22nd October 2021
Studying cardiovascular disease for over thirty years can take you to some very interesting and seemingly strange places. Places where I never expected to find myself. Connections appear where you least thought they would be, and entirely new worlds of research open up. Very often, into places where mainstream medical thinking simply does not go.
The fascinating thing is how so many things end up looping back round, in ways that you would never have considered. One of those places is within the world of vitamins. Vital…amines, and the connections to cardiovascular disease.
Unfortunately, mainstream medicine has firmly locked vitamins into a tightly constrained box. Yes, it is accepted that vitamins are vital, because you die without them – that is where the ‘vital’, in vitamins, comes from after all.
However, it is universally believed that the exact requirements for all vitamins – known as the recommended daily allowance (RDA) – which were established decades ago. It is also universally believed that everyone gets sufficient vitamin intake from their diet, so there is absolutely no need for supplementation.
But how true are these comfortable assumptions? At one point I looked into Vitamin B12 deficiency. Even mainstream medicine agrees that this can, and does, occur and can lead to very serious medical problems. Irreversible nerve damage and paralysis, for example.
The normal range for Vitamin B12 in the UK varies from 190 to 950 picograms/ml (pg/ml). [A picogram (pg) is one trillionth of a gram]. This at least is the normal range, in some laboratories… in some places the UK. In truth, it is almost impossible to find a consistent figure.
This ‘normal’ range also varies enormously from country to country. In Japan, for example, it is 500 – 1300 pg/ml. Thus, the lower range is nearly three times higher in Japan than the UK1. If you went to your GP in the UK with a level of four hundred and said you were Vitamin B12 deficient they would point you to the door. In Japan, they would treat you.
Another thing to note here is that the range is almost always ridiculously wide. It can vary by a factor of five! This alone suggests that people are pretty much guessing at what “is” normal. Despite this, most doctors remain perfectly content that a normal/healthy level has been well established and is based on robust science. There is no need to look again.
This is not the case, not even remotely. Here, for example, are the first three key recommendations on determining what constitutes Vitamin B12 ‘deficiency’ from the British Society for Haematology – with some of the highly technical text removed. They use the term cobalamin here, not Vitamin B12, although it is (basically) the same thing [Cobalamin (Vitamin B12) comes in several different formulations e.g., hydroxycobalamin, methylcobalamin, cyanocobalamin]
- The clinical picture is the most important factor in assessing the significance of test results assessing cobalamin status because there is no ‘gold standard’ test to define deficiency
- Serum cobalamin currently remains the first‐line test… Serum holotranscobalamin has the potential as a first‐line test, but an indeterminate ‘grey area’ may still exist.
- Definitive cut‐off points to define clinical and subclinical deficiency states are not possible, given the variety of methodologies used and technical issues, and local reference ranges should be established2
There you are, clear…. as mud. What the British Haematology Society informs us is that: there is no gold standard test for vitamin B12 deficiency, there are also ‘grey’ areas, and ‘definitive cut-off points to define deficiency states are not possible.’
As with almost all areas of medical research, the more you dig down, the more uncertain things become. The authors of the report are not even sure if you should be measuring cobalamin, or holotranscobalamin – whatever that may be. It sounds like something from Star Trek.
When it comes to vitamin D there is a similar lack of clarity. In the UK, recent guidelines on vitamin D suggested more people should take supplements… finally. However, the NHS advice on vitamin D then goes on to make this statement:
‘…although roughly one in five people has low vitamin D levels, this is not the same as a vitamin D deficiency. It is not accurate to say that millions of people are at risk of deficiency.’3
So, according to the NHS, a low level is not a deficiency. However, a low level cannot, by definition, be normal. For, if it were normal, you could not call it “low”! So, what is it? Here is where words really start tripping over each other. Low, deficient, normal…optimal, inadequate, sub-optimal? Trying to pin any clear definition down is, I can assure you, like trying to pick up mercury using your fingertips.
