front of other people absolutely terrifying. To them, giving a lecture would create massive negative strain.
In short, we cannot know the strain that someone else is under by looking at what they do, or how they act. Even massive events, such as having a partner die, will not have the same impact. For most of us this would be shocking and terrible. However, if your partner has been an abusive bully for thirty years, their death may come as a relief. Yes, it is all complex stuff indeed.
The reality is that, if you want to know if someone has suffered a level of negative stress, sufficient to have damaged them, you have to measure it. Yes, the dreaded objective medical science. Of course, before measuring things you have to have a hypothesis to test.
The hypothesis here is reasonably straightforward. It is as follows. Long term negative stressors (or one overwhelming acute event) can create damage to the neuro-hormonal system that coordinates the physiological reaction to strain. This, in turn, has negative physiological effects that can lead to serious disease e.g. CVD, or diabetes, or both.
If a tiger walked in the room, we would all react in pretty much the same way. Sudden terror. This would activate a vast array of different responses, and this reaction starts in the hypothalamus – deep within the brain. When stimulated, the hypothalamus releases hormones that, in turn, activate the pituitary gland to release further hormones. These hormones travel to the adrenal glands where the stress hormones are synthesized. Cortisol, adrenaline (epinephrine) and suchlike. This is called the Hypothalamic-Pituitary-Adrenal axis (HPA-axis).
The stress hormones that are released, speed up the heart rate, release glucose into the bloodstream, dilate the pupils, shunt blood supply from the guts to the muscles, and suchlike. At the same time the unconscious nervous system, which is tightly interwoven with the HPA-axis, lights up, and this puts every other system in the body onto ‘fight or flight’ mode. The blood pressure goes up, sweat glands are activated, blood clotting factors are released, and so on and so forth.
This is all normal, and natural and, assuming you survive, after about twenty minutes, or so, all systems start to wind back down to ‘normal.’ If the fight or flight system switches on ‘accidentally’ due to a perceived threat, that is not a real threat, this is usually called a panic attack. Which is why some people go nuts on aeroplanes and try to open the doors at 35,000 feet. In the midst of a panic attack the conscious mind is over-ridden, as the persons ‘inner chimp’ desperately tries to flee the situation. [The ‘Inner chimp’ is the part of the brain fuelled on impulsive emotion and gut instinct].
Some people who suffer from post-traumatic stress disorder (PTSD) are far more likely to see threatening situations all around them, and trigger panic attack mode far more often than others. Their fight or flight system has been set to super-sensitive mode. A child shouting may trigger the memory of a battlefield attack. Ditto a plane passing overhead, or a car changing direction rapidly. Not easy to live in a state of hair-trigger fight or flight.
Children who have been physically, or sexually abused have much the same hair-trigger systems in place. They live life on high alert, and are ready for fight or flight at any time. Billy Connolly, a Scottish comedian, who was abused when he was a young boy, always said he did not like being touched. It brought back memories that setoff deep, negative reactions.
All this is well known, and widely accepted. What is less widely accepted is that repeated activation of fight or flight can, in time, lead to a breakdown/burn-out/dysfunction of the HPA-axis and the unconscious nervous system – usually called the autonomic nervous system. In part, this is because people have steadfastly measured the wrong things, at the wrong times.
Perhaps the single greatest ‘measurement’ problem is to look at cortisol levels only n the morning. Cortisol is a key ‘stress’ hormone that is released in response to stressful situations. It also naturally fluctuates during the day. It rises to its highest level in the morning, just before you wake up, then it drops. Then rises and falls during the day.
Researchers, looking to link ‘strain’ to heart disease, and diabetes, and suchlike, have made the mistake of only measuring early morning cortisol in those with CVD, and found it to be lower than normal. They have then stated that HPA-axis dysfunction cannot be an underlying cause of CVD and/or diabetes – or any other serious medical condition.
This, of course, is exactly the wrong interpretation. If the HPA-axis is damaged, the normal rise and fall of cortisol, will break down. Or, to put it another way. A burnt-out HPA-axis leads to ‘flat-line’ cortisol production. It gets pumped out at the same rate – no matter what is going on Therefore, if you measure the cortisol level in the morning, in those with HPA-dysfunction, it can appear to be low, not high.
The correct way to diagnose HPA-axis damage, is to take regular cortisol measurements over a twenty four hour period. This was known by a Swedish researcher called Per Bjorntorp, who used hourly measurements of cortisol, to see what the flexibility of the HPA-axis was in people suffering from ‘cardio-metabolic disease.’ That is, people who have the ‘metabolic syndrome.’
The metabolic syndrome is a group of abnormalities that are often found clustered together. Abdominal obesity, high blood pressure, raised blood sugar levels (sometimes high enough to be called type II diabetes), raised clotting factors, high triglycerides/low HDL, higher LDL levels, high insulin levels.
This syndrome is also (has also been) called: insulin resistance syndrome, pre-diabetes, syndrome X and Reaven’s syndrome. Whatever you call it, it is the same thing. It is associated with a greatly raised risk of CVD. Around six-fold in some studies a.k.a. 600%.
Per Bjorntorp did a series of studies looking at HPA-axis dysfunction, and the metabolic syndrome, and he concluded that the underlying cause of the metabolic syndrome was indeed HPA-axis dysfunction. Here, I quote from his paper. ‘The metabolic syndrome – a neuroendocrine disorder?’
‘Central obesity is a powerful predictor for disease. By utilizing salivary cortisol measurements throughout the day, it has now been possible to show on a population basis that perceived stress related cortisol secretion frequently is elevated in this condition. This is followed by insulin resistance, central accumulation of body fat, dyslipidaemia and hypertension (the metabolic syndrome). Socio-economic and psychosocial handicaps are probably central inducers of hyperactivity of the hypothalamic–pituitary adrenal (HPA) axis. Alcohol, smoking and traits of psychiatric disease are also involved. In a minor part of the population a dysregulated, depressed function of the HPA axis is present, associated with low secretion of sex steroid and growth hormones, and increased activity of the sympathetic nervous system. This condition is followed by consistent abnormalities indicating the metabolic syndrome. Such ‘burned-out’ function of the HPA axis has previously been seen in subjects exposed to environmental stress of long duration.’ 2
It shouldn’t really be a great surprise that if you damage the HPA-axis/autonomic nervous system that you will end up with the metabolic syndrome. The short-term effects of activating the flight or fight system are to: raise blood pressure, raise blood clotting factors, raise blood sugar levels, raise LDL, and direct energy stores out of subcutaneous fat.
If this becomes a chronic state, you will end up with chronically: raised blood pressure, raised blood clotting factors, insulin resistance/type II diabetes and increased abdominal fat/central obesity, as fat stores are moved from the subcutaneous to the central fat stores.
We have a perfect model confirming this sequence with Cushing’s disease. This is a condition where excess cortisol is produced in the adrenal glands (usually due to a small cortisol secreting tumour). The long-term effects of Cushing’s disease are:
- Raised blood pressure
- Raised blood clotting factors
- Insulin resistance/type II diabetes
- Raised VLDL, low HDL (dyslipidaemia)
- Central obesity
- Greatly increased risk of CVD, around 600%
In short, long term increased cortisol production, creates a severe form of the metabolic syndrome, and a very high rate of CVD.
I suppose the final link in the chain is to look at what happens if we prescribe people cortisol. In truth, we do not do this, not exactly. Instead, we prescribe them corticosteroids. These are often just called ‘steroids’. They are used to treat inflammatory conditions, such as asthma, Crohn’s disease, Rheumatoid arthritis and suchlike.
All the prescribed corticosteroids are synthesized from the basic cortisol template. Cortisol is also called a corticosteroid, because it is a steroid hormone manufactured in the ‘cortex’ of the adrenal gland. One commonly prescribed corticosteroid is prednisolone, and the chemical structure of cortisol and prednisolone can be seen in the two diagrams.
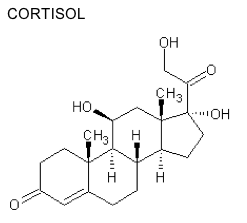
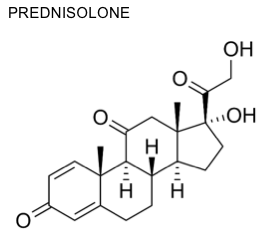
If you prescribe steroids long-term, they too cause insulin resistance, then the metabolic syndrome, then type II diabetes, and much higher risk of CVD. The risk of CVD is increased by, up to, 600%. 3
Personally, I see this whole issue as a bit of a ‘slam dunk,’ where all the evidence fits together in an almost perfect causal chain:
Bjorntorp, in a series of well controlled studies, demonstrated that environmental ‘stressors’ can lead to HPA-axis dysfunction/physiological strain. This, in turn, leads to the metabolic syndrome. The metabolic syndrome, in turn, leads to a vastly increased risk of CVD.
PTSD is also a condition where the HPA-axis is dysfunctional4, and the rate of CVD is vastly increased5. Equally those who are victims of childhood abuse demonstrate HPA-axis dysfunction6 and a greatly increased risk of CVD7. Severe depression is also associated with HPA-axis dysfunction8 and a greatly increased risk of CVD9.
The key hormone in this process appears to be cortisol, because a high level of cortisol, independently of HPA-axis dysfunction, also leads to the metabolic syndrome, and a very high rate of CVD. In addition, if you prescribe corticosteroids they, too, lead to the metabolic syndrome and a very high rate of CVD.
Which of the elements of the resultant metabolic syndrome are most important? This is not entirely clear. Is it the raised blood pressure, the clotting factors, the high insulin or sugar? To an extent it does not matter that much. If you can get rid of the underlying cause, they will all disappear.
Next blog. How to get rid of the underlying cause?
1: https://www.stress.org/about/chairmans-blog/
2: https://www.cambridge.org/core/services/aop-cambridge-core/content/view/S0007114500000957
3: http://www.bmj.com/content/345/bmj.e4928
4: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3182008/
5: https://www.ncbi.nlm.nih.gov/pubmed/27566327
6: https://www.ncbi.nlm.nih.gov/pubmed/15471614
7: https://www.ncbi.nlm.nih.gov/pubmed/24923258
8: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC181180/
9: https://academic.oup.com/eurheartj/article/35/21/1365/582931

HAppy Hogmanay
Will people manage to turn their comments towards diet?
I think we should be told
Would be interested in your views on using meditation as a help in reducing stress
The healthy body runs upon a healthy homoeostasis. Perhaps relative homoeostasis would be a better term. It has to make constant adjustments to all the complicated molecular goings on inside. The natural biological aim is to keep the molecular goings on as close to the Goldilocks ideal as is possible and for as much of the time as is possible. Chronic stress represents a departure from the biomolecular sweet-spot, and yes, perhaps we should think of stress as a cause and strain as the effect, ie departure from relative homoeostasis.
There is an undeniable mind-body relationship. Fear can be sprung upon us or we can conjure fears of our own, either way the body and inner biochemistry invokes a fight or flight response. The experience of persons who meditate is that it calms both mid and body. Even without hard edged empirical data and trials of the kind it can take to convince members of the medical profession this n=1 one experience reported by a great many ‘n’s ought to be convincing enough.
These days all a person need do to follow a hunch is enter certain terms into a search engine, better still Google Scholar. The internet is full of reliable information but beware for the good stuff is mixed amongst all the bull-crap.
“Cortisol” and “meditation” will return a great many results; including this:
https://www.nhs.uk/news/lifestyle-and-exercise/does-meditation-reduce-stress/
In this instance I feel inclined to side with the articles assessments.
It’s been awhile since I’ve participated in this stimulating discourse because I’ve been having a strainful year which appears to have culminated in three, I think connected conditions.
Firstly, about ten years ago I discovered that I had an underactive thyroid and was put on (ultimately) 100mg of Thyroxine, which athough not a perfect treatment, sufficed. Then in 2012 I had a heart attack and two stents inserted. That too, seems to have worked, after a fashion, though I still shiver if the temperature drops below 22-23C and I have brittle nails, two classic symptoms of hypothyroidism.
Then in 2015, after being on statins for three years, I took the plunge and dropped the damn things. In that same year I started to exercise more, walking every day, doing cardio workouts.
I have always eaten healthily I thought, low carbs, 70-80% veg, fish, chicken, a little red meat ocassionally, don’t smoke, the odd drink, weight, for my build, good.
But when I stopped taking the statins I was ‘bullied’ for a year by my doc, consultants, even specialist lipid nurses were launched at me, all claiming that I would die. And of course I will die, eventually. When I challenged them over how much ‘extra’ time the statins would give, no answer was forthcoming.
The upshot of this was that by last year I was, I suppose a hypochondriac, every ache and pain, weird thing in my body (I’m nearly 73), set me off. So I decided to do one of these CBT courses and to a degree it was quite helpfulin restoring some perspective.
Until a month or so ago, when I started to get palpitations, I assumed my heart, though some seemed to emanate from my solar plexus. Whatever. So I went to the doc and he thought I had atrial fibrillations and he put me on beta blockers (that I have rather unpleasant adverse reactions to), sent for an ECG and I got a workout for my bloods.
Low and behold my TSH was 7.5 ‘normally’ between 1 and 2), I was pre-diabetic (6.3%) but I’m not sure about the atrial stuff and neither is my doctor. And I’d lost 7kgs! What is going on I wondered?
So, back to the strain. I surmise that the strain has affected my thyroid, they think I’m now hyperthyroid, which in turn has affected my heart rythmns and the pre-diabetic, where does that come from? I don’t eat any processed food, rarely drink, don’t ever drink sodas in any form, don’t eat fast food, though I do, perhaps once a month devour a bar of super dark chocolate, but that’s about it.
So, thyroid to heart arythmia to pre-diabetic: I strain the connecting thread I wonder? In 2015, the consultant who saw me about the statins denied there was ANY connection between stress and a wonky thyroid, and so far two gps at my surgery concur. I’m not so sure.
Me too. I’ve been taking ‘steroids’ (inhalers) for asthma for about 40 years. I also have a plentiful supply of visceral fat. Dead man walking.
Inhaled steroids are not a problem, too small a dose.
Tony Youens: Giving up grains got rid of my visceral fat in about three weeks. One of the smartest things I’ve ever done.
