[Yes, this one took a long time to write]
When I started looking at heart disease, or cardiovascular disease (CVD) it was initially because I was interested to know why the Scots and the French had such different death rates. I had also just finished a book by James le Fanu called ‘Eat your heart out’ in which he made it very clear, or at least he did to me, that fat/saturated fat in the diet had nothing to do with CVD in any way shape of form.
However, at the time le Fanu was very much a voice crying in the wilderness. The experts had a very different song, or dirge. Namely that the Scots diet was terribly unhealthy, and this fully explained why they kept keeling over from heart attacks. Their bad diet raised cholesterol levels and…. thud (sound of Scots person falling over dead).
This is still very much the case. All of our medical authorities still announce the absolute truth of the ‘terrible Scottish diet’ with adamantine confidence. They usually bring out the almost mythical ‘deep fried mars bar’ as the perfect example as to why the Scots die of heart attacks, and strokes, and suchlike. ‘Well, what can you expect of a nation that eats deep fried mars bars… ho, ho.’
The truth is that hardly any Scotsman, or women, has ever eaten such a thing. And if they did it once, they will most certainly never do it again (I was certainly put off for life after one drunken foray on a Saturday night). Of course, there is also a perfect irony here. A mars bar is almost entirely made up sugar (not fat). When you fry it, it will be in vegetable/polyunsaturated fat – as saturated fats have been virtually banned in deep fat fryers. So, in theory, a deep fried mars bar should be somewhat more heart healthy than a ‘virgin’ mars bar. As it now contains a mass of hot sugar plus some heart ‘healthy’ polyunsaturated fat.
I suppose this example, at least to me, highlights the complete lack of any consistent logic or thought in the diet heart world. A fact that I became very painfully aware of, over many years. Indeed, I came to realise that there is no area of human existence where more nonsense is spouted than the ever-changing beliefs about what constitutes a healthy, or unhealthy diet. Frankly, it is almost entirely wall to wall rubbish.
At one point I made an effort to look at the classical ‘risk factors’ for heart disease between France and Scotland. This was done some years ago as part of a paper I wrote called ‘Does Insulin Resistance cause atherosclerosis in the post-prandial period?’ Something which I still think is at least part of the picture of CVD.
Here is the table I put together from a number of different sources – there was no single source for the data I was looking for. [I could not find separate UK and Scottish figures for a number of the factors, so I had to look at the UK as a whole. In addition, at there were no clear cut data on saturated fat, so I used animal fat as a proxy – which is almost the same thing]
| Risk factors and death rates from CHD in the UK and France per 100,000/year (men 55 – 64) | ||
| France | UK | |
| Animal fat % total energy intake | 25.7% | 27% |
| Fruit/veg % total energy intake | 5.0% | 4.3% |
| Percentage smoking | 32% | 29% |
| Total cholesterol level | 6.1mmol/l | 6.2mmol/l |
| HDL level | 1.3mmol/l | 1.3mmol/l |
| Systolic BP | 150 | 148 |
| Prevalence type II diabetes | ~2% | 2% |
| Percentage who never exercise | 32% | 24% |
| Mean BMI | 26.6 | 26.6 |
| Death rate from IHD (IHD 410-4) | 128 | 487 |
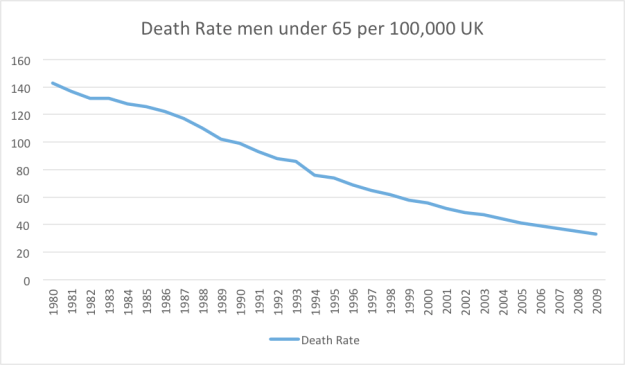
As you can see, there was virtually no difference in the classical risk factors for UK men and French men. Despite this, the French had one quarter the risk of death from ischaemic heart disease [what you or I would tend to call heart disease]. Since that time the French rate of heart disease has continued to fall, as it has also done in the UK, whilst the French consumption of saturated fat has risen. Interestingly total cholesterol levels have fallen in both countries.
So, whatever was going on had very little to do with diet. And if it had very little to do with diet, then it also had little to do with cholesterol either. If your hypothesis is that eating saturated fat increases cholesterol, or LDL cholesterol levels, which then causes CVD then how can two countries with exactly the same saturated fat consumption and cholesterol level (and all other risk factors equal) have such a different rate of CVD? And how could France, whilst continuing to eat more saturate fat, have a falling cholesterol levels? And how does the Ukraine, which currently has the lowest saturated fat intake in Europe, end up with the highest rate of CVD etc. etc. etc.