In the same article it is stated that a blood level of 20nmol/l is ‘sufficient’. Again, what does sufficient mean? Is it the same thing as normal, or is it optimal? Is this really the level we should be aiming for? The National Institutes of Health in the US provides completely different figures for vitamin D deficiency. Or, as they choose to call it – ‘inadequacy.’
‘Some people are potentially at risk of inadequacy at 30 to 50 nmol/L (12–20 ng/mL). Levels of 50 nmol/L (20 ng/mL) or more are sufficient for most people. In contrast, the Endocrine Society stated that, for clinical practice, a serum 25(OH)D concentration of more than 75 nmol/L (30 ng/mL) is necessary to maximize the effect of vitamin D on calcium, bone, and muscle metabolism.’
The truth is that, wherever you look the figures are all over the place. Made more complicated by the fact that the US uses different units of measurement to everyone in the civilised world, by which I mean Europe… of course. When they say seventy-five, they really mean thirty. ‘You say nanograms per millimole, I say nanomoles per litre – let’s call the whole thing off.’
So, should you be aiming for 20nmol/l? Or is it thirty or forty, or fifty? If in doubt aiming higher would be my advice, better safe than sorry. After all, it has been found that the majority of people with cancer have ‘low’, if not ‘deficient’ levels of Vitamin D.
‘More than three-fourths of people with a variety of cancers have low levels of vitamin D, and the lowest levels are associated with more advanced cancers, a new study suggests.’4
If having a low level of Vitamin D means you are more likely to get cancer, then I would certainly define this as deficient, not low, and I would certainly want to do something about it.
And it is not just cancer. There are studies linking low vitamin D to many other diseases, such as kidney disease and, more importantly for the sake of this article, diabetes, and cardiovascular disease. As highlighted in this paper: ‘Vitamin D deficiency increases risk of nephropathy and cardiovascular diseases in Type 2 diabetes mellitus patients.’
‘Vitamin D (VD) deficiency is associated with insulin function and secretion. It is linked with diabetes mellitus (DM) progression, and complications were also recorded…The evidence from this study suggest that patients with Type 2 diabetes with vitamin D deficiency are at higher risk for developing CVD and nephropathy [kidney damage].’ 5
Additionally, a low Vitamin D level can be a factor that drives obesity and diabetes in the first place. Here, from the study: ‘Vitamin D deficiency is a risk factor for obesity and diabetes type 2 in women at late reproductive age.’
‘Our results showed that vitamin D insufficiency is highly prevalent in the population of healthy women. Low 25(OH)D [a form of vitamin D] levels correlated with high body fat, glucose levels and decreased insulin sensitivity. We conclude that vitamin D deficiency is a potential risk factor for obesity and development of insulin resistance leading to diabetes type 2. 6
If you choose to look, the evidence for the potential harms of low… deficient… inadequate…insufficient… suboptimal Vitamin D stretch on, and on, and on. Cancer, diabetes, obesity, kidney failure, cardiovascular disease. In the era of COVID19, there are also significant benefits from vitamin D in boosting of the immune system and reducing the risk of infection.7
Cutting to the chase, most doctors are eager to dismiss the benefits of Vitamin D on, pretty much, anything. However, I think the evidence for benefits on overall, and cardiovascular health are overwhelming.
Of equal importance is the fact that vitamin D is incredibly safe to take. It is true that toxicity has been seen in a few people, very few. However, it took sixty thousand units a day for several months to reach this point.
‘Taking 60,000 international units (IU) a day of vitamin D for several months has been shown to cause toxicity.8 ‘
Frankly, taking that dose would be nuts, and would not be required by anyone, ever. Personally, I take nine thousand units a day from October to March. I am l looking to get my levels above 50nmol/l, and keeping them there, if possible.
And why on earth would you not? Vitamin D is remarkably safe, and cheap. In the summer you don’t need to take any at all. You can get all you need by going out in the sun when it shines and, shock, horror, exposing your skin for an hour or so. Even more if you like.