Robert Sapolsky convinced of this some years ago when I read his book, Why Zebras Don’t Get Ulcers. I have since noted it in myself – even though I keep calm, when in company for some hours with ‘difficult’ people my blood pressure goes up compared to when with nice people. I am currently reading Sapolsky’s book, Behave.
In fact when mentioning these issues to people I always explain ‘more cortisol’ when I say stress.
Robert, this is pretty much expected normal behaviour of the human nervous system- via mirror neurones and integrating areas in the brain like the insula we assess the other person’s stress state and mirror it to some extent. This is important to do- as a stress state in the other may hide an intention to make a sudden attack.
A lovely, if weighty, tome for someone you care about this Christmas. What an excellent man.
A great CVD-input as ever!
Complex indeed!
Now spending a couple of days with an old friend of mine at a relaxing spa hotel I am still offset from normal habits. E.g. there is a four course dinner every night (and I am also cheating on carbs) and I have great difficulties going to sleep and for sure I am in a strained state. I can “feel” the cortisol on high.
But were is the stressor? It must be a cause and actually the same thing happens every time I have a big meal late in the evening.
Food as stressor?
A possible stress, contributing to strain on the HPA-axis? If this is the case, it is not surprising that food can be perceived as an important factor in dis-ease.
Yes, and in particular biochemically ‘altered’ food such as grains and those with large glucose containing volumes, that act like hormones when absorbed.
They do say breakfast like a king but dine like a pauper.Try it for your indigestion.
or the intermittent fasting folks say skip breakfast.
I just break my fast later in the day after noon when I am intermittently fasting – I therefore do not skip breakfast!
Frederica Huxley: Me, too. Since I eat twice a day, the first meal is breakfast and the second is supper. I chew them well and thoroughly enjoy them!
I have recently discovered meals after about 4pm especially of high protein causes disturbed and shortened sleep. Smaller late snack higher fat causes far less sleep disruption.
Is this from personal experience, or from an external information source? Over a number of years, I have attempted to follow ayurveda guidlines for diet and daily routine. It is advised that digestion is strongest at noon, which is when the main meal of the day and heavier foods should be consumed.
Goran, it sounds like your inner struggle with saying “no” may be part of your stress as well as giving in to consuming the food you know is not good for you. A struggle/stressor I also share when eating at the homes of generous friends…
Vitamin D, Deep sleep & Gut Bacteria w/ Dr. Stasha Gominak
This is a beautiful example of how we live in a world of plenty, yet it turns on us so that we overdo and suffer the consequences. I think we have genes that encourage us to take advantage of plentiful food for the times when there is none. Only, those times don’t come, thankfully, so we may need to incorporate them into our day by spending time away from food, especially when we have indulged heartily. It seems to me we are built to stuff ourselves, but not everyday. We are built for moving around and lifting things everyday. I don’t, for the life of me, understand why some of us can’t get it right. We’ll have to keep trying.
Goran, the benefits of Intermittent fasting has been discussed here a few times..But ( infrequent) intermittent feasting also has it’s benefits. I hope you enjoy spa holiday from clearing the snow and splitting the firewood.
🙂
Goran,
Perhaps if you become convinced you need a very special diet, eating otherwise is in fact stressful!
Or: Stress of being away from those normal routines which you see as your salvation. Guilt over cheating is stressful, no matter what the cheat.
Let’s take a vacation from food in 43.
@ Goran: You’re at a spa and you’re over-stressed?? Goodness sakes. You ask “where is the stressor”? You are doing this to yourself, sir. You have yourself so guilt-ridden from having a few carbs (you actually called it “cheating”) it’s no wonder you’re having trouble sleeping.
People obsess about food. No, make that OVER obsess about food. Eating healthy is and has always been a hit or miss thing, and we all should always keep in mind that not everyone is the same, not everyone responds the same to foods, and certainly people get themselves into a tizzy by trying to be “the perfect eater”.
Relax on your spa vacation. The worrying will always be there waiting for you, but you certainly shouldn’t carry it around wherever you go.
Thank you for all comments!
It is complex, isn’t it?
This last night at the spa hotel I had a very restful sleep.
Could it have been that I and my friend (who had lost 10 kg in two month on strict LCHF) successfully converted our waiter to go and buy a book about what we are up to? Or could it have been the last Ardbeg shot we shared before saying good night? Or could it have been (God forgive me!) that I now resisted all carb temptations.
Avoiding anything which appears a strain seems the first action. Second is avoid seeing doctors for anything except broken limbs.
Of course, what appears to be strain might not be. I would imagine someone watching me lift weights would think I was in immense discomfort for most of it. However, I love it and would do it daily if my joints would allow. It is likely that my body is releasing cannabinoids in response to the strain, which makes me feel relaxed and focused.
In a related theme, I’d heard a sociologist on NPR the other day discussing the jump scare in horror films. She noted that when we anticipate a fright, our body preemptively releases endorphins (or cannabinoids) in response to anticipated pain. She hypothesized that this was why we enjoyed being frightened in films. One could surmise that the control over the stimulus (one could turn off the TV and thus exert control over the stress) is what makes it pleasurable (as opposed to being chased by a tiger).
Equally it may be that exposure to apparently threatening stimuli that do not present a life threat helps to tone up the autonomic nervous system, like a cold shower.
I guess I find it peculiar that some people are still skeptical about the role of stress in CVD and other diseases. It would seem a slam-dunk to recognize that stress can increase one’s chances for CVD, and also for cognitive issues, allergies, various autoimmune conditions, cancer, etc. As time goes on, more and more researchers are examining the role of stress in the medical conditions they study, and, in every case I have read, they find stress is a risk factor. I’m currently reading Dr. Amen’s “Memory Rescue”, wherein he indicates that stress increases one’s chances of developing Alzheimer’s or other severe cognitive disorder by 200%. Any condition that plays havoc with the body’s basic metabolic processes ends up weakening the immune system and other systems, so that disease is to be expected. It is logical, it is supported by the data, and we have at least a working understanding of the physiologic mechanisms by which it works. And, like diet, stress — or our response to it — is a risk factor over which we can exert a great deal of control.
Beware of Amen. I agree with the notion that stress might increase one’s chances of encountering many forms of body and brain degradation, but his work falls firmly in the quackery realm. Using SPECT scans to detect all kinds of mental illness is a scam – both dangerous (in the unnecessary exposure to radiation) and not sensitive enough to detect what he claims the scans detect. I had a kid come in a few years ago who had gone through the scan, and the Amen psychiatrist had diagnosed “fire” ADHD. Er, what? It took me about 5 minutes playing and chatting with the young fellow to know that he fell on the Autism spectrum. No radiation necessary. Of course, I don’t own a mansion overlooking the Pacific Ocean, so maybe I’m not doing this right.
See – https://www.salon.com/2008/05/12/daniel_amen/
You are correct in your assumption of Amen. Had to laugh at the last sentence in your post – we must all be doing something wrong (i.e., not lying to the public for cash!) or we’d all be living in mansions.
Interesting article. I recall in one episode of “Doctor in the House”, Dr Rangan Chatterjee giving a patient a saliva cortisol testing kit to use at home throughout the day. They don’t seem to be very expensive, so I would have thought it would be something that the NHS could provide via a GP and would give so much more useful information regarding a person’s state of health than the early morning test? Btw, I’m glad that you’ve stopped using Roman numerals!! Once they get into larger numbers it becomes a little confusing (for me, anyway!)
Just had another thought – it seems that a magnesium deficiency can cause people to react more to stressors and from what I read, a large majority of people are suffering from such a deficiency as it’s less available in our modern diet due to intensive farming methods. The usual NHS test for magnesium is a blood serum test which tells you diddly-squat because the blood levels are maintained by robbing magnesium from the body’s stores. So if you actually have a magnesium deficiency show up in a blood test, you’d be seriously deficient.
The other thing about magnesium is that ‘stress’ or ‘strain’ or whatever you call it (obviously different for each of us) ‘uses up’ the body’s magnesium, creating more of a need for it and potentially contributing to the deficiency that might already be present.
I often wonder if, because we are all likely to have some deficiency, whether our teenagers are suffering from more ‘psychiatric’ disorders as a result of this, that they are not able to cope as well as they might with things that to us seem trivial.
Finally, we are told that most people in the developed world are also suffering from a vitamin D deficiency – this in itself could be a result of magnesium deficiency as without adequate magnesium, the body doesn’t correctly utilise whatever vitamin (“hormone”) D it has available.
I live in Queensland, the sunshine state. A doctor commented that he was surprised that so many of his patients were Vit D deficient. We have been told to lower our cholesterol, stay out of the sun and eat a low fat diet.
Jillm: I tend to do the opposite of what the government/medical industry promotes, so I’ve raised my cholesterol, bask in the sun, and eat plenty of fat. Works for me! Lots of sun here in California, too, but I don’t much like winter any more. I’m envious that you’re in summer!
Jillm, the man (doctor) is an idiot… and a blind one at that!
Jillm & gary, I think it unfair that Qld has badged itself the ‘Sunshine state” when you nearly always get loads of cloud and rain during Summer… Whereas here in dry desserty South Australia we get sunshine nearly all year. 🙂
But I agree entirely that Australia wide since the 1980’s the common message from the ‘experts’, has been stay out of the sun, lower cholesterol and eat low fats….Which I happily ignore completely by getting loads of sunlightm & lots of organic pastured butter. ( I counted 5 different types of organic butter the other day in a supermarket here not counting the one tainted with canola oil. Such a wonderful range of choice.
It also helps that I avoid statins !
What would you recommend on how to increase magnesium and VD
Mg and Vit D supplements, alter your diet to include (yet) more leafy greens.. mushrooms, sardines or Herring…, .and luxuriate in “Bath Salts” – after 10 to 15 minutes under the midday sun, sans excess clothes…
As James DownUnder says, using Epsom salts in the bath or Magnesium flakes would help your Mg status. Or applying magnesium oil to the skin – that way the body will absorb as much as is needed and will also help vitamin D status
biddy99: Epsom salt bath or foot soak. Doesn’t cost much. I also use a spray-on magnesium chloride brine and drink mineral water (Gerolsteiner has 100mg/L).
Its interesting you mentioned Magnesium.
Take a 45 year old patient who is complaining of heart palpitations, goes to the docs, gets an ECG and they realise he is in Atrial Fibrillation. Get prescribed some Warfarin before a couple of attempted Cardio Versions which dont work, Gets a blood test for Serum Mg, everything is fine says the doc, just one of those things. 5 years later watches the widow maker, gets a CAC scan. Horror – 180, arteries of an 80 year old. Does a lot more reading, orders a RBC Magnesium test from the docs, Magnesium very low, now we have a root cause – The Mg deficiency drove the AF, the Warfarin blocked Vitamin K which with the low MG meant the calcium in the blood got stuffed into the Arteries – no amount of Vitamin D will help here as the mechanisms cant work as they should.
The only solution is to swap warfarin for Rivaroxaban, Supplement with K2 MK7 and Mg and repeat the CAC in 2 years.. Just a thought, I’m not a Doc.
I think I’d rather see you Mike than a GP who has no nutritional training!!
Taking zinc (up to 50 mg daily) with your mag supplement is also very good to help with blood pressure control, or so I read. I’ve just started doing this myself, so cannot attest to its veracity yet. I also have been taking a supplement of potassium with added magnesium for several years and I do a lot of foot soaks with the epsom salts or the magnesium chloride flakes. I love foot soaks! The K2 (MK7) is basically to help the D3 with bone structure and to get the calcium into the bones and not into the arteries. That’s how I understand it, anyhow.
I’m also a big fan of mag oil (which is not an “oily” oil, BTW) and mag oil lotion, too. At least it doesn’t mess with my GI tract and send me scooting for the biffy!
sundancer55: I find it hilarious that Mg has this effect! On my hikes I drink mineral water containing about 100mg, and always have to hit the throne at the end; once I had to make like a bear.
@ Gary Ogden: It’s not so hilarious when you are out in public and it “hits you”! I would imagine lots of people have had to make like a bear if they’re not near a toiddy. Heh!
I don’t take all that many supplements (try to eat well) but a few just have to be gotten through supps because there’s not enough food consumption that would cover a daily dose needed.
Haven’t seen you over at Gumpert’s blog for a while – where ya been? Things got a little hairy over there for a while when politics would enter the discussion, but there hasn’t been much of that lately. It comes up from time to time but I usually ignore it if possible.
Keep up the foot soaks and you can avoid the “bear in the woods” scenario. 🙂
sundancer55: I do, too (ignore the politics). The past election season was so ugly. I simply haven’t the time or interest to make comments routinely on more than two blogs, although I appreciate what he is doing, and have both of his books. He is one of those suffering cognitive dissonance.
What can be more relevant to optimal health–too much of one thing or too little of another? Mg has been written about as a culprit in multiple diseases, including diabetes as It is an essential component in B-cells of pancreas and the insulin molecule. Maybe too simplistic a link?
What of folk who deliberately eschew certain food groups–like vegetarians, vegans and grain haters?
@ Donald Scott: I try not to be restrictive in my diet too much. Actually, if a person is going to be restrictive to any degree they should follow the intermittent fasting (I do the 14-16 hour one about 3 times weekly) but I think all types of foods are healthy if you eat them in a healthful way. I have a friend who thinks “candied carrots” are healthy (they are made with lots of brown sugar) just because they’re carrots. Personally I just steam them, put a little butter and S&P on them and maybe a little parsley. That’s the difference, IMPHO. Ditto for all the food groups. There are both healthy ways to eat things and junky ways to eat things. People have to pick whatever works for them, I guess. I don’t eat paleo or whatever it’s called by now, because they eliminate important dairy and whole grains,. ANd I will simply never understand people who choose to eat complete vegetarian or vegan diets because they are missing out on more than they know. BUt, to each his own,.
How do we embrace a relaxed lifestyle in this, fast and sometimes aggressive society.
Can we compare it to times past, before family planning, before a five day week, before busy motorways, endless other things that contribute to raised cortisol and metabolic syndrome.
Of course I should not wish to live as we did then, but I was born 1940 and a strong loving family and good neighbours gave us wonderful support, community. Young people adapt to a very different way, but the needs of a person are still to love and be loved surely.
Super post Dr Kendrick, you make it easy for us ordinary mortals to understand. Thank you.