When you start looking at facts like this you must start to question the diet-heart cholesterol hypothesis. Or at least I thought you must. How wrong I was. Virtually the entire medical profession was wedded to the diet-heart cholesterol hypothesis – still is. Facts appear to have no impact whatsoever on this belief system.
Anyway, once I started to look at CVD in more detail, I was confronted with a choice. Accept that I must be wrong. After all, how can all the researchers and experts and Nobel prize winners be wrong. They must surely be seeing things that I cannot. Or, accept that the diet-heart cholesterol hypothesis was wrong. The blue pill, or the red pill.
Dear reader, I chose the red pill, in the sure and certain knowledge that rejecting the conventional thinking was certainly not going to be an easy path to follow. I also knew that if I was going to reject the diet-heart/cholesterol hypothesis, then I had to try and find out what does actually cause CVD. When I looked around at first there, were few alternative voices, or hypotheses out there. If truth be told, there seemed to be none (at least initially). But if not cholesterol, then what?
Over time, as I looked around, some ghosts in the machine began to emerge. I was aware of a doctor (whose name I cannot even remember) who firmly believe that fibrinogen was the main cause of CVD, and I went to a talk that he gave on the subject – not paying it much heed in truth. Then the Scottish Heart Health Study was published, and the single most powerful risk factor that emerged for CVD risk was… fibrinogen. A blood clotting factor. Aha. Could CVD actually be due to blood clotting abnormalities?
This was a time before the internet, before search engines, before finding information was so easy. This was an era when you had to traipse down to the medical library and pull actual books from actual shelves if you wanted to find out stuff. After pulling a lot of books off a lot of shelves I learned of Duguid, a Scottish doctor, who argued that blood clotting was the cause of CVD (I paraphrase).
His work was published shortly after the second world war, and has remained mostly unread. Then I went all the way back to Karl von Rokitansky who, in 1852, felt that atherosclerotic plaques were, in fact, just blood clots – in various stages of repair. An observation which, from time to time, other researchers have noted. Most particularly a doctor called Smith, from Aberdeen. He is no longer active in this area of research.
Here is the abstract from his paper ‘Fibrinogen, fibrin and fibrin degradation products in relation to atherosclerosis’. I have quote the abstract in full, for those who like to see a bit more detail. Others may glaze over, or skip to the last sentence:
‘Many human atherosclerotic lesions, showing no evidence of fissure or ulceration, contain a large amount of fibrin which may be in the form of mural thrombus on the intact surface of the plaque, in layers within the fibrous cap, in the lipid-rich centre, or diffusely distributed throughout the plaque. Small mural thrombi are invaded by SMCs (smooth muscle cells) and collagen is deposited in patterns closely resembling the early proliferative gelatinous lesions. In experimental animals, thrombi are converted into lesions with all the characteristics of fibrous plaques, and in saphenous-vein bypass grafts, fibrin deposition is the main cause of wall thickening and occlusion. There seems little doubt that fibrin deposition can both initiate atherogenesis and contribute to the growth of plaques.
Epidemiological studies indicate that increased levels of fibrinogen and clotting activity are associated with accelerated atherosclerosis, and although blood fibrinolytic activity has given inconsistent results, in arterial intima both fibrinolytic activity and plasminogen concentration are decreased in cardiovascular disease. Fibrin may stimulate cell proliferation by providing a scaffold along which cells migrate, and by binding fibronectin, which stimulates cell migration and adhesion. Fibrin degradation products, which are present in the intima, may stimulate mitogenesis and collagen synthesis, attract leukocytes, and alter endothelial permeability and vascular tone.
In the advanced plaque fibrin may be involved in the tight binding of LDL and accumulation of lipid. Thus there is extensive evidence that enhanced blood coagulation is a risk factor not only for thrombotic occlusion, but also for atherogenesis. Enhanced blood coagulation frequently coexists with hyperlipidaemia and, together, these may have a synergistic effect on atherogenesis.’ 1
For those whose eyes did glaze over, concentrate only on the last sentence. ‘Enhanced blood coagulation frequently coexists with hyperlipidaemia and, together, these may have a synergistic effect on atherogenesis.’
Here, ladies and gentlemen, lies my little secret. My evil twin brother who I have kept in the attic for the last twenty years, gnawing at the floorboards. The terrible truth that there is an association between LDL levels/familial hypercholesterolemia and CVD. Something which I appear to have argued against for many, many, years.
Does this mean that the experts have been right, all along? High LDL cholesterol levels do cause CVD? Well maybe, maybe not. At this point I need to take you back to the statement again. ‘Enhanced blood coagulation frequently coexists with hyperlipidaemia.’