Why do doctors dislike vitamins so much? It is complicated, but primarily driven by the pharmaceutical industry, who absolutely hate the idea of people buying ‘health’ products that they cannot make any money from. So, they make wild claims about vitamins damaging health, and suchlike. They are simply trying to take out the opposition, usual tactics. For example:
‘….a USA TODAY investigation finds that a wide array of dietary supplement companies caught with drug-spiked products are run by people with criminal backgrounds and regulatory run-ins. Consumers buying products from these firms are in some cases entrusting their health and safety to people with rap sheets for crimes involving barbiturates, crack cocaine, Ecstasy and other narcotics, as well as arrests for selling or possessing steroids and human growth hormone. Other supplement company executives have records of fraud, theft, assault, weapons offenses, money laundering or other offenses, the investigation shows.9’
Blah de blah. I amuse myself by reading the title of the book by Peter Gøtzsche: ‘Deadly Medicines and Organised Crime. How big pharma has corrupted healthcare.’ As he says. ‘If you don’t think the system is out of control, please email me and explain why drugs are the third leading cause of death… If such a hugely lethal epidemic had been caused by a new bacterium or a virus, or even one-hundredth of it, we would have done everything we could to get it under control…’
Something reinforced by Richard Smith (previous long-time editor of the British Medical Journal) in the foreword to Gøtzsche’s book:
‘It is scary how many similarities there are between this industry (the pharmaceutical industry) and the mob. The mob makes obscene amounts of money, as does this industry. The side effects of organised crime are killings and death, and the side effects are the same in this industry. The mob bribes politicians and others, and so does the drug industry.’
Just in case you think Gøtzsche and Smith are over-reacting, here is what Harvard University states:
‘Few know that systematic reviews of hospital charts found that even properly prescribed drugs (aside from misprescribing, overdosing, or self-prescribing) cause about 1.9 million hospitalizations a year. Another 840,000 hospitalized patients are given drugs that cause serious adverse reactions for a total of 2.74 million serious adverse drug reactions. About 128,000 people die from drugs prescribed to them. This makes prescription drugs a major health risk, ranking 4th with stroke as a leading cause of death. The European Commission estimates that adverse reactions from prescription drugs cause 200,000 deaths; so together, about 328,000 patients in the U.S. and Europe die from prescription drugs each year. The FDA does not acknowledge these facts and instead gathers a small fraction of the cases.10’
Ouch. And there are those who think I am highly critical of the pharmaceutical industry. I’m a pussy cat in comparison. How many deaths have there been from vitamins? Last time I looked; it was one, over a ten-year period. I think a large crate of vitamin D fell off a lorry and squashed someone… (joke).
Anyway, yes, as you may have noticed, I have not yet talked about C… Vitamin C. I have just been setting the scene. Rearranging the mental furniture. So, now to vitamin C. How much do you need? What good does it do?
I find it somewhat strange that almost all animals can synthesize their own Vitamin C, but we cannot. Along with a few great apes, a couple of fruit bats and guinea pigs. Animals synthesize it from glucose, in four steps.
Humans have retained the first three steps but lack the fourth. We lost this fourth step about forty million years ago. Perhaps because we learned to re-cycle vitamin C within our red blood cells, so we need far less of it. The ‘electron transfer hypothesis.’ If making Vitamin C uses up resources that we need for other things… why bother. Just eat it, there is plenty about11.
Anyway, for whatever the exact reason, we lost the ability to make vitamin C. So, we now have to eat it. Mostly from fruit and plants. Tricky if you are Inuit. However, animal meat does contain enough vitamin C to keep the Inuit going.
There is a hypothesis that the Inuit ensure that they eat the adrenal glands of various animals they kill, because this is where there is the highest concentration of vitamin C lies. I don’t think I have seen this proven. Anyway, how could the Inuit possibly have known where vitamin C was concentrated? A clever trick indeed. Do they have secret biochemical labs hidden within glaciers?