Another excellent read, providing a check list of things to look out for.
Cortisol is the key hormone – any others?
I ask because I did a saliva cortisol test a few weeks back (4 samples during the day) and came back normal. And yet, self diagnosing as we all do for stress/anxiety/depression, things are not right.
Would a cortisol test be the same as any other blood test, or blood pressure check – just a snapshot in time with the need for regular checking/testing to build up a more complete and accurate picture?
Perhaps the regular cortisol testers can comment?
@Charles Gale
Having a result from any test – blood, saliva or anything else – which comes back as being within the reference range isn’t sufficient to say that it is “optimal”, although doctors will tell you that the result is “normal”.
In some cases doctors will say that a result is “normal” if it is outside the reference range but they consider it to be “close enough”. For example, get a ferritin (iron stores) result with a reference range of 13 – 150, and patients are frequently told that a result of 4 or 5 is “normal”. After all, 4 isn’t much smaller than 13, so of course it must be normal!
For saliva cortisol testing where the patient provides 4 cortisol samples throughout the day, a suggested optimal set of results is described in “Example 1” on this page :
http://www.rt3-adrenals.org/cortisol_testing.html
I don’t like Americanisms much but the words : Very Insightful describe it so well. Can’t wait for No 43.
Dr. Kendrick, thanks for this post..As always well written and cogent That is it makes sense and I want you to be right about this !
But there may be a paradox which tests your proposition. In the previous blog Smartersig and I have been beating each other up about how CVD dropped significantly in Norway during WW2. and whether iit was diet caused or not, and if so, what kind of diet. But that is not what is interesting to me.
I am interested in the simple equation that war usually means loads more stress and thus more cortisol etc etc.. = a n increase in the CVD rate.
But during WW2 in Norway, there was no increase CVD. In fact CVD dropped. How can this be explained ?
Suicides fall during war time as well. In the UK CVD dropped shortly after the war started, and before rationing started. Then it went up. I think there are many things going on in war, tricky to disentangle them all.
CVD and Diabetes fell dramatically due to the rationing. Interestingly enough, diabetics were substituted sugar rations for butter during WW1 and WW2. Rationing = Reduced Calories or Missed meals = Intermittent Fasting. I guess there was a greater sense of sticking together and being there for each other during war times.
Mike there is now a whole swag if folks who do intermittent fasting….I do myself : once a week I don’t eat any food for a day…It certainly helped me lose weight this year…
I’ve also wondered why CVD rates dropped during WWII. Possibly because there is more social cohesion and support — people standing together against a common enemy, their differences forgotten.
During the 2010 World Cup in South Africa there was a tremendous spirit. People smiling, waving flags, blowing vuvuzelas, being nice to each other. Now that it’s over we are back to the usual interracial sniping and bad-mouthing. I don’t know what the heart attack rates were, but I predict they went down during the World Cup because of the friendlier atmosphere..
Makes complete sense. Can’t wait for the follow up, but you must have been writing this over Christmas, Dr K – you need some relaxing time! Very best wishes for 2018, your new book, and the continuation of this blog.
Book finished, next book started. Blogs will continue.
What is your new book about, and does it have a title yet?
Enjoy learning more, thanks from a novice.
Are you referring to Hans Selye?
Did I spell it wrong?
I presumed it was this person you were referring to?
https://en.wikipedia.org/wiki/Hans_Selye
Hans Selye is correct sp
I think stress is very important and very bad for you. I also think many of the differences between cultures and their heart disease rates are attributable to stress and not diet.
Having said that, I’ve lost 50+ pounds (about 25+ kg, no idea about stones 😉 mainly by eating fewer carbohydrates and adding intermittent fasting to that mix. No discernible change in stress, although I think going from a high carb diet to a low carb diet affects stress. For instance, on a high carb diet, it was a wild ride. I would eat, get a “high” and then crash and have to eat again. I also was depressed and angry. Now on a low to zero carb diet, I am never depressed. I don’t get sleepy during the day, my moods are the same at all times (whereas I had massive mood swings on high carb), etc. I am much more mellow now.
So, while I think that stress is incredibly important, diet can help with stress. Which one is more important? To me, I take steps to reduce stress in my life, but changing to a low carb diet has been a Godsend in terms of (1) reducing stress naturally and (2) gaining the ability to help with stress reduction.
One additional item that I think helps with stress is exercise. I still exercise two days per week (have exercised my entire life, even while gaining weight on a high carb diet), and this helps with stress reduction. I find lifting weights is better in this regard than is aerobics, as when I lift, I exercise the entire body. For most aerobics, this isn’t the case. I also find I can lift weights for 20 minutes and get a massive stress reduction, whereas with aerobics (say, cycling) it takes at least an hour to get the same reduction.
BobM I have always wondered why a diet with close to zero carbs doesn’t put the body into a stressed state. I would have thought cortisol would be released to assist in activating gluconeogenesis in the liver. After all, your body really doesn’t want to be hypoglycemic. I also wonder whether there would be any glycogen storage given that glycogen breakdown is triggered by both glucagon and cortisol which would both be elevated on a zero carb diet. How does the burden of constant gluconeogenesis affect the liver longer term? I have said it before but perhaps cortisol is a bigger problem than insulin with respect to blood glucose control or lack thereof.
Absolutely fascinating!
This is certainly a cliffhanger while we wait to see how to get rid of the underlying cause that leads to heart disease. While I explore various diet and lifestyle interventions (my hobby!) I am constantly disappointed in all of them and come back to what do I want to eat or how do I want to move my body today to feel alive and healthy. Above all, it comes down to what will allow me to feel calm and secure (in this crazy, confusing world). Why can’t I remember that? I keep exploring diets like that will save me. It hasn’t so far. Well, I mean, I am still alive, but food is just food and can only do so much. What you are explaining is so far beyond what food can do. Let’s hope people will listen and understand and stop worrying about stupid stuff (primarily me). Thanks Doc! I appreciate your work. I may move to Scotland!
Carolyn Trammel: One of the things I do which brings calmness and happiness is to plan in advance all the activities I wish to accomplish the following day before I sleep. I always wake up looking forward to my day.
All of philosophy can be summed up in two words — “shit happens”.
Or, to put it a little more poetically — “Into each life a little rain must fall.”
I’ve had a stressful couple of days. My card was declined in a busy upmarket supermarket, despite having ample funds. It’s very embarrassing. Everyone stares at you while they call the supervisor, and the staff treat you like a simpleton as they ask if you’re SURE you put your pin in correctly; are you SURE it’s a cheque account not a savings account? I took the card to my bank. They say there’s nothing wrong with it.
Next day (yesterday) my cell phone was snatched out of my pocket as I was walking home from the local shops. I offered to buy it back from the thief then and there, and ended up losing the phone and the money. It was a young woman thief, too. At 69 years old and 5’2″ tall I’m no match for these young kids. I blocked the number within minutes, and reported the theft to the cops. They told me they could do nothing without a reference number from Vodacom. The Vodacom website said they could not issue a reference number without a case number from the cops. Catch 22!
Eventually I found another website that explained the proper procedure and the phone is now blacklisted. I have a borrowed phone temporarily. My card seems to be working again. And I’m pretty calm, considering. Because I accept that these things happen. The Bad Luck fairy flies around invisibly and sometimes needs to take a rest, and if she sat on your shoulder and not the other guy’s, it’s because you were there and he wasn’t. Not because of any malice towards you from the universe.
“Into each life a little rain must fall.”
If you can accept that, and bear your share of the bad luck that floats around without complaining, you are well on the way to finding peace and tranquility.
Martin
I find that sort of thing is stressful. Well done if you have got over it.
Martin Back, “shit happens” is much clearer than stress/strain. Since all medical conditions are expressed in greek, suggest that the stress/strain hypothesis of CVD be renamed the “KAKA hypothesis”. The word “pollution” could be substituted for “KAKA” for people not familiar with medical terms. Applying this reasoning, a unified theory of disease can be developed. Source of all diseases is caused by either:
1. polluted air- get a hepa air filter for indoors
2. polluted water- drinking water can be recycled sewage with added chlorine, use a water filter
3. polluted food- avoid the bad stuff such as GMO’s, seed oils, wheat, sugar etc.
4. polluter ether- electromagnetic radiation from cell phones etc.
5. polluted thoughts- negative experiences/thinking can rewire the brain
6. inactivity- need to keep the lymph circulating
7. doctors- ?
Especially enjoying the stress.org website. (mentioned in references). Regarding meditation as a way of dealing with stress/strain, I am becoming even more confused by the minute! After my own cardiac arrest/stenting, I was discharged with the “magic bullet” Atorvastin(discarded after 7 weeks, and that was 3 years ago!)). However confusingly, on being discharged, the package I received also included a manual almost two inches thick entitled “The Heart Manual, Post Myocardial Infarction Edition”, together with a comprehensive CD of relaxation techniques! Perhaps this was them hedging their bets? Joking aside, I have to say the CD was actually amazing, in that I NEVER once got to the end of it without falling asleep! I think that meant it worked! lol p.s. I still use it occasionally, but probably not enough!
I completely agree that strain is the likely the root cause of CVD and a host of other mental and physical diseases. I can see it today in the rapidly increased suicide rates among teens that I believe is attributable to the rise of social media and the false expectations these applications raise in their minds of the need to be as pretty/handsome/socially accepted as they see others portraying themselves. In adults, it is the failure to achieve “the good life” in terms of the consumption driven expectations of society. In other words, the pathogens causing these diseases are memes, not viruses.
Looking forward to your views on the treatment in your next post. For me, I have found the study and application of Stoicism to be highly effective. “If you are distressed by anything external, the pain is not due to the thing itself, but to your estimate of it; and this you have the power to revoke at any moment.” ― Marcus Aurelius, Meditations.
Michael: I agree. A good, healthful practice. Recommended reading: “A Guide to the Good Life {the ancient art of stoic joy} by William B. Irvine. Heard him interviewed in 2011, bought the book and read it on the plane-very peaceful flight!
Gary thanks for this comment. I looked at Irvine’s book on Stoicism via Amazon & read a few pages at random by looking inside. I really like the plain sense & wisdom in it. So I will get it. The Serenity Prayer was, when I was ‘religiously inclined’ an inspiration in daily life. But even now when I am no longer ‘religiously inclined’, the fundamental insight in it is still true.
Gary – I agree, “the Good Life” book is an excellent introduction and one I recommend to people who are looking for an good introduction into what Stoicism is all about. The fact that the leading psychological therapy, CBT or Cognitive Behavioral Therapy, grew from the principles of Stoicism demonstrates is enduring relevance. Another book that I recommend as a good modern introduction is “The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good Life” by Mark Manson. Mark blogs as well with a funny, Stoic slant that makes great reading. Finally, for those who want to dive into the source materials, any of the Letters by Seneca (the Roman Senator and tutor to Nero) are still surprisingly relevant to modern times and issues – you will be surprised on how relevant as you read them.
I think you mean Hans Selye (pronounced ‘sell-yay’).
Yes, I knew of Hans Selye back in the sixties, when my father, a physician who was investigating the stress disorders rampant among air traffic controllers in the Chicago area at the time, referred to his work in depth.
Splendid post as usual Dr Kendrick: it goes a long way to explaining the ‘French paradox’.
Interesting account of the warring couple whose outwards appearance is so different. It brings to mind the wonderful old Indian proverb: “Never judge a man until you have walked a mile in his moccasins.”
Interesting. I think we are dealing with two separate failures of the body’s control systems:
– A failure of the appetite control system, leading to eating too much, and eating junk.
– A failure of the stress control system, leading to perverse stress and chronic stress.
By “perverse stress” I mean stress which causes the sufferer to seek more stress, just like the overweight person seeks more food, or the drunk person more alcohol. For instance, abused people who go back to their partners time and again. Soldiers who repeatedly volunteer for dangerous missions.
We all need to feel hunger and fear. They are important for survival. But they are needed only up to a point. In a healthy person you expect hunger -> eat -> hunger gone; fear -> run away -> fear gone. (Or any other stress which can be relieved by taking action.)
There’s some sort of addiction mechanism at work here causing a dysfunctional response, but what it is exactly I don’t know.
Very good
So, 44 will address ridding oneself of the underlying cause. Is that another way of saying you will address the resuscitation of a “burnt-out HPA-axis”? Burnt-out sounds so final. I’m guessing that most of us are here because we’re burnt.
I wonder if Transcendental Meditation has any part to play in this.
Meditation helps, but you have to do a lot to get a lasting and substantial result. For most of us, retiring to a monastary for 3 years is impractical. My Tai Chi teacher tells me that is what is required to correct the problems in people as debilitated as Westerners usually are.
Thank you, Dr. K. I’m just wondering how harmful a steroid inhaler in a twice daily dose is. One could find oneself between a rock and a hard place.
By the way, how on Earth do you find the time to do this? Tell us your secret, please. I am mystified and full of admiration.
Inhalers are not a problem, the dose is not high enough. Oral steroids are the problem
Thank you. Kind.
This is reassuring.. esp. coming from you! Best wishes for 2018! Thank you for all that you do.
Of the many stressors causing strain I wonder the role of chronic energy overload and the resultant adipose hypertrophy and potential strain associated with such?
You mean eating too much and getting fat?
Might be of interest – it’s a pdf.
http://www.dtic.mil/cgi-bin/GetTRDoc?AD=ADA564611
FTL: This study demonstrates a significant relationship between attachment style and PTSD symptoms within a military population, potentially providing the basis for future research in this area.
Thanks, Malcolm. I enjoy reading your blog, and your arguments in this post seem solid. But is this hypothesis of stress/strain compatible with the declining rates of CVD in the western world?
JP Patten – burnt out HPA axis and Anglosvizzera (saliva cortisol kits)
I’ve seen an endrocrinologist here in England (armed with Zapolsky’s Zebra book and Bjorntorp’s work) and asked this very question. Did it recover? She wasn’t interested, didn’t have time to read and vaguely said it did. And, sadly and predictably, then she dragged the consultation back to high LDL high cholesterol and statins.
Maybe this will be addressed next blog – how does it recover? How quickly? Once the stressors are removed?
Anglosvizzera – cortisol testing kits provided by NHS via GP.