Does this mean that hyperlipidaemia actually causes enhanced blood coagulation? Or does it mean that something else causes both. Here is the old ‘yellow fingers and lung cancer’ discussion.
‘People with yellow fingers are more likely to die of lung cancer.’
Why… because people with yellow fingers smoke, and smoking causes lung cancer. Ergo yellow fingers are simply a sign of smoking, they do not actually cause lung cancer.
‘People with raised LDL are more likely to die from CVD’
Why… because people with raised LDL are also more likely to have enhanced blood coagulation. Ergo, raised LDL levels are only associated with enhanced blood coagulation, they do not actually cause CVD. It is the blood coagulation factors.
Alternatively, raised LDL may actually enhance blood coagulation, all by itself.
Where does the answer lie? In truth the answer has been very difficult to tease out. Even now, after many years, I do not feel that I can fully disentangle the data. Here for example, is a paper called ‘Maternal familial hypercholesterolaemia (FH) confers altered haemostatic profile in offspring with and without FH.’
‘Children with (n=9) and without (n=7) FH born of mothers with FH, as well as control children (n=16) born of non-FH mothers were included in the study. The concentrations of tissue plasminogen activator, plasminogen activator inhibitor (PAI-1), tissue factor (TF), TF pathway inhibitor (TFPI), thrombomodulin, fibrinogen, prothrombin fragment 1+2 and von Willebrand Factor were measured. Our findings show i) higher levels of PAI-1 and TFPI in children with and without FH born of mothers with FH compared with control children, ii) lower levels of thrombomodulin in children with FH compared with control children, and iii) significant correlations between maternal PAI-1 levels during pregnancy and PAI-1 levels in the offspring.’2
What this tells us is that, if a mother has Familial Hypercholesterolaemia, she passes on abnormalities of blood coagulation to her children. Both those that have, and those that do not have FH. [Not all children of mothers with FH will end up with the FH gene]. Some of this may be epigenetically modulated. In short, it is not the LDL that is important, it is simply the mother’s genes….
Or is it? Here is a paper suggesting that the LDL itself, independently of anything else, makes platelets more likely to stick together (a key step in blood clotting).
‘The interaction of platelets with lipoproteins has been under intense investigation. Particularly the initiation of platelet signaling pathways by low density lipoprotein (LDL) has been studied thoroughly, since platelets of hypercholesterolemic patients, whose plasma contains elevated LDL levels due to absent or defective LDL receptors, show hyperaggregability in vitro and enhanced activity in vivo. These observations suggest that LDL enhances platelet responsiveness….’ 3
However, maybe these researches misinterpreted what they were seeing. For example, another paper found that the level of LDL in those with FH was not related to their risk CVD. It was purely the level of clotting factors that was related to CVD. This paper entitled: ‘Coronary artery disease and haemostatic variables in heterozygous familial hypercholesterolaemia.’
‘Haemostatic variables were measured in 61 patients with heterozygous familial hypercholesterolaemia, 32 of whom had evidence of coronary heart disease. Age adjusted mean concentrations of plasma fibrinogen and factor VIII were significantly higher in these patients than in the 29 patients without coronary heart disease, but there were no significant differences in serum lipid concentrations between the two groups. Comparisons in 30 patients taking and not taking lipid lowering drugs showed lower values for low density lipoprotein cholesterol, high density lipoprotein cholesterol and antithrombin III, and a higher high density lipoprotein ratio while receiving treatment. The results suggest that hypercoagulability may play a role in the pathogenesis of coronary heart disease in patients with familial hypercholesterolaemia.’4
So it is not the high LDL? It is the raised blood clotting factors that are found in some, but not all of those with FH. As you can see, it is not straightforward at all.
Just to complicate the picture further, here is a paper strongly suggesting that HDL is directly anti-coagulant.
‘Native HDL prevents platelet hyperreactivity by limiting intraplatelet cholesterol overload, as well as by modulating platelet signalling pathways after binding platelet HDL receptors such as scavenger receptor class B type I (SR-BI) and apoER2′. The antithrombotic properties of native HDL are also related to the suppression of the coagulation cascade and stimulation of clot fibrinolysis. Furthermore, HDL stimulates the endothelial production of nitric oxide and prostacyclin, which are potent inhibitors of platelet activation. Thus, HDL’s antithrombotic actions are multiple and therefore, raising HDL may be an important therapeutic strategy to reduce the risk of arterial and venous thrombosis.’ 5
And what about VLDL?