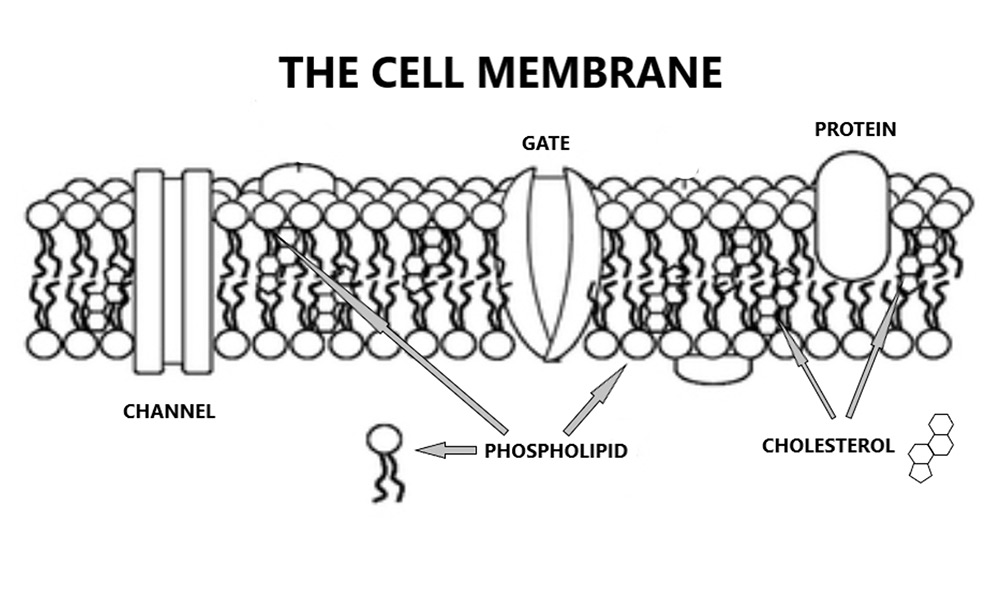
Moving on. What happens if you do not eat enough vitamin C? Well, a whole lot of different things. But the most serious problem is that vitamin C is required to create collagen. Think of collagen as being like the steel bars in concrete, providing support and strength for tissues around the body. Without collagen, things can start to break apart quite dramatically.
Blood vessels, for example, need a lot of collagen, as they have to withstand a lot of pressure, and squeezing and bending and suchlike. So, one of the first clinical signs of scurvy (Vitamin C deficiency) is often bleeding gums. Followed by bleeding everything else. Followed by bleeding to death. Not recommended.
What is both pertinent, and fascinating at this point in the vitamin C story, is that evolution came up with a plug to reduce the risk of bleeding to death in vitamin C deficiency. Until enough vitamin C could be found and consumed again, and collagen synthesis got back to normal.
This plug is called Lipoprotein(a). Or Lp(a).
If blood vessels start to crack, this action attracts a Lp(a) to the scene. It then flings itself at the cracks, to form a plug that is highly resistant to being broken apart. More so, than any other part of a blood clot. It achieves this resistance by using a very clever trick, which is that it blocks the activation of the enzyme specifically designed to break down blood clots.
At this point I need to explain a bit more about blood clots… So, off we go once more, on a detour.
The enzyme designed to break clots apart is plasmin, which does the job of slicing apart strands of fibrin. Fibrin is the very tough strand of protein that wraps around all blood clots, then binds them together, then tightens up the entire clot up and makes it very tough and difficult to ‘lyse’ i.e. slice apart.
Fibrin is constructed when smaller pieces of protein, called fibrinogen are linked up, end to end, to form the much longer fibrin strand. This is the final step of the monstrously complex ‘clotting cascade’. [You could not allow long strands of fibrin to float about freely in the blood. They would just end getting tangled around everything else and getting stuck in various vital places.]