Nice thought. But…in our dreams. After my CVD incident, and settling on stress/strain as a strong contender, it was like getting blood out of a stone for the normal morning test, ditto for the one with the tablet. My GP didn’t want to know or waste his time about 24 hours cortisol testing. Now, he said, about your high LDL cholesterol and statins.
I paid for it myself. Not too expensive either.
I won’t rant and rave about how they find the money for e.g. gastric band surgery, health tourism, self inflicted problems such as drugs and drink…ooops, I just have.
Several weeks ago you mentioned you were attending a conference on an ‘alternative way of looking at cancer’. My guess is that this conference probably refuted 70 years of medical dogma that holds that cancer is a genetic disease, i.e. the somatic mutation theory (SMT). Following the abject failure of the multi-billion dollar funded cancer genome atlas (TGCA) project, evidence seems to be pointing towards the primary cause of cancer being ‘metabolic’, I.e. Injury to the mitochondria and the subsequent activation of (I think) heptokinase II. Do you subscribe to the latter view as originally put forward by Otto Warburg? Or are you are you a traditionalist in this sense?
Many thanks for this, after a much abused childhood, I have always loved on a hair trigger, had a major stroke. Just over a year ago, still fighting back from it. Good to have some sort of insight into possible reasons Best wishes Edith Holmes ________________________________
Well. The next blog should be worth its weight in laxors. Who care about gold? ( I did mention quite awhile back that the ANS is thought by some “advanced” thinkers to be the source of CVD. You seem to be coming closer to this thought?)
Dr K, what is the effect of “strain” (as you define it) on thyroid dysfunction?
Complex, but there is a strong relationship, in both direction.
I read all the posts and comments with great interestI am a very interested layman. Aged 51 I had a heart attack out of the blue. Fit, healthy and interested in diet. Resolved with 2 stents. Fast forward 8 years, another stent fitted. Consultant’s view, “some people just fur up”!! Have since taken control, started LCHF and stopped statins. My history is of acute stress over a long period of time. I still worry that another intervention will be necessary, so I realise that the ‘stress loop’ could become a self-fulfilling prophecy. I await Malcolm’s next post with great interest!
I guess that there are stress hormons among all the other hormons and now I have another take on this when reading a scary book (I shouldn’t really read this kind of books though, since by definition they are stressing) about how chemicals in our environment interact with our hormon receptors.
The book is “The MYTHS of SAFE PESTICIDES” by André Leu. As the title indicates it is the modern agriculture and the pesticides which is causing havoc and especially among our hormons and in the long run starting with the development in the fetuses and with devastating effects that are often epigenetic. And Leu knows what he is talking about. Autism i just one of “modern diseases” which “coincides” with the introduction of the dramatic increase of pesticide use by 1995.
There are many people out there in the world who enjoy a good adrenaline “rush”. They go sky-diving, bungee-jumping, attend movies featuring clowns and other King stories. They’re generally younger. They generally get addicted and “need” further stimulus. What damage (strain!) are they doing themselves with all this fun artificial stress?
I, myself, have given up TV and most movies.
For entertainment, I content myself with an occasional nice relaxing murder mystery novel. Though, I must admit, the better ones can get my heart beating too hard as the climactic scene approaches.
Stress is everywhere! Even intentionally self-administered doses.
Does the “intention” make a difference to the strain outcome?
JD
My belief is that most kids are very keen on “excitements” but on “the safe side” and that there is nothing negative involved here – it is all about playing which is important for the mental development of any child.
However, as Leu convincingly elaborates on, irreversibel damages on the central nervous system (CNS) are invoked by the hormonal mimicking chemicals of the pesticides which are close to nerve gases in terms of origin and chemistry. So there is definitely a scare “logic” involved.
In fetuses and in infants the CNS is under physiological rapid development and is then very sensitive to disturbances of many kinds.
My own CNS is hopefully pretty much set at 70 + and as you I now enjoy more relaxing “excitements” as e.g. on this blog or reading one of my books.
I used to know Andre Leu years ago here in Oz. He is an organic tropical fruit farmer up in Qld. Bright bloke and a good grower ! But I have not seen that book. Maybe it was published under another name here.
By the way Goran there were many very dangerous pesticides used from the 1960’s onwards. Mostly organo-chlorines and organo-phoshates – Very very dangerous and persistent like DDT
Bill,
Small world?
The book is easy to get hold of and really worth reading.
HB – thanks for the cortisol test result link.
Normal vs optimal – I had this issue with a homocysteine test result where there appears to be no real consensus as to what it should be. On the one hand, it fell within Kilmer McCully’s normal range for a middle aged man but on the other hand was that desirable?
Looking forward to your next posting. “Next blog. How to get rid of the underlying cause?”
Is it possible that Mental Stress is one form of strain and Physical Stress say due to ill health, Sugar, Alcohol, Over feeding is the other
Strain can be caused by both physical and psychological stressors
I will reply in more detail later- but I would suggest that the physical stressors cause the alcohol, over feeding ill health.
Thanks!
Many thanks for your continued wisdom. Best wish we for 2018.John Studzinski
Sent from a Samsung Galaxy C9 Pro smartphone.
When you’re glycine deficient you can suffer inflammation from any tissue injury, even micro injuries such as what occurs all the of the time in arteries. Glycine is known to be protective of such injuries and may help prevent heart disease. https://www.theguthealthprotocol.com/wp/glycine-the-most-important-inflammation-regulator/
Randall,
I am puzzled as to how anyone becomes glycine deficient, unless they live on a low protein diet. Gycine is the simplest amino acid and is a common constituent of many proteins:
http://www.tiem.utk.edu/~gross/bioed/webmodules/aminoacid.htm
David Bailey: The way I learned it (through WAPF) is that this is possible in those who eat the government way: skinless, boneless chicken breast, for example, since skin, bone, and cartilage contain a higher proportion of glycine than muscle meat. This would also apply to smartersig’s squirrels, since their skin is obviously inedible.
Dire warning about squirrels!
This bit about dining on squirrel is irrelevant humor, right? Then, nevermind.
If not, and in any case, steer clear of our beautiful little native flying squirrel. It’s the only known living continuous vector for Epidemic Typhus. Typhus can kill. It will certainly at the least make you horrifically ill if you get near enough to an infected squirrel.
You will be ok with good nutrition, and sufficient vitamins, it’s not necessary to eat them though, there are plenty of greys around, and they only carry a pox.
Sorry AH. I’m at a loss.
Who is “you”?
Not necessary to eat…flyers?
What “pox”, and which are you suggesting carries it?
In case anyone is concerned that this might be a jokey off-topic distraction, I’d like to make this clear:
The feces of the parasites of certain populations of American flying squirrels contain spores of Rickettsia prowazikii, the bacterium causing epidemic typhus.
The dry airborne feces might be breathed in or blinked in. Proximity to the squirrel or nest will do it. Eating the squirrel is not required.
The bit relevant to our blog: ENDOTHELIAL CELL DEATH.
The bacteria proliferate and directly attack and destroy the endothelial cells of any/all of the smaller vessels in your body. All bodily systems supplied by those vessels suffer, eventually shutting down and dying if no intervening immune system or antibiotic overwhelms the invaders.
Get the implications? Shall I go on?
JDP, there are no flying squirrels here in Oz. But there has been typhus occasionally. ( Normally via infection from introduced animals. ) However CVD rates seem similar to elsewhere in the western world.
JDPatten: How common is this? What is the range of the American flying squirrel? We don’t have them at all in the West. What we do have are introduced European red squirrels, which are terrible garden marauders and pests. I wish smartersig would come and capture them all.
Gary, while smartersig is over catching the red squirrels, would you or a compatriate like to come over th the UK and shoot all the north American grey squirrels? They are terrible garden mauraders and pests, and steal birds eggs to boot.
JDPatten: Out of curiosity I did a bit of sleuthing, and reached the MMWR of October 22, 1982. Epidemic typhus is now considered a rare disease (30 cases from 1976-1982, in widely scattered locations, no deaths). Most of the cases were in the South, one in California, and 17 associated with Glaucomys volans, the Southern flying squirrel, although they stress that body lice are the main carrier of Rickettsia prowazekii. Interestingly, just last August a new species was described (Journal of Mammology), living in Oregon and California: G. oregonensis, once considered belonging to G. sabrinus, the Northern flying squirrel (these are negative for antibodies to Rickettsia). I take back my comment that they don’t occur in the West. They sure do! I won’t worry about them, though, although the untreated disease sounds really nasty for cardiac health.
Gary, et al,
“Flyers” occupy the same mixed hardwood/conifer forests as greys and reds in most of the Eastern states. Flyers are shy, though. Rarely seen.
Typhus from flyers IS comparatively rare. About a half-dozen a year in he U S, as I recall.
You just DO NOT want to be the rarity!
Available statistics put the death rate at between 10% and 40%. The elderly (whoever that might be!?) come out at up to 60%. Flyer strains do seem to be less virulent. ‘Course, it all depends on your own particular vulnerability as well as the virulence of the R. provazekii strain.
And: The disease is virtually unknown to generalists in modern medicine. Only the CDC has the capacity to diagnose. How many deaths documented as due to “fever of unknown cause” can actually be laid at the four feet of the little squirrel?
And, and: How many subsequent CVD deaths can be laid at their feet? I’m currently trying to find if there’s a relationship between typhus and high CAC scores. There’s little interest in such an “antique” disease, so very little info seems to be available.
This is what the CDC has to say:
https://www.cdc.gov/typhus/epidemic/index.html
I stand by the CDC in this matter, as far as it goes.
Think again if you believe a good immune system will protect you. The bacteria, challenged by a good immune system will sporify, hiding under your skin… and wait.
You will get it again… unless treated in a timely fashion with Modern Pharma’s doxycycline.
This is me:
As the subject of this paper, I’m in a position to stand by all that is said here as well.
https://academic.oup.com/cid/article/51/6/712/460729
OK. That’s enough from me on this. Just had to vent to keep the stress from turning bad.
DHEA supplementation enhanced anabolic balance throughout sustained military stress—–
Effects of dehydroepiandrosterone supplementation during stressful military training: a randomized, controlled, double-blind field study.
Taylor MK1, Padilla GA, Stanfill KE, Markham AE, Khosravi JY, Ward MD, Koehler MM.
Author information
Abstract
Dehydroepiandrosterone (DHEA) and DHEA sulfate (DHEAS) are anabolic prehormones involved in the synthesis of testosterone. Both have been shown to exert neuroprotective effects during stress. In this randomized, controlled, double-blind field study, we examined the effects of a 12-day DHEA regimen on stress indices in military men undergoing survival training.
Forty-eight men were randomized to either a DHEA treatment group or placebo control group. The treatment group received 50 mg of oral DHEA supplementation daily for 5 days during classroom training followed by 7 days of 75 mg during stressful field operations. Control subjects received identical placebo pills.
Salivary assays (DHEA[S], testosterone, and cortisol) were conducted at four time points: distal pre-stress (T1), proximal pre-stress (T2), mock-captivity stress (T3), and 24 h recovery (T4). Subjective distress was also assessed at T1, T3, and T4. As expected, DHEA treatment resulted in higher salivary concentrations of DHEA and DHEAS during daily living, mock-captivity stress, and recovery. Similar patterns were observed for salivary markers of anabolic balance: DHEA/cortisol, DHEAS/cortisol, and testosterone/cortisol concentration ratios. Despite notable time effects, no group differences emerged for subjective distress.
A brief, low dose DHEA regimen yielded large increases in salivary DHEA(S) concentrations and enhanced anabolic balance throughout sustained military stress. These physiological changes did not extrapolate to subjective distress.
PMID: 21790446 DOI: 10.3109/10253890.2011.585189
Super interesting! I am learning so much, thank you!
HAPPY NEW YEAR MALCOLM!
Tom McMaster
Sent from my iPhone.
Nice little article about stress from Robert Burton MD some years ago:
https://www.salon.com/2000/03/20/stress/
Act more like a zebra and it won’t kill you.
You turn a corner and are accosted by a mugger. Your body responds with a “fight or flight” outpouring of adrenaline and cortisol (the naturally occurring cortisone secreted by the adrenal gland). You make it safely to your car, outrunning the overweight, out-of-shape mugger. If you were a zebra that had just outrun a lion, you would relax and return to daily zebra business, with no accompanying implications. And, if you were a zebra, your stress hormone levels would quickly return to normal.
16 years ago, at the Stress Research Unit at York University, England, psychologists began looking for the aspects of personality that might moderate the impact of stress. The most powerful predictor turned out to be the tendency to ruminate about emotional upset. This led them to redefine stress as precisely that: rumination about negative emotion.
Was reading an article about the perpetual economic tragedy that is West Virginia, when the author focused on cumulative stress responses to populations under duress for long periods. The article linked to this –
https://www.sciencedirect.com/topics/neuroscience/allostatic-load
FTL: “Besides fat deposition, there are other cumulative changes in other systems that can result from repeated stress, for example, neuronal remodeling or loss in hippocampus, atherosclerotic plaques, left ventricular hypertrophy of the heart, glycosylated hemoglobin and other proteins by advanced glycosylation end products as a measure of sustained hyperglycemia, high cholesterol with low high-density lipoprotein (HDL), increased oxidative stress, elevated proinflammatory mediators, and chronic pain and fatigue, for example, in arthritis or psoriasis, associated with imbalance of immune mediators.”
I went to your link and found the below:
Stress Reactivity and Disease Progression
Allostatic load has been defined as the price that the body has to pay for maintaining allostasis (stability through environmental change). Recently, it has been suggested that increased allostatic load, which may occur through the cumulative build-up of stress over a lifespan, may significantly hinder the functioning of different physiological systems…
Reactivity to stressors involves not only the initial response but also the system’s ability to reset itself after stress. Older organisms seem to reset themselves after a stressor less readily, leaving stress response systems more tonically upregulated for longer periods of time after cessation of the stressor. Cancer particularly affects older people, and chronic disease-related stressors are likely to further decrease the flexibility of stress response mechanisms.
============
I think a combination of both these paragraphs relate to my situation. I have actually had a huge number of stressful events over the course of my life, and I have also noted in myself and several other middle aged women a sense of not having the resilience to bounce back after stress that we did when younger.