‘There is a considerable body of evidence supporting an association between hypertriglyceridaemia (high level of VLDL), a hypercoagulable state and atherothrombosis. A disorder of triglyceride metabolism is a key feature of the metabolic syndrome that increases risk of both ischaemic heart disease and type 2 diabetes approximately 3-fold. An increasing prevalence of obesity and metabolic syndrome is likely to contribute markedly to the prevalent ischaemic heart in the foreseeable future, and therefore it is crucial to understand mechanisms linking hypertriglyceridaemia and a hypercoagulable state. Activation of platelets and the coagulation cascade are intertwined. VLDL and remnant lipoprotein concentrations are often increased with the metabolic syndrome. These lipoproteins have the capacity to activate platelets and the coagulation pathway, and to support the assembly of the prothrombinase complex. VLDL also upregulates expression of the plasminogen activator inhibitor-1 gene and plasminogen activator inhibitor-1 antigen…’ 6 etc.
You can go back and forward in this area, finding research that contradicts itself upside down and inside out again. What I think I know for certain is the following:
- High LDL levels/familial hypercholesterolemia is closely associated with increased blood coagulation (in a high percentage of those with FH, though not all) – through many different interrelated mechanisms. Some genetic, some possibly directly due to LDL itself.
- VLDL (triglyceride) seems to increase blood coagulation – and this seems a very consistent finding
- HDL has anticoagulant effects
I don’t know how powerful these different pro and anti-coagulant effects are, but they certainly exist. To an extent I could just say what does it matter if LDL does, or does not increase blood coagulation directly – but is simply associated with blood clotting abnormalities. It all fits within the processes that I have outlined in this series of blogs. Namely, anything that increases the risk of blood clotting increases the risk of CVD. And LDL (directly, or through genetic association) does increase the risk.
However, I thought it would be dishonest of me not to highlight the fact that there could well be a causal association between LDL (and VLDL) and CVD. Also there does seem to be a causal protective mechanism provided by HDL.
Or, to put this another way, perhaps all the experts were (a bit) right all along. Even if they have consistently promoted a process that does not make any sense at all i.e. LDL leaks into artery walls causing inflammation and plaque growth etc.
A further proviso is that I cannot see that the LDL/VLDL/HDL effects are very strong. After all I just co-authored a paper showing that higher LDL levels in the elderly are associated with increased life expectancy and a slight reduction in CVD risk. [There are many other factors clouding the issue here – too many to discuss in one go]. Confused yet… welcome to my world.
So where did I get to. I think I got to the point where I accept that:
- LDL is pro-coagulant and – at very high levels e.g. in FH – increases the risk of CVD [though it is difficult to disentangle this from intertwined genetic pro-coagulant factors]
- VLDL is pro-coagulant, and increases the risk of CVD
- HDL is anticoagulant and protects against CVD
Which then brings onto statins, and how they work. First to re-iterate that statins do reduce the risk of CVD [Something, I have never disputed]. However, they do it not by lowering LDL, but because they have anticoagulant effects. Not that potent, about the same as aspirin, but the effect does exist.
Here from a paper entitled ‘statins and blood coagulation’:
‘The 3-hydroxy-3-methylglutaryl (HMG)-coenzyme A (CoA) reductase inhibitors (statins) have been shown to exhibit several vascular protective effects, including antithrombotic properties, that are not related to changes in lipid profile. There is growing evidence that treatment with statins can lead to a significant downregulation of the blood coagulation cascade, most probably as a result of decreased tissue factor expression, which leads to reduced thrombin generation…. Treatment with statins can lead to a significant downregulation of the blood coagulation cascade….’ 7 An effect confirmed by their protection against DVT.
‘Venous thromboembolism (VTE) includes both deep vein thrombosis (DVT) and pulmonary embolism. The 2009 JUPITER trial showed a significant decrease in DVT in non-hyperlipidemic patients, with elevated C-reactive protein (CRP) levels, treated with rosuvastatin.’ 8 Yet, the experts continue to tell us that statins work, purely, by lowering LDL levels. Ho hum.
Whilst I could have written this series and simply pushed LDL, VLDL and HDL to one side. I thought I needed to bring them into the discussion. Not to dismiss them but, I hope, to explain what their role within CVD may actually be – pro and anti-coagulant agents. Here is where they fit, and make sense. Looking at lipoproteins in the light also helps to explain how statins actually work.
References:
1: http://www.ncbi.nlm.nih.gov/pubmed/3524931
2: http://europepmc.org/abstract/med/23199546
3: http://www.ncbi.nlm.nih.gov/pubmed/16877876
4: Br Heart j 1985; 53: 265-8
5: http://www.ncbi.nlm.nih.gov/pubmed/24891399
6: https://www.karger.com/Article/Pdf/93221
7: http://www.ncbi.nlm.nih.gov/pubmed/15569822
8: http://www.ncbi.nlm.nih.gov/pubmed/22278047