So, whilst fibrin has a critical function in blood clot formation, if you cannot break it down – once the bleeding has stopped, and repair has started – then you cannot break apart the blood clot either – at least not easily. And if you cannot break apart blood clots, then they are going to hang around – almost forever. Which is not a good thing, as you can probably imagine.
Which is where the enzyme known as plasmin comes in. Once bleeding has stopped, plasmin is ‘activated’ to slice – or lyse – the clot apart, and then it is gone.
How do you activate plasmin? Well, this process starts with another protein called plasminogen – which is incorporated into all blood clots as they form. Plasminogen then sits there doing nothing much. However, you can convert plasminogen into plasmin using another enzyme called tissue plasminogen activator (TPa).
TPa + plasminogen → plasmin → fibrin sliced apart ‘lysed’
Yes, step after step… after step. Tissue plasminogen activator is now made commercially and is colloquially known as a ‘clotbuster’. It is often given to people having a stroke to ‘bust’ the clot apart. [Unless you are having a stroke due to a bleed, not a clot, at which point given TPa would not be a great idea].
So, and keep holding on here, because I am going to get back to Vitamin C in a bit… so, what if you could not break up clots? At least, not so easily. Well, whilst this is a good thing if your blood vessels are cracking due to a lack of collagen, as the blood clot ‘plugs’ will need to last for a long time. At least until Vitamin C intake goes up, and collagen can be made.
However, if you do not have scurvy, having blood clots that resist lysis is a bad thing, because these clots are more likely going to hang around for ages. They will be stuck to blood vessel walls for quite a long time. Which means that they can become the focus for atherosclerotic plaques. [At least this is what happen if you believe in the thrombogenic hypothesis – which I do].
Now, getting back to Lp(a). How does it stop clots being broken down? Well, the(a) in Lp(a) stands for apolipoprotein(a). This protein is almost identical to plasminogen – the protein that is incorporated into all blood clots as they form. However, apolipoprotein(a) cannot be converted to plasmin by tissue plasminogen activator. Instead, it acts as a tissue plasminogen activator inhibitor. It jams up the active site of TPa.
So, deep breath. If you have a lot of Lp(a) around, you are in danger of creating difficult to shift blood clots. As outlined in the paper ‘Lipoprotein(a) as a modifier of fibrin clot permeability and susceptibility to lysis.’
‘We here provide the first evidence that elevated plasma Lp(a) levels correlate with decreased fibrin clot permeation and impaired susceptibility to fibrinolysis both in apparently healthy subjects and patients with advanced coronary artery disease. The relationship between Lp(a) and clots …are associated with extremely unfavourable clot properties12.’
Therefore, if you have a lot of Lp(a) in you blood, you will have blood clots with ‘extremely unfavourable clot properties.’ And so, you may end up dying of cardiovascular disease. Here is an article from the New York Times:
‘To millions of Americans, Bob Harper was the picture of health, a celebrity fitness trainer who whipped people into shape each week on the hit TV show “The Biggest Loser.”
But last February, Mr. Harper, 52, suffered a massive heart attack at a New York City gym and went into cardiac arrest. He was saved by a bystander who administered CPR and a team of paramedics who rushed him to a hospital, where he spent two days in a coma.
When he awoke, Mr. Harper was baffled, as were his doctors. His annual medical checkups had indicated he was in excellent health. How could this have happened to someone seemingly so healthy?
The culprit, it turned out, was a fatty particle in the blood called lipoprotein(a). While doctors routinely test for other lipoproteins like HDL and LDL cholesterol, few test for lipoprotein(a), also known as lp(a), high levels of which triple the risk of having a heart attack or stroke at an early age.’
You may think, why have I never heard of Lp(a). Fear not, you are not alone, as most doctors have never heard of it either. The surprising fact is that, although you may think you have never heard of Lp(a) you have. Because it is actually….
Drum roll, great suspense…
It is…. Low Density Lipoprotein (LDL). Yes, it is ‘bad cholesterol’ itself. The evil substance of doom itself. What a remarkable coincidence…
You think I am pulling your leg. I am, but only slightly. In fact, to be fully accurate, Lp(a) is actually low-density lipoprotein (LDL), with an extra strand of protein attached to it. And that protein is apolipoprotein(a).