That caught my eye too, Anna. I feel as if I have a trip switch, in that when stressors breech a certain threshold, I’m vulnerable to being in a (what feels to be perpetual) heightened state of anxiety. I’ve gotten better at downregulating via exercise, time with family, mindfulness and maybe a glass of wine, so I’ve generally kept in a reasonable balance, which means I have to be vigilant about not becoming hyper-vigilant.
I didn’t realize there were ever people who took seriously that pesticides or herbicides could be harmless.
AnnM: Only the EPA.
AnnaM. Well, what I didn’t know was the nonlinear effects of the pesticides on hormon receptors. I.e. at high doses no toxicity is detected while at 100 or even 1000 times lower concentrations there are obvious interferences. On top there are epigenetic expression effects lasting for generations after initial exposure.
In the ‘World News’ section of my newspaper today:
____
‘Black Lives Matter activist dies at 27’. The daughter of Eric Garner, the man whose death at the hands of New York police helped fuel the rise of the Black Lives Matter movement died yesterday of a heart attack. Erica Garner, 27, a mother of two, became a prominent activist after her father died in 2014 when a police officer put him in a choke hold while arresting hem for selling single cigarettes.
____
Happy New Year to one and all. Eat well, sleep well, play well and get on well with all those around (including on here). Don’t forget to sing when in the bath (or if you prefer a shower), be happy and keep smiling.
I wrote this message late last night. But in the comments of the previous blog which was not my intention. Lest some not see it I will double it up here.
“Here in South Oz it is now 1.49 am of first day of the New Year, 2018. Happy New Year to everyone here !!
We went down to Adelaide and danced tango with friends for hours, chatted, drank a nice glass of red etc. It was a relaxing lovely evening and I think my cortisol dropped and my stress levels as well.
In view of the fact that meditation, while being fit for the purpose of lowering stress, takes three years and also involves residing in a monastery for that time, I suggets that dance is far more easy, and fun. And for men such as myself, it also involves dancing with a whole variety of lovely women.”
Having done both meditation & tango, I know I prefer the latter.
🙂
Happy New Year Doctor Kendrick!
Happy New Year to all readers and commenters!
Martin Back
Thanks for finding and posting the Robert Burton stress article. It struck a chord with me: sent off to boarding school at age 8 at which point I developed both dandruff and dermatitis which continue to plague me to this day.
And having recently taken a solitary job (no colleagues…not as good as it sounds) and going home to an empty house just lends itself to rumination.
This is usually the point when people start to offer obvious solutions e.g. change your job as if conquering mental health problems was that simple.
From a biography of poet Edward Thomas, which also struck a chord:
“Thomas had been plagued by depression from before his university days at Oxford. There, he fought to shake it out of himself: he tried drink and opium, took up rowing and rowdiness, but could not hold the bleak moods black”.
Happy new year Dr. Kendrick
Finally I am beginning to appreciate the importance of stress. Thank you Dr. K.
A. STRESSORS :
1. Physical -injury/trauma
2. chemical- neurotoxins such as MSG, pesticides, herbicides, heavy metals (mercury), medications,
3. physiological- hypertension, inflammation (gut dysbiosis, leaky gut, bacterial/viral infections), hyperglycaemia, sleep depravation, nutrient deficiencies ( vitamins C, Mg, D3, gluten intolerance, lack of sunshine, inactivity
4. emotional- depression, aggression,
B. IMPORTANCE OF HYPOTHALAMUS:
– part of the brains (limbic system )
– master regulator of body temperature, blood volume, blood pressure appetite, libido etc.
gets information from hormones, serotonin, dopamine etc.
– analyzes immune system status (cytokines)
C. WHERE PROBLEM STARTS: disturbed pro-oxidant/antioxidant balance leading to,
oxidative and nitrosative stress affecting mitochondrial ATP production
D. HPA AXIS AND ADRENAL FATIGUE:
– abnormal daily free cortisol pattern
– low cortisol production by adrenal glands
– tumour necrosis factor alpha as result of macrophages and inflammation can bind to receptors on pituitary gland. Signal to adrenal glands to produce cortisol is blocked.
E. EFFECT OF STRESSORS ON BODY:
– neuronal remodelling in brain
– cellular malfunction
– basically cause of most diseases
Cognitive dissonance I’ve thinking a great deal about. The journey from belief to agnosticism has been, at times smooth and liberating, and at times has been vaguely unsettling, a feeling I don’t like one bit. The loss of religious belief was so gradual that it has never caused a problem, and in any case, I am profoundly grateful for the moral code that underpins my approach to all questions of how to live and interact with others, and which I learned in Sunday school. I still find learning about religion fascinating. And thanks to William B. Irvine’s book (which I am re-reading because I need to), I’ve learned a philosophy of life. The loss of trust in our political and public institutions and, to a large extent in medicine, began in 2011, and has been a bit rocky and liberating at the same time. Even in an inquiring mind the loss of certainty can be unsettling. So what role does cognitive dissonance play in cardiac risk? Happy new year all!
Let me encourage you a little. It’s only one more small step to entirely abandoning dependency on concepts and institutions that you cannot depend on. It’s their nature to be ephemeral. The notion of faith, to me, is an abomination. Find freedom in the self-assurance that — granted, with effort — you can discern things for yourself, that you can have a strong moral base without formulaic institutional admonitions, and that it’s the most natural adult human accomplishment.
Of course learn history. Religious history, if you must. Otherwise, you’re doomed to repeat it. 🙂
JDPatten: Thanks: Yes, I’ve reached that point already. I must, on the other hand, engage with the world, with other people, and how to do so without strain is what I’m attempting to learn. Thus William B. Irvine. My boom box died today rather suddenly after 20+ years of service, so I got a new one. Chopin, Dvorak, Mozart, Liszt, Bach (E. Power Biggs on the organ!), Beethoven, Prokofiev, Gershwin, ABBA, the Beatles, Alison Krause, The Dixie Chicks, John Phillip Sousa, etc. Heaven! I hope Jennifer comes back. Her voice is instructive and heartening.
Forgot Tchaikovsky. My bad!
Gary, JD
I am on your side although I never attended Sunday school 🙂
The feeling of being a part of, belonging to a society or a group is perhaps the most profound stress “reducer”. The fundamental purpose of religious practices of every kind that has followed mankind since the “beginning” is probably the feeling of wellbeing; sympathetic stress reduction. The opposite of being all on your own, without family or friends brings a “no good” feeling for sure.
When you acquiring “knowledge” you are on a dangerous path of excluding yourself from a community – the trauma of philosophizing too much. In paradise by God through the apple and by king Salomon through the books knowledge was definitely warned against.
Goran, another way of looking at the brain and how it functions is by using a computer analogy combined with evolution. In the beginning there was a reptilian brain with separate modules each responsible for processing a sensory input. All modules are separate but interconnected. Modules that are required for survival would be:
A- a module is required to integrate sensory inputs from internal organs and exert control over them to maintain homeostasis
B- a module to regulate appetite and digestion
C- a module to identify danger from other creatures, and respond by quickly putting animal in alert mode, hard wired instincts.
D- a module to sense safety when with mother or herd
E- a modul to return system to normal after full alert
The original module structures and functions are retained and refined as evolution progresses.
Humans (primates) have added a new module located in the prefrontal cortex (PFC) that is involved in personality expression, decision making, social behaviour, emotions, planning etc.. Coordination between modules is by neurones and signalling molecules, no divine intervention has been discovered. Due to long maturation the PFC can retains stressful memories of early childhood that become wired into the neurones. By age 14 a persons likes and dislikes are set.
Chronic stressful situations increase cortisol and glucose that can damage the PFC neurones and impair cognition. Two common stressful situations are isolation from the herd and loss of control. The PFC is capable of assessing a situation and by calm rational thought avert or minimize the stress response. For some reason this is seldom done. The common response to a stressful situation is the habitual primitive fight or flight high cortisol reaction.
We are all wired differently and respond differently to stress because of our individual PFC architecture.
Hi Gary—I can relate to your evolution in your faith, and world view. I was strongly grounded, as a child, in the Catholic faith. I was a philosophy major in college, and decided that the correct starting point must be “radical scepticism”. What was there that was beyond any possibility of doubt. Cogito ergo sum—je pense donc je suis—-I think so therefore I am—of course the problem was how do I know it is I who am thinking, and not someone/something else.
I realized that we humans exist in a world of doubt. We endlessly search for the “truth” terra firma—on which to build our world view. The scientific method seemed to be the only reasonable approach. It included my desire for scepticism as a starting point, and was an open process which incorporated/required verification as well as the possibility of falsification. I still think the “method” is our species’ greatest intellectual achievement. My love of doubt never failed to rear its head, and I became aware that our “method” was built on a number of axioms that were assumed to be true. The positive results of our “scientific method” in general seem to substantiate our belief in these fundamental axioms which are accepted without proof as being true. However, I am addicted to doubt, and I was perplexed. I slowly realized that there was no humanly possible way to support the fundamental axioms of science—even though I certainly wished to. Science, fundamentally, is a religion based on faith in its belief that reality is knowable by humans. We have no way of knowing whether this is true, but what other choice have we. We believe that we are rational, and we also believe that reality is accessible to our rationality. We believe that we evolved from more primitive life forms that existed in the same world that we do. We believe that even though we evolved in this world, we have developed the ability to understand the essential nature of this world—while existing in it and not knowing its limits nor fundamental nature with certainty. Doubt is our reality. Hope is our nature. Faith is our sanctuary.
IMHO–All the best to you—on the path—
P.S. People who have never been in a foxhole when the sh*t hits the fan find it easier to doubt faith in a greater power.
Erret – Great input on philosophy!
You are raising the most fundamental question of philosophy.
“How do we know for sure?” = “Truth”
Here I am on the side of Xenophanes and turning the thumb down for Platon. The collected work of the latter has been a rather chocking, though rather interesting, reading for me and I have still a few hundred sides to go. 🙂
And more!
With the brilliant philosopher Berkeley I fully agree that I can never prove that our reality really exists but only in your head as Descartes so poignantly already had declared in you quote.
To me (and I guess to most people) the existence of our reality is still an assumption that makes living more safe and especially when driving your car in heavy traffic.
Errett: Your post script is undeniably true. Religious faith is the rock upon which my mother built a good, and very long life, while weathering some of the cruelest slings and arrows of fate. Steadfast and remarkable was her faith. I have instead faith in the power of love and kindness, unshakeable faith, and unending joy and delight in the natural world. The forest is my church, my fellow hikers my pew-mates. I had only a brief bout of cognitive dissonance, and emerged intact and strengthened, but I see others experiencing it. Three books completely shattered the mythology I, and all of us, have been spoon fed in school and the newspapers and so forth: “Dissolviing Illusions,” “The Devil’s Chessboard,” and Thomas DiLorenzo’s “The Real Lincoln.” Music helps, too. Listening last night to Vladimir Horowitz play Chopin on CD was heavenly. Slept like a rock. Can’t decide if there should be a comma between “long” and “life.” and I was an English major!
Errett,
Is that an invitation to compare fans?
There’s no greater comfort than being relieved of the notion that there is a fantastical “power” that you must relinquish your intellect to in order to cope.
Put your head in the sand of Faith and all will be well. It works.
Until reality shows up.
Are we involved in this blog because of Faith?
Science is as flawed — and as perfect — as those practicing it. It will always be a mix. It will always be a struggle. It’s the best we’ve got. Rejoice in the best.
People won’t like this, but faith in a greater power is only a sky hook. Faith will not stop bad things happening to you or anyone else
Dr K, I hope you will allow this link from here in South Oz. It has nothing to do with CVD. It’s about eating a good diet to avoid becoming brain dumb ! But there is a lot in it which confirms and supports what you have said about CVD and ways to minimise it..
A very interesting read.. And not paywalled 🙂
https://indaily.com.au/eat-drink-explore/2017/08/09/diet-making-dumb/
Bill in Oz, some people frown on the mention of diet in this section of the blog. The consensus is that stress/strain is the big factor in CVD. The sense/perception of stress/strain originates in some part of the brain, therefore it can be said that the brain is the cause of CVD.
Andy, yes I know that. But if you actually read the link you will read that they are suggesting doing things which lesson stress. Like eating meals with family & friends…Curious eh ?
Excellent article Dr K .
I would highly recommend 24 hour saliva cortisol testing. It is a very useful tool indeed. It really made me stop and think what I was doing to myself. I found this website, very helpful when interpreting my results: https://www.drlam.com/
Sadly, many of your colleagues in the UK, think that such tests are utter bunkum but like you always say, opinions are changed one person at a time.
JDPatten reminded us yesterday that Dr Kendrick posed the question, “Why do atherosclerotic plaques never form in veins?”
Given that the focus of this entry in the CVD saga is stress — and I presume we are talking of mental or psychological stress — one wonders why stress doesn’t affect both blood vessels equally. Somewhere on the cascade of consequences that stem from the original stress, there has to be a branch, one side leading to arteries, the other to veins.
Reading Sapolsky’s “Why Zebras Don’t Get Ulcers”, he writes “One of the hallmarks of the stress-response is the rapid mobilization of energy from storage sites and the inhibition of further storage. Glucose and the simplest forms of proteins and fats come pouring out of your fat cells, liver, and muscles, all to stoke whichever muscles are struggling to save your neck.”
Heart rate, blood pressure, and breathing rate increase as well, to deliver fuel and oxygen to the muscles.
Sapolsky doesn’t mention the blood vessel repair mechanism (at least, not in the part I’ve read), but one would expect that the repair mechanism would be put on high alert during fight or flight because the chance of injury is far greater than when peacefully grazing.
And plaque is how the body repairs arteries. (How does the body repair veins? Don’t know.)
So everything is in place for a rapid build-up of plaque during a stressful event.
Another way to build up glucose levels in the blood is to eat plenty of carbs and not burn them off with physical exercise. Does the increased glucose level fool the blood vessel repair mechanism into thinking that it is a fight-or-flight situation and must go onto high alert? Don’t know, but I’m betting that it does.
If stress causes CVD and over-indulgence causes CVD, somewhere the paths must converge, and it looks like it’s at elevated glucose.
Martin Back: Last week I listened to an interview, recorded in 2006, with the late Howard W. Wayne, M.D., a cardiologist from the Noninvasive Heart Center, then read his web page on atherosclerosis. Lots of interesting stuff.
I just bought the book from Amazon for 3 USD! WIll read with (a) bated breath!
So re stress and elevated glucose: Would ketogenesis mitigate effects of profound stress?
Martin Back, veins do clog up if subjected to the same conditions as arteries like in CABG.
Glucose as being at the center of CVD (and many other diseases) is also my opinion. Inflammation is the common disease state and is caused by hyperglycaemia as well as gut dysbiosis, both can be controlled by diet. Effect of stress is to raise blood glucose levels This blog is about heart disease but what causes CVD also affects all the other organs.
My stress level just went down from this bit of news:
http://www.renalandurologynews.com/hypertension/editorial-questions-systolic-blood-pressure-target-of-less-than-120-mm-hg/article/478896/
“The researchers note that based on the results, for 1,000 persons treated over 3.2 years with a systolic BP target of less than 120 mm Hg versus 140 mm Hg, 16 persons would benefit, 22 would be seriously harmed, and 962 would experience no benefits or harms. In addition to a small decrease in event rates, the aggressively treated group more frequently had serious adverse drug events, which were possibly or definitely related to the intervention.”
http://www.renalandurologynews.com/hypertension/higher-systolic-bp-target-recommended-for-older-patients/article/632209/
“The American College of Physicians and the American Academy of Family Physicians have issued new clinical guidelines on hypertension recommending that adults aged 60 years and older be treated to a target systolic blood pressure of less than 150 mm Hg to reduce the risks of early death, stroke, and cardiovascular events.”
Andy S: Thanks! Lovely New Years gift. This agrees with the Port, et al analysis of the Framingham data.
Gary
Surely it is not correct to say that 962 would see no benefit’ some of them might have shares in pharmaceutical companies?
Cardiobrief has an odd pro-statin post today. Odd in that he is dismissive about the lack of patient data available for public scrutiny. Seems a blind spot. Yet he is the one who said cardiology is dead.
Ah, yes. Today is the day set aside for bankers — and other such-like upstanding professionals . . . and others — to recuperate from their, uh, day of recuperation . . .
It’s all Hogmanay, right??
Not really about heart disease, but readers here might find it interesting –
https://www.eurekalert.org/pub_releases/2017-12/lu-dd122017.php
FTL: “The research, published in Brain Research, could bring substantial improvements in the treatment of Alzheimer’s disease through the use of a drug originally created to treat type 2 diabetes.”
Or you could eat better, exercise, reduce stress, sleep better and fast…
Kidpsych,
: Interesting link, Thank you !
2; The drug used on the mice is not specified. Why ?
3 : Probably because it is a drug no longer under patent protection
4 : I wonder if the drug use is Metformin which has been used for a long while for T2D with longevity effects for such individuals…It is not under patent any longer for this purpose.
5: I wonder if it will be ‘reformulated’ and patented again as a drug for Alheimers patients
KidPsych, the Alzheimer’s Society partly funded the research. Your advice to eat better etc. would not benefit the organization.
My father-in-law went into a brief fugue state last year – not coincidentally I would say after he gorged on two boxes of Girl Scout cookies. (His girlfriend had been away and not able to stop him from overindulging.) Due to the fugue (and related loss of memory) he was tested at UCLA for memory issues and was placed on an experimental drug (to go along with statins, BP meds, and some others). I’ve made some inroads with him in regard to diet, sunshine but not exercise. Whether it’s the medication or diet (or some combination thereof), he’s been more lucid lately.
KidPsych, lesson from the Girl Scout cookie experiment: blood glucose has deleterious effect on brain function, or was separation from a loved one causing stress the cause, or perhaps a combination.
IMO, blood pressure is being treated like the cholesterol hype. “Only when SBP exceeds the 185 mark does the number of deaths start to increase steeply.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4195935/
Thanks Randal for this 2014 free access review article on High Blood Pressure. It does raise some very interesting discussion about ‘false’ or extremely confusing science .
Love it when a new month rolls over and I return from traveling. Life Extension had a couple of really interesting studies…10 years increased health via olive oil! Bifa gut bacteria in health…So there is one new thing to try as we switched to Olive oil years ago.
http://www.lifeextension.com/magazine/2018/1
tere are a lot of ageing issues with diminishing items, Hormones, gut bacteria and the like. Maybe one or a combination of these is part of the “switch” for some of the health issues such as HA, Strike and the like.
So I have been going back and forth on lots of items mentioned in the last few blog posts, chasing rabbit holes and such and there is a lot of info on the HPA axis, and lots of ways for it to go dysfunctional.
This will get into Heart Rate Variability (HRV). This is simple to measure and take action to improve in fact atheletes are using this today to gauge their fitness and response.
There is also Oaubain, which is touted for the imbalance of the parasympathetic and sympathetic imbalance issues.
There were some papers on the affect of insulin on the adrenal and HPA axis, but this is partially a diet issue, so probably not the right area? Many heart attack victims test as near diabetic..so this looks good as a possible issue. Increased body mass increased atrial fibrillation, 3x higher! depression results in 2x the HA risk. having children increases risk of HA, but as you increase the number of children, the risk reduces. Amygdala activity increases CAD! Vit C reduced post operative Afib by 87%.
About 80% of USA sudden cardiac deaths stem from abnormal electrical heart rhythm.
Ten years after Hurricane Katrina hit New Orleans, hospital admissions for heart attacks in the city were three times higher than they were before the storm
Stroke, Pneumonia, Sympathetic Nervous System
The prognosis of stroke depends mainly on the incidence of complications.1 Bacterial pneumonia is the most frequent severe complication1–3 and the most common cause of death in patients sustaining a stroke https://jneuroinflammation.biomedcentral.com/articles/10.1186/s12974-014-0213-4
Cortisol also has the function of maintaining blood glucose levels and energy metabolism during periods of stress. It suppresses the inflammatory response by inhibiting prostaglandin activity and has an adverse effect on the immune system
Glucagon is a polypeptide produced by the pancreatic islets in the upper gastrointestinal tract. The stress response causes glucagon levels to increase, so elevating the metabolic rate and lowering insulin levels. The result is hyperglycaemia and impaired glucose tolerance, together with carbohydrate, protein and fat destruction (Park et al, 2002).
Pathogen-induced heart rate changes associated with cholinergic nervous system activation.
https://www.ncbi.nlm.nih.gov/pubmed/21068197
Ageing Hypothalmus, the NF-κB pathway in the hypothalamus of mouse brains slowed aging and increased median longevity by about 20 percent, compared to controls
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3756938/
Effects of treadmill exercise on hypoactivity of the hypothalamo-pituitary-adrenal axis induced by chronic administration of corticosterone in rats
The results suggest that treadmill exercise recovered the dusregulated hypoactivity of HPA axis induced corticosterone administration. The results indicate that treadmill exercise may aid recovery of the HPA axis dysregulation in Psych diseases such as PTSD.
https://www.deepdyve.com/lp/elsevier/effects-of-treadmill-exercise-on-hypoactivity-of-the-hypothalamo-Zx0p916kGd
A spoonful of sugar: feedback signals of energy stores and corticosterone regulate responses to chronic stress
These studies revealed the marked postingestive effect of sucroseon regulation of function in the HPA axis of adrenalectom-ized rats and greatly clarified our understanding of the role of corticosteroid-sensitive metabolic feedback to brain
http://www.academia.edu/10395047/A_spoonful_of_sugar_feedback_signals_of_energy_stores_and_corticosterone_regulate_responses_to_chronic_stress
Both increased HPA axis activity and hyperinsulinemia are frequently observed in patients with diabetes. However, the effect of insulin per se on basal and stress-induced HPA tone is less clear. Brain insulin signaling is thought to play a role to stimulate the HPA axis during hypoglycemia counterregulation, Stress has an influence on adiposity, hormone release, food intake, etc.
http://www.cell.com/cell-metabolism/fulltext/S1550-4131(14)00026-6
Estrogen and brain aging in men and women: Depression, energy, stress
Besides providing new insights into biological energy and aging, the recognition that estrogen activates the stress hormone system–the pituitary-adrenal system–also provides clear insights into other problems, such as the polycystic ovary syndrome, hirsutism, adrenal hyperplasia, Cushing’s disease, etc.
http://raypeat.com/articles/articles/estrogen-age-stress.shtml
The Hypothalamic-Pituitary-Adrenal Axis and Viral Infection
The hypothalamic-pituitary-adrenal (HPA) axis plays an important immunomodulatory role during viral infection. Activation of the HPA axis ultimately leads to elevated plasma levels of glucocorticoid (GC) hormones with the ability to mediate adaptive behavioral, metabolic, cardiovascular and immune system effects.
http://online.liebertpub.com/doi/abs/10.1089/088282403322017884
Immune Modulation of the Hypothalamic-Pituitary-Adrenal (HPA) Axis during Viral Infection
cytokines, emanating from the immune system can have profound effects on the neuroendocrine system, in particular the hypothalamic- pituitary-adrenal (HPA) axis. HPA activation by cytokines (via the release of glucocorticoids), in turn, has been found to play a critical role in restraining and shaping immune responses.
http://online.liebertpub.com/doi/abs/10.1089/vim.2005.18.41
Depression and cardiovascular disease in women: is there a common immunological basis? A theoretical synthesis
We suggest that depression and CVD are both inflammatory disorders and that their cooccurrence may be related to how the HPA axis, the serotinergic system, and the RAAS via angiotensin II are affected by the excess secretion of proinflammatory cytokines.
http://journals.sagepub.com/doi/10.1177/1753944714521671
“It was found that serum IL-6 levels were about four-fold higher in men and women
who were chronically stressed by caregiving for a spouse with dementia when compared
to similar individuals who did not have care- giving responsibilities.”
https://adrenalfatigue.org/stress-cortisol-and-the-immune-system-what-makes-us-get-sick/
Glucocorticoid-induced myopathy
https://www.uptodate.com/contents/glucocorticoid-induced-myopathy?source=see_link
Take a look at Jeffrey Dachs, he covers Vit C, Ouabain, Testosterone, Estrogen, lots of referenced papers
Steve,
To me a very interesting deep digging into various causal chains.
What strikes me is the staggering interlinking in our physiology that seeps down to the molecular biology level of all our cells.
With Xenophanes we will never reach the “truth” but can get closer if we want – knowledge is possible!
Steve, superficially the olive oil study looks impressive. The problem is that the control diet was a low fat diet notorious for causing all sorts of diseases. A more realistic study would have been to compare two Mediterranean diets one with and the other without olive oil. Eating olives might provide more polyphenols.
Sorry Andy, I disagree. The low fat type diet is the one recommended as the best in many official diet regimes…This comparison of a low fat regime with a high er fat one is exactly what is needed …
But if some researchers have the funds & want to compare 2 different ‘Med type’ diets, one of which does not include olive oil, then that might also be worthwhile…
The problem is that I do not know of any country in the Mediterranean which does not used olive oil extensively. in meals. So it would be an imaginary comparison..
Bill in Oz
Fat is a better fuel for mitochondria, more ATP and less ROS. That is one reason for avoiding a low fat diet.
Exactly Andy. I agree. Yet in many countries low fat diets are the officially recommended ones.
That’s why the comparison used in this study is a good one. And it showed that low fat diets lead to lower life expectancy.
This may have been linked in past blogs, but as well as memory lapses, my not reading all of the links posted would mean I hadn’t seen it if it was.
http://www.orthomolecular.org/library/jom/search_results.shtml?cx=012934609838436511334%3Aeuo7oo38sqc&cof=FORID%3A11&q=rath+pauling&sa=Search&siteurl=orthomolecular.org%2Flibrary%2Fjom%2F&ref=&ss=3645j3202869j12
How significant it?
This should be compulsory viewing/listening for all medical students and, more importantly, their prospective patients.
On a lighter note, I have the book, now I’ve seen the film, is there a T-shirt available?
Note to all:
When posting an embedded video, it would be helpful to post the link as a line item. On iPads at least, when the emails come through it isn’t possible to see the video directly, but you have to go to the blog to find it. A text link would allow quicker access.
Since this blog is about stress as a cause for illness I now wonder if this type of “causation” has followed the human societies since the very “beginning”.
What triggers my suspicion is my present captivating reading of the book “Shamanism” by Mircea Eliade. Here I learn that the most important activity of the shamans was their “GP” activity as healers. Probably the major part of the healing activities was related to the issue of the “soul” of the patient, which had been possessed by some evil spirit as the cause for the illness. Possibly the patient had been “strained” by some external evil stressor within the society.
While the shaman “doctor” was the major player in the process of healing many members of the extended family were important participators at the seances. This sound like a holistic good way to handle and cure mental illness and infinitely superior to the ten minutes attention given and a bottle of SSRI pills handed out today.
Malcom,Are we allowed to post videos on this stream? SW
Life extension has a few things on EVOO for those diet lead individuals: http://www.lifeextension.com/Magazine/2018/1/Olive-Oil-Markedly-Extends-Human-Lifespan/Page-01 Showing 9.5 extra years (over 65) for those with the highest levels of EVOO
from this report we have a couple good items:
Protective effect of homovanillyl alcohol on cardiovascular disease and total mortality: virgin olive oil, wine, and catechol-methylathion. https://www.ncbi.nlm.nih.gov/pubmed/28446500
Wow, 30x increase in CHD from elevated F2-isoprostanes, the best biomarker found. Google the papers yourself, there is a little disagreement about the best way to measure this.
Davis CR, Bryan J, Hodgson JM, et al. A Mediterranean Diet Reduces F2-Isoprostanes and Triglycerides among Older Australian Men and Women after 6 Months. J Nutr. 2017;147(7):1348-55.
Roberts LJ, Morrow JD. Measurement of F(2)-isoprostanes as an index of oxidative stress in vivo. Free Radic Biol Med. 2000;28(4):505-13.
Schwedhelm E, Bartling A, Lenzen H, et al. Urinary 8-iso-prostaglandin F2alpha as a risk marker in patients with coronary heart disease: a matched case-control study. Circulation. 2004;109(7):843-8.