Yes, apolipoprotein(a), the very protein that pretends to be plasminogen. The protein that inhibits blood clots from being broken apart. This is all a bit like a Sherlock Holmes story. Ladies and Gentlemen, I give you…
‘The tragic case of mistaken identity.’
‘I put it to you sir, that when you looked at atherosclerotic plaques and saw LDL within them, you were actually looking at Lp(a) molecules, but you did not recognise them. Because you miserably failed to look for the apolipoprotein(a).’
Or, to switch metaphors in a heavy-handed manner to Cluedo.
‘It was Lp(a) wot done it, in the left anterior descending artery, with an apolipoprotein(a) molecule.’
Or, to put it more technical speak, from the paper ‘Quantification of apo[a] and apoB in human atherosclerotic lesions.’:
‘These results suggest that Lp[a] accumulates preferentially to LDL in plaques, and that plaque apo[a] is directly associated with plasma apo[a] levels and is in a form that is less easily removable than most of the apo B. This preferential accumulation of apo[a] as a tightly bound fraction in lesions, could be responsible for the independent association of Lp[a] with cardiovascular disease in humans13.’
Oh, my goodness, it is all so very complicated, is it not? Well, it is both complicated, and fascinating. You start looking at Vitamin C, and you end up comparing the molecular structure of plasminogen and apolipoprotein(a). Then you find that Lp(a) is, to all intents and purposes, LDL.
Now, let me see. Where does vitamin C properly fit into this tale?
Well, if you don’t have enough vitamin C, then you are more likely to end up with cracks in your blood vessels. These cracks will then be plugged by small blood clots, containing a lot of Lp(a). If you have a high Lp(a) level, then these small blood clots will be even bigger, and even more difficult to remove.
Which means that if you have a high Lp(a) level, it would be a splendid idea to ensure that you never become vitamin C deficient. Indeed, even if you do not have a high Lp(a) level it would be a splendid idea to ensure that you do not become vitamin C deficient. Because cracks in blood vessel walls are never a good thing. Ending up, potentially, as the focus for atherosclerotic plaques.
Linus Pauling, a famous double Nobel Prize winner, believed that ‘sub-clinical’ Vitamin C deficiency was ‘the’ cause of cardiovascular disease. He also believed that if everyone took enough vitamin C, cardiovascular disease would disappear.
Personally, I do not think it is ‘the’ cause of cardiovascular disease, but I do think that it is ‘a’ cause. That is, whether or not you have a high Lp(a) level. Of course, a high Lp(a) level is likely to make things far worse, were you to end up vitamin C deficient.
However, the vitamin C, cardiovascular disease story does not end here. Because vitamin C has many other critical functions that link back to cardiovascular disease in one way, or another. For example, it has a more general function in protecting endothelial cells from harm, and supports the integrity of the vascular system. Here, from the paper ‘Role of Vitamin C in the function of the vascular endothelium’:
‘Vitamin C, or ascorbic acid, has long been known to participate in several important functions in the vascular bed in support of endothelial cells. These functions include increasing the synthesis and deposition of type IV collagen in the basement membrane, stimulating endothelial proliferation, inhibiting apoptosis (endothelial cell death), scavenging radical species, and sparing endothelial cell-derived nitric oxide to help modulate blood flow. Although ascorbate may not be able to reverse inflammatory vascular diseases such as atherosclerosis, it may well play a role in preventing the endothelial dysfunction that is the earliest sign of many such diseases.’