So now my list has a new risk leader, Oxidative stress, which can be reduced by EVOO. Naturally Cushings disease is far higher, cushings causes increased adrenal function and there is a cushing syndrome….http://www.jabfm.org/content/25/2/199.full
The Big Hitters for increased HA risk:
High F2 Isoprostanes – Oxidative Stress – 30x
Upper respiratory illness – 17x
Financial stress – 13x
Eating disorders – 9x
HIV – 5.6x
Preeclampsia – 4x
Lupus/Arthritis – 2x
Someone mentioned that these may not be real percentages….a math review, when we say 30x, that means 30 times higher risk, in percentage this is 3000%. Now if you look at effectiveness of statins, they give relative risk, because it is 1.5% VS 1% which is 50% greater than 1%, which is what the news reports : “50% greater improvement for statins” this is why we should use NNT instead in these small improvement cases because for 0.5% improvement, it would require 200 people to take the statin to see one person improved. Very small indeed…but not to be confused with multiples. If someone requires more examples, please let me know.
Another interesting thing to look at are the graphs of heart disease
https://www.google.com/search?hl=en&tbm=isch&source=hp&biw=1231&bih=877&ei=XPNSWsD4MoLcjwS7lpnQCg&q=heart+disease+graphs+and+charts&oq=heart+disease+graphs&gs_l=img.1.1.0l2j0i30k1.1750.11817.0.14070.20.16.0.4.4.0.329.2463.0j1j9j1.11.0….0…1ac.1.64.img..5.15.2544…0i5i30k1.0.OTTzT_FvUBE
Remember, correlation does not mean causation!
The Australian article you sounds interesting Steve. But when I went looking I found it iis paywalled.
Now that is really annoying as nearly all academics here are very well compensated on the public titty. And looking at the author information I see that these authors are all employed at government Australian universities.
It may be boring to some : but paying $40.00 to rent 24 access to research I’ve already [aid for in my taxes is frankly a big no no. Paywalled is blackballed, especially if the researchers are Australian.
But this article Steve by almost the same authors published later in 2017, is available free and complete. Interesting the authors acknowledge a research grant for this research from the Australian government.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5490513/
It looks like somebody realised after the first was published with a paywall, that a mistake had happened. And then it was released again with free access.
Soooo..Now the issue is whether a Traditional Mediterranean Diet does make any difference.. And that raises the issue of what a Traditional Mediterranean Diet actually is. Dr K has made many remarks here that it does not exist as there are 18 countries in this region.
However the authors here specify a ‘Traditional Mediterranean’ diet to be the following :
” …. 1–3 tablespoons of extra virgin olive oil, 5–6 servings of vegetables, 2–3 servings of fruit, 4–6 servings of grain foods, up to 1 white potato, up to 200 mL of red wine and up to 1 cup of skim milk per day, and 4–6 servings of nuts, 6 servings of Greek yoghurt, 3–4 servings of cheese, 1–3 servings of poultry/pork, 3 servings of fish, 3 servings of legumes, 1–2 servings of small goods, up to 1 serve of red meat, up to 6 eggs, and up to 3 servings of discretionary foods per week…….
.. To adjust for differences in estimated energy requirements, recommended servings of key foods was reduced to create 3 additional lower energy diets, which nonetheless retained a nutrient profile in line with MedDiet principles. ”
Some of these recommended items were daily but some were weekly. It’s not clear which is which in the article and that is a failing.
This diet is by the way close to what I eat myself at this time. However I rarely eat ‘small goods’, poultry or pork, and 4-6 servings of nuts seems too high..I don’t usually drink skim milk only full fat… And I love my butter..
Without the paper specifying what constitutes a “serving”, it doesn’t seem very meaningful.
A H Notepad, the term ‘serving’ is used for many different types of food> Vegetables, Yogurt, Fruit, Nuts, Grain foods etc.. I suggest that a perousal of the actual research paper & notes, would reveal what a serving of each item consists of.
‘Everybody told him: you’re wasting your time. Obviously, the boss is going to be more stressed because he’s got more responsibility. But when Marmot published his results, he revealed the truth to be the exact opposite. The lower an employee ranked in the hierarchy, the higher their stress levels and likelihood of having a heart attack. Now he wanted to know: why?’
An excellent review of ‘Lost Connections: Uncovering the Real Causes of Depression – and the Unexpected Solutions’, by Johann Hari, in the Guardian today:
https://www.theguardian.com/society/2018/jan/07/is-everything-you-think-you-know-about-depression-wrong-johann-hari-lost-connections
A new study published in Circulation today about how exercise reduces CVD in older people.
http://circ.ahajournals.org/content/early/2018/01/03/CIRCULATIONAHA.117.030617
Also reported today also by the ABC here in Oz as apparently this research was partially done here in Oz by the Baker Medical Research Institute in Melbourne. There is an interview with one of the research ‘participants’ who lost 45 kg over the 2 years.
http://www.abc.net.au/news/2018-01-09/baby-boomers-can-protect-heart-by-exercising/9312574
The interesting thing is there is nothing I can see about diet changes.
Bill,
I, for one, is a strong believer in the importance of exercise for CVD-victims – the harder, more intensive, the better.
But I don’t for a minute believe that exercise will help you to reduce weight. I think there was a Danish well controlled experiment, som eyears ago now, where overweight people during a year or so was running a numbers of marathons and where the weight loss was miniscule.
Goran, I think you mean to say that the diet also needs to change..And I cannot argue with you about that as the article does not discuss this issue at all.
But curiously back around 2003 I was well over weight at 104 kg. I enrolled at a gym and trained quite intensively for a year of so..And at my lowest weight I was 82 kg with a BMI of 18. A really great change. However I also stopped eating comfort foods like potato chips and 50% sugar chocolate…..
I agree. Exercise for fitness, food choices/restriction for weight loss. 👍
Dr. Goran: I think you’re right about exercise and weight loss. Further, I think the obsession with weight loss is entirely a mistaken approach. It is metabolic health we should be aiming for. I’m getting sick and tired, as well, of the word “exercise.” It is being active, physically and mentally, and involved in living that is health-promoting, regardless of what those activities are (excluding criminal activities, of course, which leaves out the politicians and dietitians).
Gary Ogden, movement is what the body needs otherwise the lymphatic circulation stagnates. For us who are approaching four score, maintaining healthy lymph flow would be beneficial. Visualizing how movement assists lymph flow is a good motivator for exercise.
Andy S: Absolutely right. I’m in favor of both movement and lymph flow. Though I no longer need to chop wood to stay warm, I move vigorously twice a week or so, and moderately the rest of the time. I call it living rather than exercise.
Recently I’ve been reading Wolfgang Lutz’s “Life Without Bread”. Lutz was the Austrian physician who tried low-carb in the late 1950’s and began prescribing it to his patients.
Lutz describes an experiment with chickens. He fed one group a low-carb diet (probably resembling what wild or pasture-raised chickens eat) and the other group a “modern” grain-based diet. The low-carb group had much less atherosclerosis than the grain-fed group. But Lutz was struck that the difference was “on average”. Both groups showed a range of atherosclerosis, from none to severe, but the low-carb group as a whole had less.
This might make sense in light of strain in atherosclerosis. Lutz does not report controlling for “pecking order”, just diet. I wonder if the lower-ranking chickens were more likely to get atherosclerosis than the higher-ranking chickens. Certainly, it might worth repeating the experiment and looking for that effect.
OT: I had to laugh at Richard Lehman http://blogs.bmj.com/bmj/2018/01/08/richard-lehmans-journal-reviews-8-january-2018/
“If you put people randomly in a room to discuss statins for half an hour, the space will get hotter, its pressure will increase, and the two factions will end up at opposite sides of the room. It’s like Boyle’s Law of Gases in reverse.
“Now throw in a guideline. The gases will explode, but then the same negative entropy will reassert itself and within half an hour every particle will be back in its original position. You can do this five times and the same thing will occur each time.”
Thank you Doctor for putting this up together!
Next blog. How to get rid of the underlying cause?
Change partner, job, meet new friendly people, change inner language about self, sleep well, exercises often and eat good food in good company. 🙂
oh! And being wealthy helps too, it reduces the strain to pay bills monthly…
Vitamin C has been covered by Dr Kendrick and in readers’ comments over the years and, I think, is rated as a serious contender in triggering the artery damage/repair process.
Here’s a new talk from Dr Matthias Rath dated Nov 2017:
It clocks in at 1 hour 37 minutes and in addition to vitamin C deficiency causing plaque formation, also covers irregular heart beat and type 2 diabetes and more.
I rate him – he talks a good talk, is a good public speaker and is doing the research.
Charles, thanks for that link. I will spend soem time and watch the video of Dr Rath.
Matthias Rath is ‘number one enemy’ for the medical profession. He certainly is a maverick. I find his ideas interesting, but I tend to stay clear of talking about him too much, as he enrages doctors to the point that they lose the ability for any rational discussion. Look up HIV/AIDS matthias rath South Africa – if you wish.
Dr Kendrick, all humans are human and fallible at times. This includes medical doctors. You probably remember the Australian obstetrician William McBride. He made the link between thalidomide and the thousands of babies born grossly deformed. In this he was a true hero.
However McBride was fallible and ended his medical career in disgrace.
But this does not make his earlier medical discovery about thalidomide wrong or discredited.
Dr Rath’s work in South Africa on HIV was misguided. However does this make wrong ( or discredit ) his earlier work on CVD with Linus Pauling ?
I am at the 15 minute mark of the video. His presentation is clear and simple. And easily understood. That itself is very rare among medical talks. So I will watch the rest.
Bill in Oz: HIV/AIDS was a pharma-led scam for the benefit of pharma, like Zika, swine flu, etc., ad infinitum. All of which have disappeared without a trace. On HIV/AIDS see Dr. Peter Deusberg.
Just reading these blogs should be a cure for most ills. With proper nutrition there is little to worry about. Unless maybe, you are in a room of recently vaccinated antibiotic devouring “junkies”.
I will have to look up his work on HIV. Was he aware vitamin C is also a useful input for HIV?
The controversy that Dr. Rath got himself involved in, in South Africa was I think about treatment of HIV.
AH Notepad: HIV has never been isolated. Does it exist is a good question. If so, is it pathological is another one. We were told, in the 1980’s that soon people would be dying in the streets; such was the menace. But HIV/AIDS disappeared in the U.S.
I have now watched the whole of this video of Dr Rath’s. I can well understand why some folk in the medical business & the pharmaceutical business react to Dr Rath with fear & loathing.
He is also an inspiring speaker. Dr Rath strongly states that CVD, strokes, T2D & heart failure, can be PREVENTED. If he is right ( and I suspect he is ) then he is completely undermines their commercial ‘success’.
The key issue is whether the collagen that is the structural backbone of the coronary arteries, is weakened by insufficient Vitamin C in the diet.
Bill in Oz: And the corollary question: Does taking high-dose vitamin C strengthen and improve vascular function? Seems there is good evidence that it does.
Gary,
Are you seriously suggesting that HIV was a scam designed to sell medication and has disappeared?
In South Africa we have 7 million people living with AIDS, and 700 new infections a day. In some parts of the country 30% of sexually active people are infected with HIV. It’s no scam, it’s very, very real.
Things were even worse, but thanks to frank discussion and education, free condom distribution, and anti-retrovirals available from government clinics, the prevalence is coming down.
I knew people who died of AIDS. It was a very nasty way to die before ARVs became available and enabled a normal life for the infected.
Martin Back: I most certainly am. Here are three sources of good information about it: Dr. Peter Deusberg (from UC Berkeley), Janine Roberts “Fear the Invisible,” and Celia Farber’s (I think 2006) article in Harper’s magazine. HIV/AIDS was pharma flexing their muscles. They hired gay activists (and formed groups such as ACT-UP) to attack and vilify anyone questioning the official narrative. CDC scientists at the time were nearly unanimously opposed to the invention of HIV/AIDS, but were over-ruled by the director, who, then, as now, works for pharma rather than the public. Africa has many woes. but poverty and malnutrition, lack of clean water and sanitation are the drivers, not an unseen microbe.
Yes Gary I think there is good evidence that vitamin C is beneficial. It’s certainly part of my standard supplements list. And watching the video of Dr Rath has strengthened my views on this.
By the way this talk took place in a church in Utrecht in the Netherlands. The acoustics are fantastic and in the background are lots of wonderful carved wooden figures.
Bill in Oz: Yes, it was a beautiful setting. I only watched twenty minutes or so because he speaks very deliberately, I can’t read Dutch, and I already know enough about vitamin C. I take 3-4 g/day, from powder, produced in Scotland, mixed with Gerolsteiner mineral water, sipping it throughout the day like Dr. Goran.
Gary, first a thank you for all the (nearly) insider view of the operation of the pharma industry in the US. I remember the vilification of Duesberg in the 1980s (I think) and thinking the vaccine lobby was a bunch of opportunists. No internet then though.
Only 3-4 g a day?? Are you sure it is made in Scotland? We have many instances in the UK where it is permitted to make such claims even if a product was only sealed into a container in the UK, but was imported from anywhere.
AHNotepad: I trust my supplier (Health Ranger store), that when he says it is made in Scotland it is. I’m taking what I consider a therapeutic dose for me. I have no symptoms of any cardiac-related disease, and can do intense exercise and climb to high altitude without any difficulty. Tomorrow I will be 69. I feel like the infant among the pantheon of venerables here!
How much v c do you take and what kind thanks
Doc! Look at the can of worms you’ve opened by mentioning HIV right after having said you tend to stay clear.
And, what does it have to do with stress/strain except to stir it up?
(Fritz Perls would have had an issue with this approach.)
43 is getting a bit thin, is it not?
I wonder if Rath was not so much wrong about HIV in Africa, as incomplete.
Vitamin C, I hope, is a very useful supplement, as like several here I take quite a few grams a day plus many more grams if I feel unwell. Could it be the HIV/Africa situation is exacerbated by a generally poor diet? Which possibly includes a significant amount of refined carbohydrates? Though it appears many in Africa have the HV virus, does that mean they will suffer from AIDs? Rather in the way that many in “western” countries carry the flu, and other, vira, but because of good nutrition we don’t suffer from the diseases associated with them, except where the immune system is compromised. A video with an anecdote at the beginning indicates vitamin C might well be useful in the treatment of AIDs https://youtu.be/W5Bgdqsorg0.