Supplementation to upper normal plasma ascorbate levels is clearly indicated in most diseases and conditions in which ascorbate is depleted. However, it is seldom a priority, because patients, physicians, and health authorities are unaware of the increasing evidence for multiple potentially important functions of ascorbate. With regard to the endothelium, it is worth emphasizing observations made more than 50 years ago that early scurvy generates endothelial disruption in guinea pigs, which resembles atherosclerosis and is fully and rapidly reversible with ascorbate repletion.14’
Yes, with regard to the last part about guinea pigs. Many years ago, a researcher deliberately made guinea pigs ‘scorbutic’ – the medical term for the state of vitamin C deficiency, a.k.a. scurvy. At which point they developed atherosclerotic plaques.
When the vitamin C was added back into their diet, the atherosclerotic plaque disappeared. [Unless you left it too long, in which case, the plaques remained]. Best animal experiment on atherosclerosis ever done – never repeated.
Having just said all of this. I do not believe that most of us, most of the time, are lacking vitamin C – to any degree. At least I do not think so. However, if we become infected – with almost anything – the requirement for vitamin C shoots up. Because Vitamin C gets burned up protecting the endothelium, and it also supports the immune system
‘The role of vitamin C in lymphocytes is less clear, but it has been shown to enhance differentiation and proliferation of B- and T-cells, likely due to its gene regulating effects. Vitamin C deficiency results in impaired immunity and higher susceptibility to infections. In turn, infections significantly impact on vitamin C levels due to enhanced inflammation and metabolic requirements.15’
Another key thing to know about vitamin C, again closely related, is that people with type II diabetes, and people who smoke, have reduced circulating levels of Vitamin C.
‘Although T2DM [type II diabetes mellitus] is not traditionally considered a risk factor for vitamin C deficiency, our research indicates that those with prediabetes or T2DM are more likely to have inadequate or deficient plasma vitamin C concentrations. This did not appear to be due to a lower dietary vitamin C intake, so dietary advice needs to emphasise the importance of consuming high vitamin C foods.16’
What links smoking, type II diabetes, and vitamin C? Here I am hypothesizing a little. What links them is that with smoking, and type II diabetes, the endothelium is under ‘attack’. High blood sugar levels damage the glycocalyx (the protective lining of endothelium), and so do the nanoparticles that enter the bloodstream if you smoke.
Here is a quote from the paper: ‘Loss of endothelial glycocalyx during acute hyperglycemia coincides with endothelial dysfunction and coagulation activation in vivo.’ (In vivo means in a real live person, not just in vitro – in a test tube). Jargon alert:
‘Hyperglycemia is associated with increased susceptibility to atherothrombotic stimuli. The glycocalyx, a layer of proteoglycans covering the endothelium, is involved in the protective capacity of the vessel wall. We therefore evaluated whether hyperglycemia affects the glycocalyx, thereby increasing vascular vulnerability…
In the present study, we showed that the glycocalyx constitutes a large intravascular compartment in healthy volunteers that can be estimated in a reproducible fashion in vivo. More importantly, we showed that hyperglycemic clamping elicits a profound reduction in glycocalyx volume that coincides with increased circulating plasma levels of glycocalyx constituents like hyaluronan, an observation that is consistent with the release of glycocalyx constituents into the circulation17.’
Looking specifically at smoking:
‘Vascular dysfunction induced by smoking is initiated by reduced nitric oxide (NO) bioavailability and further by the increased expression of adhesion molecules and subsequent endothelial dysfunction. Smoking-induced increased adherence of platelets and macrophages provokes the development of a procoagulant and inflammatory environment.18’
Essentially, smoking and high blood glucose both damage the endothelium, which results in low vitamin C levels, as the endothelial cells burn through Vitamin C to maintain themselves. Ergo, fi you have type II diabetes, or smoke, you need more Vitamin C to maintain healthy levels….
Now, before I introduce you to far too many new and difference concepts – I did mention everything starts linking back together in completely unexpected ways – it is time to draw our little tale of Vitamin C together.
The first thing to say about vitamin C is that it is vital. I have only covered a few of the essential functions that it has in the human body. Those most closely related to cardiovascular disease. Importantly, it is almost impossible to cause harm by overconsumption. It is just about as safe to take, as anything can possibly be.
The next thing to say is that most of us, most of the time, probably have sufficient vitamin C intake, and require no supplements.
However, if you have a high Lp(a) level, then any damage caused by a lack of vitamin C will be amplified, dure the fact that Lp(a) sticks very tightly to areas of endothelial damage, making the resultant blood clot very difficult to remove. So, for those with high Lp(a) levels, I would recommend one gram of vitamin C a day – forever.
If you smoke, or have diabetes, the lining of your artery walls (glycocalyx and endothelium) are under constant attack from nasty substances – smoke nanoparticles and high blood glucose. This, too, will create ‘cracks’ in blood vessels.
In both situations Vitamin C is also used up more rapidly, trying to protect against this damage. So your vitamin C level is likely to be low. Which means that you too, should take one gram of vitamin C a day – forever. [Or you could try stopping smoking]
In addition, in many infections, the endothelium is under severe attack. Either directly from the microorganisms entering and killing endothelial cells (see under COVID19), or from the exotoxins (toxic waste products) released by any bacteria in the bloodstream.
The most severe endothelial attack occurs in sepsis (infection of the blood), where the exotoxins strip away the endothelium, resulting in widespread blood clotting (disseminated intravascular coagulation DIC). Which is the thing that, primarily, kills you with sepsis.
Whilst sepsis represents an extreme situation, it is still the case that if you are suffering from an infection, of any sort (gingivitis or periodontal disease) your requirement for vitamin C will shoot up. Which means that you should take as much Vitamin C as you can tolerate. Up to ten grams a day. I cannot take this amount due to the impact it has on my gastrointestinal tract. Loose, is the word. Very loose. Looser than loose.
But if you can tolerate it, Vitamin C will help to protect your endothelium. It will also boost the functioning of your immune system.
So, there we are then, vitamin C. My second favourite vitamin, after vitamin D. In the winter I take a gram a day. Along with my nine thousand units of vitamin D. Almost all medics will instantly dismiss this as ‘woo woo’ nonsense. I would tend to argue that this is because they know absolutely nothing about vitamins, or their critical roles in human physiology, and have never bothered to find out.
Pop quiz for your doctor, next time you see them. Ask them how a lack of vitamin C causes scurvy. What is the primary disease process? Watch them scrabble to bring up a Google search. Then ask them about Lp(a). What it is, what it does… I guarantee that silence will be the stern reply.
1: https://advances.augusta.edu/1014#:~:text=Interestingly%2C%20in%20Japan%20the%20reference,methylmalonate%20levels%20are%20not%20checked.
2: https://onlinelibrary.wiley.com/doi/full/10.1111/bjh.12959
3: https://www.nhs.uk/news/food-and-diet/the-new-guidelines-on-vitamin-d-what-you-need-to-know/
4: https://www.webmd.com/cancer/news/20111004/low-vitamin-d-levels-linked-to-advanced-cancers#1
5: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6540771/
6: https://pubmed.ncbi.nlm.nih.gov/23924693/
7: https://vitamindforall.org/letter.html
8: https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/expert-answers/vitamin-d-toxicity/faq-20058108#:~:text=Advertisement&text=The%20main%20consequence%20of%20vitamin,the%20formation%20of%20calcium%20stones.
9: https://eu.usatoday.com/story/news/nation/2013/12/19/dietary-supplements-executives-criminal-records-spiked/4114451/
10: https://ethics.harvard.edu/blog/new-prescription-drugs-major-health-risk-few-offsetting-advantages
11: https://academic.oup.com/emph/article/2019/1/221/5556105
12: https://onlinelibrary.wiley.com/doi/full/10.1111/j.1538-7836.2006.01903.x
13: http://www.jlr.org/content/32/2/317.full.pdf
14: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3869438/
15: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5707683/
16: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5622757/
17: https://diabetes.diabetesjournals.org/content/55/2/480
18: https://www.ncbi.nlm.nih.gov/pubmed/24554606