A H, I know very very little about HIV in South Africa. And my knowledge of Dr Rath’s role in the fight against this disease is very minimal also. So I will decline to express an opinion here. But Dr Rath seems on the money as regards vitamin C. As was his Nobel laureate mentor back in the 1970’s.
Well, I’m gobsmacked. Anyone who believes “poverty and malnutrition, lack of clean water and sanitation” can be sexually transmitted is a wacko.
Martin Back: Those four factors: poverty, malnutrition, the lack of sanitation and clean water are clearly and unequivocally causally associated with higher morbidity and mortality, especially among children. If there is such a disease as HIV/AIDS which is sexually transmitted, why has it essentially disappeared in the U.S.? If you are interested in understanding HIV/AIDS, read Janine Roberts’ “Fear of the Invisible,” a very detailed explanation. I have no dog in this fight. I’ve never known anyone impacted by this, and knew nothing about it until I read Celia Farber’s excellent piece in Harpers magazine in 2006. What I have come to realize over the past few years is that we’ve all been fed a load of BS by the media our whole lives. I am skeptical of the official story on everything. Pharma is both very powerful and diabolical, and the media is beholden to them for advertising revenue. There are few, if any, standards left in journalism. An excellent new book which discusses this issue is Jonathan Rose’ “Reader’s Liberation: The Literary Agenda” (available in March from Oxford University Press).
Gary,
I won’t bother to read your references. I would rather be instructed by people who actually have to deal with the AIDS problem on the front lines, like in South African hospitals and clinics today, and who have to educate people to prevent them getting AIDS, and counsel them when they’ve got it.
Your references are probably the same as the people our President Mbeki read in his nightly cruises of the internet, who persuaded him that HIV was merely an immune problem, and caused him to say, “Let them eat beetroot, garlic, African potato, and lemon juice.” Thus denying state-financed medication to hundreds of thousands who went on to infect the current generation, and who then died, backing up several funerals deep at the undertakers.
HIV/AIDS has “essentially disappeared in the U.S.” Er, no. “Antiretroviral therapy has transformed HIV from a death sentence to a manageable chronic condition for many. Yet as the death of 41-year-old Broadway composer Michael Friedman this past Saturday reminds us, thousands of Americans still die every year from HIV/AIDS. ” — https://www.huffingtonpost.com/entry/hiv-aids-deaths-united-states_us_59b6bb38e4b06e4604a22f2c
The reason AIDS is not a major problem in the US is that activists promptly got the information out there regarding safe sex and injection practices — even gay porn actors have to wear condoms, by industry agreement — and the early use of such ARVs as were available.
One reason ARVs weren’t used in South Africa is they were hellishly expensive by our standards, so the government had to face accusations like, “Why are you spending so much money on people who got AIDS because they were immoral, while I am honest and hard-working, but I am still poor and starving?” Fortunately the government was able to negotiate the price down, and many drugs are now off patent.
As for HIV not being sexually transmitted, that is an absurd statement. How else do you explain transmission, except by exchange of bodily fluids, as in sex, sharing needles, and blood transfusions? How else to explain this: “Research studies in East and South Africa found that circumcised heterosexual men were approximately 50% to 60% less likely to become infected with HIV than uncircumcised men.” — http://www.catie.ca/en/fact-sheets/prevention/penile-circumcision-reduce-risk-hiv-infection How else to explain how isolated women in rural South Africa got AIDS after visits from their husbands who became HIV-positive while away in the cities?
While “poverty, malnutrition, the lack of sanitation and clean water” undoubtedly contribute to weakening the immune system and thus make people more vulnerable to developing full-blown AIDS after infection, the effect cannot be great, otherwise every ‘flu epidemic would result in a huge increase in the death rate. No such increase has been noted, which tells me that the poor are nearly as virus-resistant as the well-fed. Plus the fact that health-aware doctors and nurses get AIDS from needle-stick injuries, and well-fed middle-class people got AIDS from infected blood before strict blood testing. A good immune system is no guarantee you won’t get AIDS.
Vitamin C might help by firming up the collagen structure of the skin and making it less susceptible to micro-tearing during sex. Maybe it’s an immune booster and helps to fight off slight infections. I don’t know how many virus particles are needed to overwhelm the body’s defenses.
But I see no reason to doubt the standard picture: You get infected with HIV from someone’s bodily fluids, your immune system fights the infection for a long time (the “window period”), but eventually it succumbs and you start getting opportunistic infections and cancers, and after that it’s just a matter of time until you die. But effective therapies are available these days, and provided you are diagnosed in time and take your medication religiously, you can live a normal life for a normal lifespan.
When I think of AIDS I think of Chuck (made-up name), a gay man in his 30s, a hugely talented clothing designer who was sent all over the world by his company to trade shows etc. Charles was a gym rat, fit and athletic, and always very positive and enthusiastic. He was a friend of a friend, and I happened to bump into him as he was going home to die in the care of his mother. He was shrivelled up like a little old man, with a thin trembly voice and no energy, a shocking change from the last time I’d seen him. He tried to be positive, but you could see he was finished, and he died a few months later.
I think of DeeDee (made-up name), an actress from my support group, always full of actressy dramas and a friend to everyone. But there was always a sadness about her. She never got over the fact that she had introduced her only son to the man who gave him AIDS, from which he died ten years later.
I think of the Malawian who used to hang around the car park and who I paid to wash my car once a week. Fit, energetic, built like a boxer and always friendly with a big smile, one day he disappeared. Some months later he turned up again. He was tired and wasted away, and slinking about like he didn’t want anyone to see him. I didn’t ask him what was wrong with him. It was obvious he had AIDS. He washed my car one last time and I never saw him again.
All these cases were before effective ARVs became available. It doesn’t have to happen now, because Big Pharma came to the party and developed the drugs. If they made money, they deserved to. And if you think you don’t know anyone with AIDS, check their medicine cabinet. These days you can’t see who’s got it, and no one will tell you they’ve got it, because it is still a shameful condition to have.
I do not enter the HIV debate, much, for the same reason that I stay away from the vaccine debate. Very entrenched views, enormous emotional responses. What I do know is that is a far more complex thing than most people would have us believe. AZT, for example, was so utterly toxic that it should never, ever, have other than a time of great panic, where people were grasping at any and all possible straws.
The test used to diagnose HIV/AIDS, could not actually diagnose it – according to Kary Mullis (inventor of PCR, the test used, and winner of Nobel prize for doing so). There has never been a randomised placebo controlled trials of any medication for the treatment of AIDS. Everything since AZT, has been a comparison against AZT – which killed more people than it cured. The man who first claimed to have discovered the virus, Robert Gallo, later admitted that he had not. He just made it up. As to why we have never manged to find a vaccine for HIV – well….
In my opinion, the entire saga of AIDS/HIV has been rather shameful. The most shameful thing is that anyone who dares to question anything about the ‘standard AIDS/HIV model’ is shouted down. There is a debate to be had here, but no debate can be had, because you are immediately accused of HIV-denial, or some other utterly stupid phrase, designed to demean.
Getting angry does not anyone right.
Thank you, Dr. Kendrick. I have nothing more to say on the topic.
If you get treatment, you live; if you don’t get treatment, you die. To me, that’s conclusive proof of the standard model, so I won’t say any more on the matter either.
Sorry to point this out Martin, if you get treatment you’ll die, if you don’t get treatment you’ll die.
Charles,
Thank you for the link to this great talk. It confirms that I am on the right track with my 15 g/day of vitamin C.
Charles Gale, Thanks for that link, in my opinion an excellent talk. I am now watching the talk he gave in Barletta.
There is the conundrum that though 16 million are dying each year from CVD, the world population is still increasing by 85 million a year. While looking at a fix for CVD is a good thing to do instead of forcing people to suffer debilating conditions, some solution has to be sought for the population increase. If we don’t deal with it, it will deal with us.
Interesting discussion about stress/strain. Look forward to the next blog.
Please see this article from the Globe and Mail in Toronto.
https://www.theglobeandmail.com/opinion/a-diet-high-in-fat-is-best-with-the-right-kind-of-fat/article37474768/
“A diet high in fat is best – with the right kind of fat”
Bill In Oz, I consider the term “serving” to be as meaningful as “Mediterranean diet”, ie poorly defined and approaching meaningless. A “serving” to one person will mean something different to another, and will have a different effect, probably as accurate as adding fluoride to the water in the respect that a “one size fits all” is unsatisfactory, not to mention unscientific.
A H I find it amusing & curious. A few days ago as part of adding to the discussion here, I provided this link:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5490513/
And it’s about Mediterranean diet being heart protective.
And you have basically dismissed it as useless.
Also a few days ago, again as part of the discussion, I provided two links which emphasise how exercise is beneficial and heart protective.
http://circ.ahajournals.org/content/early/2018/01/03/CIRCULATIONAHA.117.030617
http://www.abc.net.au/news/2018-01-09/baby-boomers-can-protect-heart-by-exercising/9312574
The ABC news report shows 2 photos of one of the participants in the Baker Research Trial. Before & after photos. One shows him at 135 kg. before starting the exercise program. The second show him after 2 years of the exercise program weighing 85 kg, He looks fit and glowing. A huge difference for the better.
And providing these links also drew some critical comments from folks here….
Bill In Oz, Critical comments are likely in discussions in blogs such as these because we don’t know the absolute truth, and so sometimes there will be agreement, sometimes disagreement. Most posters here have received critical comments, it’s just part of the process. There would be little to drive discussion if everyone agreed. It’s not a personal criticism.
Bill in Oz
Your point about the weight loss in the video is interesting. All the accepted sources etc say exercise does no t entail weight loss, all the exercise sites Livestrong, Verywell etc all mention running walking workouts as a sourc of weight loss. And, anecdotally, I find exercise at least stabilises my weight and encourages a bit of loss, as in the post-Christmas period. So what gives, delusion?
It is the diversity of human genetics, lifestyle, culture, diet, and personal habits….We are each unique..
It is a delusion to think that there is one simple solution.
A Phillip, that article from the Globe & Mail in Toronto is full of misinformation. It propagates yet again the theory that eating high cholesterol foods will cause heart disease. If you have read anything by Dr Kendrick here you will know that this is simply false.
I suggest that this article is a ‘Trojan horse’ to discourage meat eating and encourage vegetariansm or veganism..
And what the hell are these two diet ‘experts’ recommending Canola oil for ?
Bill in Oz, the expert on high fat diets works for the food industry. He cannot move fast in embracing cholesterol, meat and egg yolks. He is also working on official dietary guidelines.
Canola oil is not on my list of healthy fats since canola has been genetically engineered.
Thanks Andy !
Bill In Oz, the “Mediterranean” diet is not one collection of foods which is common around the Mediterranean. It depends where you are, and in most people’s view it would amount to having different diets in different places, depending on what was available locally, and their local tradition. That is why I continually question any reference to the “Mediterranean” diet, because to paraphrase Andrew Saul, the Medditerranean diet is rather like the Loch Ness Monster, “Everybody knows what it is but nobody has been able to bring one in yet”. People have brought in several different versions, all claiming to be the definitive Mediterranean diet, but they don’t necessarily look similar.
As for exercise, I agree that it is useful to maintain tissue tone, though I don’t get much as I spend too much time on good blogs 🤫, however as Goran pointed out earlier, backed up by a Danish study, exercise didn’t prove to be much of a. contributor to weight loss. Any weight loss seems to be more a diet function, ie eat pleanty of fats (expept PUFAs) and not much carbohydrate.
A H I guess there id now with with this study, an ( official ? ) Australian Mediterranean diet as well…And as it seems to work, maybe it should be adopted by those wanting to avoid CVD..
Along with lots of exercise and various supplements like Vitamins C & E, CQ10, Chondroitin sulfate, Niacin, K3, D3, Magnesium, Potassium, fish oil capsules and garlic oil capsules…
Billl in Oz, would you be interested in a traditional Baltic diet circa 1200 AD? The barbarians from the north beat the crap out of the people eating a Mediterranean diet. There was not much fruit or wheat in northern Europe at the time. My suspicion is that in the winter they existed on pickled herring and sauerkraut as staple foods supplemented with whatever they found in the forrest. No olive oil either.
LOL . I must memorise this. It’s a great repost to anyone advocating the “Mediterranean diet” at a gathering. They won’t be expecting it, and it will probably leave them speechless. If it doesn’t you will know they must be one of the readers of this blog 😂
Notes on Dr Rath’s video:
His notions of causes of cardiovascular disease differ from Dr Kendrick’s somewhat.
Rath: Collagen suffers from C deficiency and heart “movement” leading to faults in vessel walls which are addressed by the healing system of intrusive sticky lipoproteins.
C is the fix.
Kendrick: Mechanical forces cause endothelial cell stripping, triggering local clotting which is then covered with new endothelium. This traps the clot underneath with its constituents of cholesterol etc.
C is the fix.
Maybe one or he other is perfectly descriptive, or maybe it’s a combination of both. In any case, vitamin C is the preventive/treatment. The trick in both scenarios is to keep ahead of the process with C as the big helper. Not so different, perhaps, in the final effect.
Dr Rath goes on about micronutrients but only mentions briefly that they might include carnitine, CoQ10, B viamins — B1 in particular — and polyphenols. More details would have been nice. The website was no help either with drop-down search menus that lead nowhere. I did order his book. Perhaps details are there?
A quibble about Rath’s knowledge of the heart:
He shows a nice picture illustrating an artery on the surface of the heart being flattened during systole. It’s actually the smaller more distal arteries that delve into the heart muscle that get flattened by that muscle with each contraction. The surface arteries — to the contrary — swell with blood during systole, acting as an elastic reservoir to then be emptied into the smaller vessels during the relaxation of diastole when those smaller ones open again.
Whichever description is correct, there’s a lot of physical stress and strain going on there!
Here’s me quoting the news again, this time about Pres. Trumpet’s medical checkup:
‘…… the 71-year-old president enjoys fast food, and is overweight. He takes statins to keep cholesterol in check…..’
Might explain a few things about his sleep patterns, mental state &c.
And thus Craig liable to suffer a heart attack or stroke or a range of statin side effect problems..Ummmmm..The US VP needs to keep an eye on things I suggest.
a good article on topic:
http://www.greenmedinfo.com/blog/stress-trauma-and-autoimmune-disease-it-s-not-all-your-head